Codeine Sulfate
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use CODEINE SULFATE ORAL SOLUTION safely and effectively. See full prescribing information for CODEINE SULFATE ORAL SOLUTION. CODEINE SULFATE ORAL SOLUTION CIIInitial U.S. Approval: 1950INDICATIONS AND USAGECodeine sulfate is an opioid analgesic indicated for the management of mild to moderately severe pain where the use of an opioid analgesic is appropriate. (1)DOSAGE AND ADMINISTRATIONUsual adult dosage: 15 to 60 mg (2.5 mL to 10 mL) up to every 4 hours as needed. (2.2)Doses above 60 mg may fail to give commensurate pain relief, and may be associated with an increased incidence of undesirable side effects. (2.2)DOSAGE FORMS AND STRENGTHSOral Solution: Each 5 mL contains 30 mg of codeine sulfate. (3)CONTRAINDICATIONS Hypersensitivity to codeine or any component of the product (4) Respiratory depression in the absence of resuscitative equipment (4) Acute or severe bronchial asthma or hypercarbia (4) Paralytic Ileus (4) WARNINGS AND PRECAUTIONS Respiratory depression: Increased risk in elderly, debilitated patients, those suffering from conditions accompanied by hypoxia, hypercapnia, or upper airway obstruction. (5.1) Controlled substance: Codeine sulfate is a Schedule II controlled substance with an abuse liability similar to other opioids. (5.2) Risk of abuse: Assess patients for their risks for opioid abuse or addiction prior to prescribing codeine sulfate oral solution (5.2) CNS effects: Additive CNS depressive effects when used in conjunction with alcohol, other opioids, or illicit drugs. (5.3) Elevation of intracranial pressure: May be markedly exaggerated in the presence of head injury, other intracranial lesions. (5.4) Hypotensive effect: Increased risk with compromised ability to maintain blood pressure. (5.5) Prolonged gastric obstruction: Do not administer codeine sulfate to patients with gastrointestinal obstruction, especially paralytic ileus. (5.6) Pancreatic/biliary tract disease: May cause spasm of the sphincter of Oddi and diminish biliary and pancreatic secretions. (5.7) Ultra-rapid metabolizers: Conversion of codeine into its active metabolite, morphine, may occur more rapidly and completely resulting in higher than expected morphine levels and overdose symptoms. (5.9) Impaired mental/physical abilities: Caution must be used with potentially hazardous activities. (5.10) Side EffectsThe most common adverse reactions include: drowsiness, light-headedness, dizziness, sedation, shortness of breath, nausea, vomiting, sweating, and constipation. (6) To report SUSPECTED ADVERSE REACTIONS, contact Roxane Laboratories, Inc. at 1-800-962-8364 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch DRUG INTERACTIONS CNS depressants: Increased risk of additive CNS depression. Use with caution in reduced dosages. (7.1) Anticholinergics: Additive risk of urinary retention and paralytic ileus. (7.3) Antidepressants: May cause excessive sedation, acute hypotension and excessive anticholinergic effects. Codeine sulfate should not be used in patients taking MAOIs or within 14 days of stopping such treatment. (7.4) CYP2D6 inhibitors and CYP3A4 inhibitors and inducers: Concomitant use of cytochrome P450 2D6 and 3A4 enzyme inducers or inhibitors may result in an altered response to codeine. Monitor analgesic activity and adverse drug reactions. (7.5) USE IN SPECIFIC POPULATIONS Pregnancy: Based on animal data, may cause fetal harm. (8.1) Nursing mothers: The risk of infant exposure to codeine and morphine through breast milk should be weighed against the benefits of breastfeeding for both the mother and the baby. (8.3) Geriatric patients (8.5), Renal impairment (8.6), Hepatic impairment (8.7): Use caution during dose selection, starting at the low end of the dosing range while carefully monitoring for side effects.
FULL PRESCRIBING INFORMATION: CONTENTS*
- 1 CODEINE SULFATE INDICATIONS AND USAGE
- 2 CODEINE SULFATE DOSAGE AND ADMINISTRATION
- 3 DOSAGE FORMS AND STRENGTHS
- 4 CODEINE SULFATE CONTRAINDICATIONS
- 5 WARNINGS AND PRECAUTIONS
- 5.1 Respiratory Depression
- 5.2 Misuse and Abuse of Opioids
- 5.3 Interaction with Alcohol and Drugs of Abuse
- 5.4 Head Injury and Increased Intracranial Pressure
- 5.5 Hypotensive Effect
- 5.6 Gastrointestinal Effects
- 5.7 Use in Pancreatic/Biliary Tract Disease
- 5.8 Special Risk Patients
- 5.9 Ultra-Rapid Metabolizers of Codeine
- 5.10 Driving and Operating Machinery
- 6 CODEINE SULFATE ADVERSE REACTIONS
- 7 DRUG INTERACTIONS
- 8 USE IN SPECIFIC POPULATIONS
- 9 DRUG ABUSE AND DEPENDENCE
- 10 OVERDOSAGE
- 11 CODEINE SULFATE DESCRIPTION
- 12 CLINICAL PHARMACOLOGY
- 13 NONCLINICAL TOXICOLOGY
- 16 HOW SUPPLIED/STORAGE AND HANDLING
- 17 PATIENT COUNSELING INFORMATION
FULL PRESCRIBING INFORMATION
1 INDICATIONS AND USAGE
Codeine sulfate is an opioid analgesic indicated for the management of mild to moderately severe pain where the use of an opioid analgesic is appropriate.
2 DOSAGE AND ADMINISTRATION
Selection of patients for treatment with codeine sulfate should be governed by the same principles that apply to the use of similar opioid analgesics. Individualize treatment in every case, using non-opioid analgesics, opioids on an as needed basis and/or combination products, and chronic opioid therapy in a progressive plan of pain management such as outlined by the World Health Organization, the Agency for Healthcare Research and Quality, and the American Pain Society.
2.1 Individualization of Dosage
As with any opioid drug product, adjust the dosing regimen for each patient individually, taking into account the patient's prior analgesic treatment experience. In the selection of the initial dose of codeine sulfate, attention should be given to the following:
- the total daily dose, potency and specific characteristics of the opioid the patient has been taking previously;
- the reliability of the relative potency estimate used to calculate the equivalent codeine sulfate dose needed;
- the patient's degree of opioid tolerance;
- the general condition and medical status of the patient;
- concurrent medications;
- the type and severity of the patient's pain;
- risk factors for abuse or addiction, including a prior history of abuse and addiction.
The following dosing recommendations, therefore, can only be considered suggested approaches to what is actually a series of clinical decisions over time in the management of the pain of each individual patient.
Continual re-evaluation of the patient receiving codeine sulfate is important, with special attention to the maintenance of pain management and the relative incidence of side effects associated with therapy. During chronic therapy, especially for noncancer-related pain, the continued need for the use of opioid analgesics should be re-assessed as appropriate.
During periods of changing analgesic requirements, including initial titration, frequent contact is recommended between the physician, other members of the healthcare team, the patient, and the caregiver/family.
2.2 Initiation of Therapy
The usual adult dosage is 15 mg to 60 mg (2.5 mL to 10 mL) repeated up to every four hours as needed for pain. The maximum 24 hour dose is 360 mg.
Titrate the dose based upon the individual patient's response to their initial dose of codeine. Adjust the dose to an acceptable level of analgesia taking into account the improvement in pain intensity and the tolerability of the codeine by the patient.
It should be kept in mind, however, that tolerance to codeine sulfate can develop with continued use and that the incidence of untoward effects is dose-related. Adult doses of codeine higher than 60 mg fail to give commensurate relief of pain and are associated with an appreciably increased incidence of undesirable side effects.
2.3 Cessation of Therapy
When the patient no longer requires therapy with codeine sulfate, gradually taper the dose to prevent signs and symptoms of withdrawal in the physically dependent patient.
3 DOSAGE FORMS AND STRENGTHS
Each 5 mL of clear, reddish-orange to orange codeine sulfate oral solution contains codeine sulfate, USP 30 mg. The concentration of the 30 mg per 5 mL solution is 6 mg/mL.
4 CONTRAINDICATIONS
Codeine sulfate is contraindicated in patients with known hypersensitivity to codeine or any components of the product. Persons known to be hypersensitive to certain other opioids may exhibit cross-sensitivity to codeine.
Codeine sulfate is contraindicated in patients with respiratory depression in the absence of resuscitative equipment.
Codeine sulfate is contraindicated in patients with acute or severe bronchial asthma or hypercarbia.
Codeine sulfate is contraindicated in any patient who has or is suspected of having paralytic ileus.
5 WARNINGS AND PRECAUTIONS
5.1 Respiratory Depression
Respiratory depression is the primary risk of codeine sulfate. Respiratory depression occurs more frequently in elderly or debilitated patients and in those suffering from conditions accompanied by hypoxia, hypercapnia, or upper airway obstruction, in whom even moderate therapeutic doses may significantly decrease pulmonary ventilation. Codeine produces doserelated respiratory depression.
Caution should be exercised when codeine sulfate is used postoperatively, in patients with pulmonary disease or shortness of breath, or whenever ventilatory function is depressed. Use opioids, including codeine sulfate, with extreme caution in patients with chronic obstructive pulmonary disease or cor pulmonale and in patients having a substantially decreased respiratory reserve (e.g., severe kyphoscoliosis), hypoxia, hypercapnia, or pre-existing respiratory depression. In such patients, even usual therapeutic doses of codeine sulfate may increase airway resistance and decrease respiratory drive to the point of apnea. Consider alternative non-opioid analgesics and use codeine sulfate only under careful medical supervision at the lowest effective dose in such patients. [see Overdosage (10)]
5.2 Misuse and Abuse of Opioids
Codeine sulfate is an opioid agonist of the morphine-type and a Schedule II controlled substance. Such drugs are sought by drug abusers and people with addiction disorders. Diversion of Schedule II products is an act subject to criminal penalty.
Patients should be assessed for their risk for opioid abuse or addiction prior to being prescribed opioids.
Codeine can be abused in a manner similar to other opioid agonists, legal or illicit. This should be considered when prescribing or dispensing codeine sulfate in situations where the physician or pharmacist is concerned about an increased risk of misuse, abuse, or diversion.
Codeine may be abused by crushing, chewing, snorting or injecting the product. Misuse and abuse of codeine sulfate poses a significant risk to the abuser that could result in overdose and death. [see Drug Abuse and Dependence (9.2)]
Concerns about abuse, addiction, and diversion should not prevent the proper management of pain. Healthcare professionals should contact their State Professional Licensing Board or State Controlled Substances Authority for information on how to prevent and detect abuse or diversion of this product.
5.3 Interaction with Alcohol and Drugs of Abuse
Codeine sulfate may be expected to have additive effects when used in conjunction with alcohol, other opioids, or illicit drugs that cause central nervous system depression, because respiratory depression, hypotension, profound sedation, coma or death may result.
5.4 Head Injury and Increased Intracranial Pressure
Respiratory depressant effects of opioids and their capacity to elevate cerebrospinal fluid pressure resulting from vasodilation following CO2 retention may be markedly exaggerated in the presence of head injury, other intracranial lesions or a pre-existing increase in intracranial pressure. Furthermore, opioids including codeine sulfate, can produce effects on pupillary response and consciousness, which may obscure neurologic signs of further increases in intracranial pressure in patients with head injuries.
5.5 Hypotensive Effect
Codeine sulfate may cause severe hypotension in an individual whose ability to maintain blood pressure has already been compromised by a depleted blood volume or concurrent administration of drugs such as phenothiazines or general anesthetics. Codeine sulfate may produce orthostatic hypotension and syncope in ambulatory patients.
Administer codeine sulfate with caution to patients in circulatory shock, as vasodilation produced by the drug may further reduce cardiac output and blood pressure.
5.6 Gastrointestinal Effects
Do not administer codeine sulfate to patients with gastrointestinal obstruction, especially paralytic ileus because codeine sulfate diminishes propulsive peristaltic waves in the gastrointestinal tract and may prolong the obstruction.
Chronic use of opioids, including codeine sulfate, may result in obstructive bowel disease especially in patients with underlying intestinal motility disorder. Codeine sulfate may cause or aggravate constipation.
The administration of codeine sulfate may obscure the diagnosis or clinical course of patients with acute abdominal conditions.
5.7 Use in Pancreatic/Biliary Tract Disease
Use codeine sulfate with caution in patients with biliary tract disease, including acute pancreatitis, as codeine sulfate may cause spasm of the sphincter of Oddi and diminish biliary and pancreatic secretions.
5.8 Special Risk Patients
Use codeine sulfate with caution in patients with severe renal or hepatic impairment, hypothyrodism, Addison's disease, prostatic hypertrophy, or urethral stricture and in elderly or debilitated patients. [see Use in Specific Populations (8.5)] The usual precautions should be observed and the possibility of respiratory depression should be kept in mind.
Extreme caution should be exercised in the administration of codeine sulfate to patients with CNS depression, acute alcoholism, and delirium tremens.
All opioids may aggravate convulsions in patients with convulsive disorders, and all opioids may induce or aggravate seizures in some clinical settings.
Keep Codeine Sulfate Oral Solution out of the reach of children. In case of accidental ingestion, seek emergency medical help immediately.
5.9 Ultra-Rapid Metabolizers of Codeine
Some individuals may be ultra-rapid metabolizers due to a specific CYP2D6*2x2 genotype. These individuals convert codeine into its active metabolite, morphine, more rapidly and completely than other people. This rapid conversion results in higher than expected serum morphine levels. Even at labeled dosage regimens, individuals who are ultra-rapid metabolizers may experience overdose symptoms such as extreme sleepiness, confusion, or shallow breathing.
The prevalence of this CYP2D6 phenotype varies widely and has been estimated at 0.5 to 1% in Chinese and Japanese, 0.5 to 1% in Hispanics, 1 to 10% in Caucasians, 3% in African Americans, and 16 to 28% in North Africans, Ethiopians, and Arabs. Data are not available for other ethnic groups.
When physicians prescribe codeine-containing drugs, they should choose the lowest effective dose for the shortest period of time and inform their patients about these risks and the signs of morphine overdose. [see Use in Specific Populations (8.3)]
5.10 Driving and Operating Machinery
Caution patients that codeine sulfate could impair the mental and/or physical abilities needed to perform potentially hazardous activities such as driving a car or operating machinery.
Caution patients about the potential combined effects of codeine sulfate with other CNS depressants, including other opioids, phenothiazines, sedative/hypnotics, and alcohol. [see Drug Interactions (7.1)]
6 ADVERSE REACTIONS
Serious adverse reactions associated with codeine are respiratory depression and, to a lesser degree, circulatory depression, respiratory arrest, shock, and cardiac arrest.
The most frequently observed adverse reactions with codeine administration include drowsiness, lightheadedness, dizziness, sedation, shortness of breath, nausea, vomiting, sweating, and constipation.
Other adverse reactions include allergic reactions, euphoria, dysphoria, abdominal pain, and pruritis.
Other less frequently observed adverse reactions expected from opioid analgesics, including codeine sulfate, include:
Cardiovascular system: faintness, flushing, hypotension, palpitations, syncope
Digestive System: abdominal cramps, anorexia, diarrhea, dry mouth, gastrointestinal distress, pancreatitis
Nervous system: anxiety, drowsiness, fatigue, headache, insomnia, nervousness, shakiness, somnolence, vertigo, visual disturbances, weakness
Skin and Appendages: rash, sweating, urticaria
7 DRUG INTERACTIONS
7.1 Central Nervous System (CNS) Depressants
Concurrent use of other opioids, antihistamines, antipsychotics, antianxiety agents, or other CNS depressants (including sedatives, hypnotics, general anesthetics, antiemetics, phenothiazines, or other tranquilizers or alcohol) concomitantly with codeine sulfate may result in additive CNS depression, respiratory depression, hypotension, profound sedation, or coma. Use codeine sulfate with caution and in reduced dosages in patients taking these agents.
7.2 Mixed Agonist/Antagonist Opioid Analgesics
Do not administer mixed agonist/antagonist analgesics (i.e., pentazocine, nalbuphine, and butorphanol) to patients who have received or are receiving a course of therapy with a pure opioid agonist analgesic such as codeine sulfate. In these patients, mixed agonist/antagonist analgesics may reduce the analgesic effect and/or may precipitate withdrawal symptoms.
7.3 Anticholinergics
Anticholinergics or other medications with anticholinergic activity when used concurrently with opioid analgesics may result in increased risk of urinary retention and/or severe constipation, which may lead to paralytic ileus.
7.4 Antidepressants
Use of monoamine oxidase inhibitors (MAOIs) or tricyclic antidepressants with codeine sulfate may increase the effect of either the antidepressant or codeine. MAOIs markedly potentiate the action of morphine, the major metabolite of codeine. Codeine should not be used in patients taking MAOIs or within 14 days of stopping such treatment.
7.5 CYP2D6 and CYP3A4 Inhibitors and Inducers
Codeine is metabolized by the cytochrome P450 2D6 and 3A4 isoenzymes [see Clinical Pharmacology (12.3)]. Patients taking CYP2D6 inhibitors or CYP3A4 inhibitors or inducers may demonstrate an altered response to codeine, therefore analgesic activity should be monitored.
Inhibitors of CYP2D6 or CYP3A4: Since the CYP2D6 and CYP3A4 isoenzymes play a major role in the metabolism of codeine, drugs that inhibit CYP3A4 (e.g., macrolide antibiotics (e.g., erythromycin), azole-antifungal agents (e.g., ketoconazole), protease inhibitors (e.g., ritonavir)), or CYP2D6 activity (e.g., certain cardiovascular drugs including amiodarone and quinidine as well as polycyclic antidepressants), may cause decreased clearance of codeine which could lead to an increase in codeine plasma concentrations. If coadministration with codeine sulfate oral solution is necessary, caution is advised when initiating therapy with, currently taking, or discontinuing CYP450 inhibitors. Evaluate these patients at frequent intervals and consider dose adjustments until stable drug effects are achieved. [see Clinical Pharmacology (12.3)]
Inducers of CYP3A4: CYP450 inducers, such as rifampin, carbamazepine, and phenytoin, may induce the metabolism of codeine and, therefore, may cause increased clearance of the drug which could lead to a decrease in codeine plasma concentrations, lack of efficacy or, possibly, development of an abstinence syndrome in a patient who had developed physical dependence to codeine. If co-administration with codeine sulfate oral solution is necessary, caution is advised when initiating therapy with, currently taking, or discontinuing CYP3A4 inducers. Evaluate these patients at frequent intervals and consider dose adjustments until stable drug effects are achieved.
7.6 Drug-Laboratory Test Interaction
Codeine may cause an elevation of plasma amylase and lipase due to the potential of codeine to produce spasm of the sphincter of Oddi. Determination of these enzyme levels may be unreliable for some time after an opiate agonist has been given.
8 USE IN SPECIFIC POPULATIONS
8.1 Pregnancy
Teratogenic Effects
Pregnancy Category C
There are no adequate and well-controlled studies in pregnant women. Codeine should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
Codeine has been shown to have embryolethal and fetotoxic effects (reduced fetal body weights and delayed or incomplete ossification) in the hamster, rat and mouse models at approximately 2 to 4 times the maximum recommended human dose of 360 mg/day based on a body surface area comparison. Maternally toxic doses that were approximately 7 times the maximum recommended human dose of 360 mg/day, were associated with evidence of resorptions and incomplete ossification, including meningioencephalocele and cranioschisis. In contrast, codeine did not demonstrate evidence of embryotoxicity or fetotoxicity in the rabbit model at doses up to 2 times the maximum recommended human dose of 360 mg/day based on a body surface area comparison. [see Nonclinical Pharmacology (13.3)]
Nonteratogenic Effects
Neonatal codeine withdrawal has occurred in infants born to addicted and non-addicted mothers who had been taking codeine-containing medications in the days prior to delivery. Typical symptoms of narcotic withdrawal include irritability, excessive crying, tremors, hyperreflexia, seizures, fever, vomiting, diarrhea, and poor feeding. These signs occur shortly after birth and may require specific treatment.
Codeine (30 mg/kg) administered subcutaneously to pregnant rats during pregnancy and for 25 days after delivery increased neonatal mortality at birth. This dose is 0.8 times the maximum recommended human dose of 360 mg/day on a body surface area comparison.
8.2 Labor and Delivery
Opioid analgesics cross the placenta and may produce respiratory depression and psychophysiologic effects in neonates. Codeine is not recommended for use in women during and immediately prior to labor. Occasionally, opioid analgesics may prolong labor through actions which temporarily reduce the strength, duration, and frequency of uterine contractions. However, this effect is not consistent and may be offset by an increased rate of cervical dilatation, which tends to shorten labor. Closely observe neonates whose mothers received opioid analgesics during labor for signs of respiratory depression. Have a specific opioid antagonist, such as naloxone, available for reversal of opioid-induced respiratory depression in the neonate.
8.3 Nursing Mothers
Codeine is secreted into human milk. In women with normal codeine metabolism (normal CYP2D6 activity), the amount of codeine secreted into human milk is low and dose-dependent. However, some women are ultra-rapid metabolizers of codeine. These women achieve higherthan-expected serum levels of codeine's active metabolite, morphine, leading to higher-thanexpected levels of morphine in breast milk and potentially dangerously high serum morphine levels in their breastfed infants. Therefore, maternal use of codeine can potentially lead to serious adverse reactions, including death, in nursing infants.
The prevalence of this CYP2D6 phenotype varies widely and has been estimated at 0.5 to 1% in Chinese and Japanese, 0.5 to 1% in Hispanics, 1 to 10% in Caucasians, 3% in African Americans, and 16 to 28% in North Africans, Ethiopians, and Arabs. Data are not available for other ethnic groups.
The risk of infant exposure to codeine and morphine through breast milk should be weighed against the benefits of breastfeeding for both the mother and the baby. Caution should be exercised when codeine is administered to a nursing woman. If a codeine containing product is selected, the lowest dose should be prescribed for the shortest period of time to achieve the desired clinical effect. Mothers using codeine should be informed about when to seek immediate medical care and how to identify the signs and symptoms of neonatal toxicity, such as drowsiness or sedation, difficulty breastfeeding, breathing difficulties, and decreased tone, in their baby. Nursing mothers who are ultra-rapid metabolizers may also experience overdose symptoms such as extreme sleepiness, confusion, or shallow breathing. Prescribers should closely monitor mother-infant pairs and notify treating pediatricians about the use of codeine during breast-feeding [see Warnings and Precautions (5.9)].
8.4 Pediatric Use
The safety, effectiveness and the pharmacokinetics of codeine sulfate in pediatric patients below the age of 18 have not been established.
8.5 Geriatric Use
Codeine may cause confusion and over-sedation in the elderly (aged 65 and older). In general, use caution when selecting a dose for an elderly patient, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
8.6 Renal Impairment
Codeine pharmacokinetics may be altered in patients with renal failure. Clearance may be decreased and the metabolites may accumulate to much higher plasma levels in patients with renal failure as compared to patients with normal renal function. Start these patients cautiously with lower doses of codeine sulfate or with longer dosing intervals and titrate slowly while carefully monitoring for side effects.
8.7 Hepatic Impairment
No formal studies have been conducted in patients with hepatic impairment so the pharmacokinetics of codeine in this patient population are unknown. Start these patients cautiously with lower doses of codeine sulfate or with longer dosing intervals and titrate slowly while carefully monitoring for side effects.
9 DRUG ABUSE AND DEPENDENCE
9.1 Controlled Substance
Codeine sulfate is an opioid agonist and is a Schedule II controlled substance. Codeine sulfate can be abused and is subject to criminal diversion.
9.2 Abuse
Drug addiction is characterized by compulsive use, use for non-medical purposes, and continued use despite harm or risk of harm. Drug addiction is a treatable disease, utilizing a multidisciplinary approach, but relapse is common.
"Drug seeking" behavior is very common in addicts and drug abusers. Drug-seeking tactics include emergency calls or visits near the end of office hours, refusal to undergo appropriate examination, testing or referral, repeated "loss" of prescriptions, tampering with prescriptions and reluctance to provide prior medical records or contact information for other treating physician(s). "Healthcare provider shopping" to obtain additional prescriptions is common among drug abusers and people suffering from untreated addiction.
The risks of misuse and abuse should be considered when prescribing or dispensing codeine sulfate. Concerns about abuse and addiction, should not prevent the proper management of pain, however, treatment of pain should be individualized, balancing the potential benefits and risks for each patient.
Abuse and addiction are separate and distinct from physical dependence and tolerance. Physicians should be aware that addiction may not be accompanied by concurrent tolerance and symptoms of physical dependence. The converse is also true. In addition, abuse of opioids can occur in the absence of true addiction and is characterized by misuse for non-medical purposes, often in combination with other psychoactive substances. Careful record-keeping of prescribing information, including quantity, frequency, and renewal requests is strongly advised.
Codeine is intended for oral use only. Abuse of codeine poses a risk of overdose and death. The risk is increased with concurrent abuse of alcohol and other substances. Parenteral drug abuse is commonly associated with transmission of infectious diseases such as hepatitis and HIV.
Proper assessment of the patient, proper prescribing practices, periodic re-evaluation of therapy, and proper dispensing and storage are appropriate measures that help to limit abuse of opioid drugs.
Infants born to mothers physically dependent on opioids will also be physically dependent and may exhibit respiratory difficulties and withdrawal symptoms. [see Use in Specific Populations (8.2)]
9.3 Dependence
Tolerance to opioids is the need for increasing doses of opioids to maintain a defined effect such as analgesia (in the absence of disease progression or other external factors). The first sign of tolerance is usually a reduced duration of effect. Tolerance to different effects of opioids may develop to varying degrees and at varying rates in a given individual. There is also inter-patient variability in the rate and extent of tolerance that develops to various opioid effects, whether the effect is desirable (e.g., analgesia) or undesirable (e.g., nausea). Physical dependence is manifested by withdrawal symptoms after abrupt discontinuation of a drug or upon administration of an antagonist. Physical dependence and tolerance are frequent during chronic opioid therapy.
Instruct patients using codeine sulfate not to change their dose without first contacting their health care providers. The opioid abstinence or withdrawal syndrome is characterized by some or all of the following: restlessness, lacrimation, rhinorrhea, yawning, perspiration, chills, myalgia, and mydriasis. Other symptoms also may develop, including irritability, anxiety, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhea, or increased blood pressure, respiratory rate, or heart rate.
In general, opioids should not be abruptly discontinued. [see Dosage and Administration (2.3)]
10 OVERDOSAGE
10.1 Symptoms
Acute overdose with codeine is characterized by respiratory depression (a decrease in respiratory rate and/or tidal volume, Cheyne-Stokes respiration, cyanosis), extreme somnolence progressing to stupor or coma, skeletal muscle flaccidity, cold and clammy skin, constricted pupils, and sometimes bradycardia and hypotension. In severe overdosage, apnea, circulatory collapse, cardiac arrest, and death may occur.
Codeine may cause miosis, even in total darkness. Pinpoint pupils are a sign of opioid overdose but are not pathognomonic (e.g., pontine lesions of hemorrhagic or ischemic origin may produce similar findings). Marked mydriasis rather than miosis may be seen with hypoxia in overdose situations.
10.2 Treatment
Give primary attention to re-establishment of a patent airway and institution of assisted or controlled ventilation. Employ supportive measures (including oxygen and vasopressors) in the management of circulatory shock and pulmonary edema accompanying overdose as indicated. Cardiac arrest or arrhythmias may require cardiac massage or defibrillation. Induction of emesis is not recommended because of the potential for CNS depression and seizures. Activated charcoal is recommended if the patient is awake and able to protect his/her airway. In persons who are at risk for abrupt onset of seizures or mental status depression, activated charcoal should be administered by medical or paramedical personnel capable of airway management to prevent aspiration in the event of spontaneous emesis. Severe agitation or seizures should be treated with an intravenous benzodiazepine.
The pure opioid antagonist, naloxone, is a specific antidote to respiratory depression resulting from opioid overdose. Since the duration of reversal is expected to be less than the duration of action of codeine sulfate, carefully monitor the patient until spontaneous respiration is reliably reestablished. If the response to opioid antagonists is suboptimal or only brief in nature, administer additional antagonist as directed by the label of the product.
Do not administer opioid antagonists in the absence of clinically significant respiratory or circulatory depression secondary to codeine sulfate overdose. In an individual physically dependent on opioids, administration of the usual dose of the antagonist will precipitate an acute withdrawal syndrome. The severity of the withdrawal symptoms experienced will depend on the degree of physical dependence and the dose of the antagonist administered. Reserve use of an opioid antagonist for cases where such treatment is clearly needed. If it is necessary to treat serious respiratory depression in the physically dependent patient, initiate administration of the antagonist with care and titrate with smaller than usual doses.
11 DESCRIPTION
Chemically, codeine sulfate is morphinan-6-ol,7,8-didehydro-4,5-epoxy-3-methoxy-17-methyl- (5α,6α)-, sulfate (2:1) (salt), trihydrate. Codeine sulfate trihydrate is a fine, white, crystalline powder which is soluble in water and insoluble in chloroform and ether. Its empirical formula is (C18H21NO3)2 • H2SO4 • 3H2O and its molecular weight is 750.85 g/mol.
Its structure is as follows:
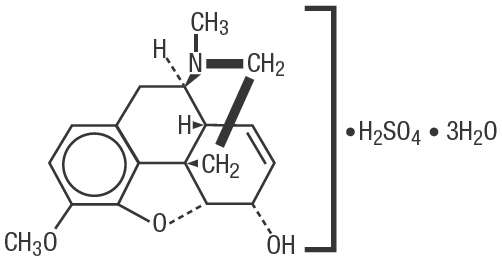
Each 5 mL of oral solution contains 30 mg of codeine sulfate, USP and the following inactive ingredients: sorbitol, glycerin, ascorbic acid, citric acid, disodium edetate, sucralose, sodium benzoate, FD&C Yellow No. 6, FD&C Red No. 40, Orange Flavor XBF-709818, and water. The pH of the oral solution is 3.3.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Codeine is an opioid agonist, related to morphine, but with less potent analgesic properties. Codeine is selective for the mu receptor, but with a much weaker affinity than morphine. The analgesic properties of codeine have been speculated to come from its conversion to morphine, although the exact mechanism of analgesic action remains unknown.
Effects of the Central Nervous System (CNS): The principal therapeutic action of codeine is analgesia. Although the precise mechanism of the analgesic action is unknown, specific CNS opiate receptors and endogenous compounds with morphine-like activity have been identified throughout the brain and spinal cord and are likely to play a role in the expression and perception of analgesic effects. Other CNS effects of codeine include anxiolysis, euphoria, and feelings of relaxation. Codeine causes respiratory depression, in part by a direct effect on the brainstem respiratory centers. Codeine and other related opioids depress the cough reflex by direct effect on the cough center in the medulla. Codeine may also cause miosis.
Effects on the Gastrointestinal Tract and on Other Smooth Muscle: Gastric, biliary and pancreatic secretions may be decreased by codeine. Codeine also causes a reduction in motility and is associated with an increase in tone in the antrum of the stomach and duodenum. Digestion of food in the small intestine is delayed and propulsive contractions are decreased. Propulsive peristaltic waves in the colon are decreased, while tone is increased to the point of spasm. The end result may be constipation. Codeine can cause a marked increase in biliary tract pressure as a result of the spasm of the sphincter of Oddi. Codeine may also cause spasms of the sphincter of the urinary bladder.
Effects on the Cardiovasclar System: In therapeutic doses, codeine does not usually exert major effects on the cardiovascular system. Codeine produces peripheral vasodilation which may result in orthostatic hypotension and fainting. Release of histamine can occur, which may play a role in opioid-induced hypotension. Manifestations of histamine release and/or peripheral vasodilation may include pruritus, flushing, red eyes, and sweating.
Endocrine System: Opioid agonists have been shown to have a variety of effects on the secretion of hormones. Opioids inhibit the secretion of ACTH, cortisol, and luteinizing hormone (LH) in humans. They also stimulate prolactin, growth hormone (GH) secretion, and pancreatic secretion of insulin and glucagons in humans and other species, rats and dogs. Thyroid stimulating hormone (TSH) has been shown to be both inhibited and stimulated by opioids.
Immune System: Opioids have been shown to have a variety of effects on components of the immune system in in vitro and animal models. The clinical significance of these findings is unknown.
12.2 Pharmacodynamics
Codeine plasma concentrations do not correlate with codeine brain concentrations or relief of pain.
The minimum effective concentration varies widely and is influenced by a variety of factors, including the extent of previous opioid use, age and general medical condition. Effective doses in tolerant patients may be significantly higher than in opioid-naïve patients.
12.3 Pharmacokinetics
Absorption: Codeine, when administered as codeine sulfate, is absorbed from the gastrointestinal tract with maximum plasma concentration occurring 60 minutes post administration.
Food Effects: When 60 mg codeine sulfate was administered 30 minutes after ingesting a high fat/high calorie meal, there was no significant change in the rate and extent of absorption of codeine.
Steady-state: Administration of 15 mg codeine sulfate every four hours for 5 days resulted in steady-state concentrations of codeine, morphine, morphine-3-glucuronide (M3G) and morphine- 6-glucuronide (M6G) within 48 hours.
Distribution: Codeine has been reported to have an apparent volume of distribution of approximately 3-6 L/kg, indicating extensive distribution of the drug into tissues. Codeine has low plasma protein binding with about 7-25% of codeine bound to plasma proteins.
Metabolism: About 70-80% of the administered dose of codeine is metabolized by conjugation with glucuronic acid to codeine-6-glucuronide (C6G, about 60%) and via O-demethylation to morphine (about 5-10%) and N-demethylation to norcodeine (about 10%) respectively. UDPglucuronosyltransferase (UGT) 2B7 and 2B4 are the major enzymes mediating glucurodination of codeine to C6G. Cytochrome P450 2D6 is the major enzyme responsible for conversion of codeine to morphine (about 5-10%) and P450 3A4 is the major enzyme mediating conversion of codeine to norcodeine. Morphine and norcodeine are further metabolized by conjugation with glucuronic acid. The glucuronide metabolites of morphine are morphine-3-glucuronide (M3G) and morphine- 6-glucuronide (M6G). Morphine and M6G are known to have analgesic activity in humans. The analgesic activity of C6G in humans is unknown. Norcodeine and M3G are generally not considered to possess analgesic properties.
Elimination: Approximately 90% of the total dose of codeine is excreted through the kidneys, of which approximately 10% is unchanged codeine. Plasma half-lives of codeine and its metabolites have been reported to be approximately 3 hours.
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis: Two year carcinogenicity studies have been conducted in F344/N rats and B6C3F1 mice. There was no evidence of carcinogenicity in male and female rats, respectively, at dietary doses up to 70 and 80 mg/kg/day of codeine (approximately 2 times the maximum recommended daily dose of 360 mg/day for adults on a mg/m2 basis) for two years. Similarly there was no evidence of carcinogenicity activity in male and female mice at dietary doses up to 400 mg/kg/day of codeine (approximately 5 times the maximum recommended daily dose of 360 mg/day for adults on a mg/m2 basis) for two years.
Mutagenesis: Codeine was not mutagenic in the in vitro bacterial reverse mutation assay or clastogenic in the in vitro Chinese hamster ovary cell chromosome aberration assay.
Impairment of Fertility: No animal studies were conducted to evaluate the effect of codeine on male or female fertility.
13.3 Reproduction and Developmental Toxicology
Studies on the reproductive and developmental effects of codeine have been reported in the published literature in hamsters, rats, mice and rabbits.
A study in hamsters administered 150 mg/kg twice daily of codeine (oral; approximately 7 times the maximum recommended daily dose of 360 mg/day for adults on a mg/m2 basis) reported the development of cranial malformations (i.e., meningoencephalocele) in several fetuses examined; as well as the observation of increases in the percentage of resorptions per litter examined. Doses of 50 and 150 mg/kg, bid resulted in fetotoxicity as demonstrated by decreased fetal body weight. In an earlier study in hamsters, doses of 73-360 mg/kg level (oral; approximately 2-8 times the maximum recommended daily dose of 360 mg/day for adults on a mg/m2 basis), reportedly produced cranioschisis in all of the fetuses examined.
In studies in rats, doses at the 120 mg/kg level (oral; approximately 3 times the maximum recommended daily dose of 360 mg/day for adults on a mg/m2 basis), in the toxic range for the adult animal, were associated with an increase in embryo resorption at the time of implantation.
In pregnant mice, a single 100 mg/kg dose (subcutaneous; approximately 1.4 times the recommended daily dose of 360 mg/day for adults on a mg/m2 basis) reportedly resulted in delayed ossification in the offspring.
No teratogenic effects were observed in rabbits administered up to 30 mg/kg (approximately 2 times the maximum recommended daily dose of 360 mg/day for adults on a mg/m2 basis) of codeine during organogenesis.
16 HOW SUPPLIED/STORAGE AND HANDLING
Codeine Sulfate Oral Solution
Codeine Sulfate Oral Solution, 30 mg per 5 mL is a clear, reddish-orange to orange solution available as follows:
NDC 68094-760-62
2.5 mL per unit dose cup
Thirty (30) cups per shipper
NDC 68094-761-62
5 mL per unit dose cup
Thirty (30) cups per shipper
Storage
Store at controlled room temperature, 20° to 25°C (68° to 77°F), excursions permitted between 15° and 30°C (between 59° and 86°F).
Protect from light and moisture.
Dispense in well-closed container as defined in the USP/NF.
All opioids, including codeine sulfate, are liable to diversion and misuse both by the general public and healthcare workers and should be handled accordingly.
17 PATIENT COUNSELING INFORMATION
See FDA-approved patient labeling.
17.1 Information for Patients and Caregivers
- Advise patients that codeine sulfate is a narcotic pain medication and should be taken only as directed.
- Advise patients not to adjust the dose of codeine sulfate without consulting a physician or other healthcare professional.
- Advise patients that codeine may cause drowsiness, dizziness, or light-headedness and may impair the mental and/or physical abilities required for the performance of potentially hazardous tasks (e.g., driving, operating machinery). Advise patients started on codeine sulfate or patients whose dose has been adjusted to refrain from any potentially dangerous activity until it is established that they are not adversely affected.
- Advise patients that codeine sulfate will add to the effects of alcohol and other CNS depressants (such as antihistamines, sedatives, hypnotics, tranquilizers, general anesthetics, phenothiazines, other opioids, and monoamine oxidase [MAO] inhibitors).
- Advise patients not to combine codeine sulfate with central nervous system depressants (sleep aids, tranquilizers) except by the orders of the prescribing physician, and not to combine with alcohol because dangerous additive effects may occur, resulting in serious injury or death.
- Advise patients that codeine sulfate is a potential drug of abuse. They must protect it from theft. It should never be given to anyone other than the individual for whom it was prescribed.
- Advise patients to keep codeine sulfate in a secure place out of the reach of children. When codeine sulfate is no longer needed, the unused solution should be destroyed by flushing down the toilet.
- Advise patients of the potential for severe constipation when taking codeine sulfate; appropriate laxatives and/or stool softeners as well as other appropriate treatments should be initiated from the onset of therapy.
- Advise patients of the most common adverse events that may occur while taking codeine sulfate: drowsiness, lightheadedness, dizziness, sedation, shortness of breath, nausea, vomiting, constipation, and sweating.
- Advise patients that some people have a genetic variation that results in their liver changing codeine into morphine more rapidly and completely than other people. These people are more likely to have higher-than-normal levels of morphine in their blood after taking codeine, which can result in overdose symptoms such as extreme sleepiness, confusion, or shallow breathing. In most cases, it is unknown if someone is an ultra-rapid codeine metabolizer. Nursing mothers taking codeine can also have higher morphine levels in their breast milk if they are ultra-rapid metabolizers. These higher levels of morphine in breast milk may lead to life-threatening or fatal side effects in nursing babies. Nursing mothers should be advised to watch for signs of morphine toxicity in their infants which includes increased sleepiness (more than usual), difficulty breastfeeding, breathing difficulties, or limpness. Instruct nursing mothers to talk to the baby's healthcare provider immediately if they notice these signs and, if they cannot reach the healthcare provider right away, to take the baby to an emergency room or call 911 (or local emergency services).
- Advise patients that if they miss one dose of Codeine Sulfate Oral Solution they can take the dose when they remember it if they have pain, or they can wait for the next dose.
- If patients have been receiving treatment with codeine sulfate for more than a few weeks and cessation of therapy is indicated, counsel them on the importance of safely tapering the dose and that abruptly discontinuing the medication could precipitate withdrawal symptoms. Provide a dose schedule to accomplish a gradual discontinuation of the medication.
- Advise women of childbearing potential who become or are planning to become pregnant to consult a physician prior to initiating or continuing therapy with codeine sulfate.
- Advise patients that safe use in pregnancy has not been established and prolonged use of opioid analgesics during pregnancy may cause fetal-neonatal physical dependence, and neonatal withdrawal may occur.
Manufactured by:
Roxane Laboratories, Inc., Columbus, Ohio 43216
Manufactured for:
TAGI Pharma, Inc., 722 Progressive Lane, Room 205, South Beloit, IL 61080
Packaged By:
Precision Dose, Inc., South Beloit, IL 61080
LI888 Rev. 11/12
PRINCIPAL DISPLAY PANEL - 30 mg/5 mL Dose Cup Label
NDC 68094-761-59
PrecisionDose™
CODEINE SULFATE
Oral Solution
30 mg/5 mL
CII
Pkg: Precision Dose, Inc., S. Beloit, IL 61080

Codeine SulfateCodeine Sulfate SOLUTION
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||