A3301-25 PORTEX SPINAL 25G WHITACRE
FULL PRESCRIBING INFORMATION
EPINEPHRINE injection, USP
1:1000 (1 mg/mL)
Ampul
Protect from light until ready to use.
Rx only
DescriptionEpinephrine Injection, USP 1:1000 is a sterile, nonpyrogenic solution.
Each mL contains epinephrine 1 mg; sodium chloride 9 mg; sodium
metabisulfite 0.9 mg added. May contain
hydrochloric acid for pH
adjustment. The solution contains no bacteriostat or antimicrobial
agent. It is administered by the following routes: intravenous,
intracardiac (left ventricular chamber), via endotracheal tube into the
bronchial tree, subcutaneous or intramuscular. Epinephrine, USP is a
sympathomimetic (adrenergic) agent designated chemically as
4-[1-hydroxy-2 (methylamino) ethyl]-1,2 benzenediol, a white,
microcrystalline powder. It has the following structural formula:
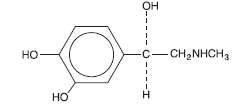
Sodium Chloride, USP is chemically designated NaCl, a white, crystalline compound freely soluble in water.
Clinical PharmacologyThe actions of epinephrine resemble the effects of
stimulation of adrenergic nerves. To a variable degree it acts on both
alpha and beta receptor sites of sympathetic effector cells. Its most
prominent actions are on the beta receptors of the heart, vascular and
other smooth muscle. When given by rapid intravenous injection, it
produces a rapid rise in blood pressure, mainly systolic, by (1) direct
stimulation of cardiac muscle which increases the strength of
ventricular contraction, (2) increasing the heart rate and (3)
constriction of the arterioles in the skin, mucosa and splanchnic areas
of the circulation. When given by slow intravenous injection epinephrine
usually produces only a moderate rise in systolic and a fall in
diastolic pressure. Although some increase in pulse pressure occurs,
there is usually no great elevation in mean blood pressure. Accordingly,
the compensatory reflex mechanisms that come into play with a
pronounced increase in blood pressure do not antagonize the direct
cardiac actions of epinephrine as much as with catecholamines that have a
predominant action on alpha receptors.
Total peripheral resistance
decreases by action of epinephrine on beta receptors of the skeletal
muscle vasculature and blood flow is thereby enhanced. Usually this
vasodilator effect of the drug on the circulation predominates so that
the modest rise in systolic pressure which follows slow injection or
absorption is mainly the result of direct cardiac stimulation and
increase in cardiac output. In some instances peripheral resistance is
not altered or may even rise owing to a greater ratio of alpha to beta
activity in different vascular areas. Epinephrine relaxes the smooth
muscles of the bronchi and iris and is a physiologic antagonist of
histamine. The drug also produces an increase in blood sugar and
glycogenolysis in the liver. Intravenous injection produces an immediate
and intensified response. Following intravenous injection epinephrine
disappears rapidly from the blood stream. Epinephrine is rapidly
inactivated in the body and is degraded by enzymes in the liver and
other tissues. The large portion of injection doses is excreted in the
urine as inactivated compounds. The remainder is excreted in the urine
as unchanged or conjugated compounds.
Uses
Indications and UsageEpinephrine is used to relieve respiratory distress due to bronchospasm, to provide rapid relief of hypersensitivity reactions to drugs and other allergens, and to prolong the action of anesthetics. Its cardiac effects may be of use in restoring cardiac rhythm in cardiac arrest due to various causes, but it is not used in cardiac failure or in hemorrhagic, traumatic, or cardiogenic shock. Epinephrine is used as a hemostatic agent. It is also used in treating mucosal congestion of hay fever, rhinitis, and acute sinusitis; to relieve bronchial asthmatic paroxysms; in syncope due to complete heart block or carotid sinus hypersensitivity; for symptomatic relief of serum sickness, urticaria, angioneurotic edema; for resuscitation in cardiac arrest following anesthetic accidents; in simple (open angle) glaucoma; for relaxation of uterine musculature and to inhibit uterine contractions. Epinephrine Injection can be utilized to prolong the action of anesthetics used in local and regional anesthesia.
ContraindicationsEpinephrine is contraindicated in patients with known
hypersensitivity to sympathomimetic amines, in patients with angle
closure glaucoma, and patients in shock (nonanaphylactic). It should
not
be used in patients anesthetized with agents such as cyclopropane or
halothane as these may sensitize the heart to the arrhythmic action of
sympathomimetic drugs. Addition of epinephrine to local anesthetics for
injection of certain areas (e.g., fingers, toes, ears, etc.) is
contraindicated because of danger that vasoconstriction may result in
sloughing of tissue.
Except as diluted for admixture with local
anesthetics to reduce absorption and prolong action, epinephrine should
not ordinarily be used in those cases where vasopressor drugs may be
contraindicated,
e.g., in thyrotoxicosis, diabetes, in obstetrics when maternal blood
pressure is in excess of 130/80 and in hypertension and other
cardiovascular disorders.
Inadvertently induced high arterial blood pressure may result in angina pectoris, aortic rupture or cerebral hemorrhage. Epinephrine may induce potentially serious cardiac arrhythmias in patients not suffering from heart disease and in patients with organic heart disease or who are receiving drugs that sensitize the myocardium. Parenterally administered epinephrine initially may produce constriction of renal blood vessels and decrease urine formation. Epinephrine Injection, USP is subject to oxidation and should be protected against exposure to light and stored in light-resistant containers. Epinephrine is the preferred treatment for serious allergic or other emergency situations even though this product contains sodium metabisulfite, a sulfite that may in other products cause allergic-type reactions including anaphylactic symptoms or life-threatening or less severe asthmatic episodes in certain susceptible persons. The alternatives to using epinephrine in a life-threatening situation may not be satisfactory. The presence of a sulfite in this product should not deter administration of the drug for treatment of serious allergic or other emergency situations.
PrecautionsDo not use the Injection if its color is pinkish or
darker than slightly yellow or if it contains a precipitate. Do not
administer unless solution is clear and container is intact. Discard
unused portion. Although epinephrine can produce ventricular
fibrillation, its actions in restoring electrical activity in asystole
and in enhancing defibrillation of the fibrillating ventricle are well
documented. The drug, however, should be used with caution in patients
with ventricular fibrillation. Epinephrine should be used cautiously in
patients with hyperthyroidism, hypertension and
cardiac arrhythmias.
All vasopressors should be used cautiously in patients taking monoamine
oxidase (MAO) inhibitors. Epinephrine should not be administered
concomitantly with other sympathomimetic drugs (such as isoproterenol)
because of possible additive effects and increased toxicity. Combined
effects may induce serious cardiac arrhythmias. They may be administered
alternately when the preceding effect of other such drugs has subsided.
Administration of epinephrine to patients receiving cyclopropane or
halogenated hydrocarbon general anesthetics such as halothane which
sensitize the myocardium, may induce cardiac arrhythmia. (See
CONTRAINDICATIONS.) When encountered, such arrhythmias may respond to
administration of a beta-adrenergic blocking drug. Epinephrine also
should be used cautiously with other drugs (e.g., digitalis glycosides)
that sensitize the myocardium to the actions of
sympathomimetic
agents. Diuretic agents may decrease vascular response to pressor drugs
such as epinephrine. Epinephrine may antagonize the neuron blockade
produced by guanethidine resulting in decreased antihypertensive effect
and requiring increased dosage of the latter.
Pregnancy Category C. Animal reproduction
studies have not been conducted with epinephrine. It is also not known
whether epinephrine can cause fetal harm when administered to a
pregnant woman or can affect reproduction capacity. Epinephrine should be given to a pregnant woman only if clearly needed.
Labor and Delivery. Parenteral
administration of epinephrine if used to support blood pressure during
low or other spinal anesthesia for delivery can cause acceleration of
fetal heart rate and
should not be used in obstetrics when maternal blood pressure exceeds 130/80. (See CONTRAINDICATIONS.)
Transient and minor side effects of anxiety, headache, fear and palpitations occur only with systemic therapeutic doses, especially in hyperthyroid individuals. Adverse effects such as cardiac arrhythmias and excessive rise in blood pressure may occur with systemic therapeutic doses or with inadvertent overdosage. Other adverse reactions include cerebral hemorrhage, hemiplegia, subarachnoid hemorrhage, anginal pain in patients with angina pectoris, anxiety, restlessness, headache, tremor, weakness, dizziness, pallor and respiratory difficulty. Such reactions are unlikely when epinephrine is diluted to 1:200,000 for injection with local anesthetic agents.
OverdosageErroneous administration of large doses of epinephrine may lead to precordial distress, vomiting, headache, dyspnea, as well as unusually elevated blood pressure. (See WARNINGS.) Toxic effects of overdosage can be counteracted by injection of an alpha-adrenergic blocker and a betaadrenergic blocker. In the event of a sharp rise in blood pressure, rapid-acting vasodilators such as the nitrites, or alpha-adrenergic blocking agents can be given to counteract the marked pressor effect of large doses of epinephrine.
Dosage and AdministrationSubcutaneously or intramuscularly – 0.2 to 1 mL (mg). Start with a small dose and increase if required.
Note: The subcutaneous is the preferred route
of administration. If given intramuscularly, injection into the buttocks
should be avoided.
Hypersensitivity Reactions
For bronchial asthma and certain allergic manifestations, e.g.,
angioedema, urticaria, serum sickness, anaphylactic shock, use
epinephrine subcutaneously. The adult intravenous dose for
hypersensitivity
reactions or to relieve bronchospasm usually ranges from 0.1 to 0.25 mg
injected slowly. Neonates may be given a dose of 0.01 mg per kg of body
weight; for the infant 0.05 mg is an adequate initial dose and this may
be repeated at 20 to 30 minute intervals in the management of asthma
attacks.
Cardiac Resuscitation
A dose of 0.5 mL (0.5 mg) diluted to 10 mL with sodium chloride
injection can be administered intravenously or intracardially to restore
myocardial contractility. Intracardiac injection should only be
administered by personnel well trained in the technique, if there has
not been sufficient time to establish an intravenous route. External
cardiac massage should follow intracardial administration to permit the
drug to enter coronary circulation. The drug should be used secondarily
to unsuccessful attempts with physical or electromechanical methods.
Ophthalmologic Use
Ophthalmologic use (for producing conjunctival decongestion, to
control hemorrhage, produce mydriasis and reduce intraocular pressure) –
use a concentration of 1:10,000 (0.1 mg/mL) to
1:1000 (1 mg/mL).
Regional Anesthesia
A final concentration of 1:200,000 of epinephrine injection is
recommended for infiltration injection, nerve block, caudal or other
epidural blocks. From 0.3 to 0.4 mg of epinephrine (0.3 to
0.4 mL of
1:1000 solution) may be mixed with spinal anesthetic agents. Parenteral
drug products should be inspected visually for particulate matter and
discoloration prior to administration. (See PRECAUTIONS.)
Epinephrine Pack Label

LIDOCAINE HYDROCHLORIDE (lidocaine hydrochloride anhydrous) injection, solution
AQUEOUS SOLUTIONS FOR INFILTRATION
AND NERVE BLOCK
Ampul
Plastic Multiple-dose Fliptop Vial
Glass Teartop Vial
Rx only
DESCRIPTIONLidocaine Hydrochloride Injection, USP is a sterile, nonpyrogenic solution of lidocaine hydrochloride in water for injection for parenteral administration in various concentrations with characteristics as follows:
|
Concentration |
0.5% |
1% |
1.5% |
2% |
|
mg/mL lidocaine HCl (anhyd.) |
5 |
10 |
15 |
20 |
|
mg/mL sodium chloride |
8 |
7 |
6.5 |
6 |
Multiple-dose vials contain 0.1% of methylparaben added as preservative. May contain sodium hydroxide and/or hydrochloric acid for pH adjustment. The pH is 6.5 (5.0 to 7.0). See HOW SUPPLIED section for various sizes and strengths.
Lidocaine is a local anesthetic of the amide type.
Lidocaine Hydrochloride, USP is chemically designated 2-(diethylamino)-N-(2,6-dimethylphenyl)-acetamide monohydrochloride monohydrate, a white powder freely soluble in water. The molecular weight is 288.82. It has the following structural formula:

The semi-rigid vial used for the plastic vials is fabricated from a specially formulated polyolefin. It is a copolymer of ethylene and propylene. The safety of the plastic has been confirmed by tests in animals according to USP biological standards for plastic containers. The container requires no vapor barrier to maintain the proper drug concentration.
CLINICAL PHARMACOLOGYMechanism of action: Lidocaine stabilizes the neuronal membrane by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.
Hemodynamics: Excessive blood levels may cause changes in cardiac output, total peripheral resistance, and mean arterial pressure. With central neural blockade these changes may be attributable to block of autonomic fibers, a direct depressant effect of the local anesthetic agent on various components of the cardiovascular system and/or the beta-adrenergic receptor stimulating action of epinephrine when present. The net effect is normally a modest hypotension when the recommended dosages are not exceeded.
Pharmacokinetics and metabolism: Information derived from diverse formulations, concentrations and usages reveals that lidocaine is completely absorbed following parenteral administration, its rate of absorption depending, for example, upon various factors such as the site of administration and the presence or absence of a vasoconstrictor agent. Except for intravascular administration, the highest blood levels are obtained following intercostal nerve block and the lowest after subcutaneous administration.
The plasma binding of lidocaine is dependent on drug concentration, and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 mcg of free base per mL, 60 to 80 percent of lidocaine is protein bound. Binding is also dependent on the plasma concentration of the alpha-1-acid glycoprotein.
Lidocaine crosses the blood-brain and placental barriers, presumably by passive diffusion.
Lidocaine is metabolized rapidly by the liver, and metabolites and unchanged drug are excreted by the kidneys. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage, and conjugation. N-dealkylation, a major pathway of biotransformation, yields the metabolites monoethylglycinexylidide and glycinexylidide. The pharmacological/toxicological actions of these metabolites are similar to, but less potent than, those of lidocaine. Approximately 90% of lidocaine administered is excreted in the form of various metabolites, and less than 10% is excreted unchanged. The primary metabolite in urine is a conjugate of 4-hydroxy-2, 6-dimethylaniline.
The elimination half-life of lidocaine following an intravenous bolus injection is typically 1.5 to 2.0 hours. Because of the rapid rate at which lidocaine is metabolized, any condition that affects liver function may alter lidocaine kinetics. The half-life may be prolonged two-fold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine kinetics but may increase the accumulation of metabolites.
Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6.0 mcg free base per mL. In the rhesus monkey arterial blood levels of 18-21 mcg/mL have been shown to be threshold for convulsive activity.
Uses
INDICATIONS AND USAGELidocaine Hydrochloride Injection, USP is indicated for production of local or regional anesthesia by infiltration techniques such as percutaneous injection and intravenous regional anesthesia by peripheral nerve block techniques such as brachial plexus and intercostal and by central neural techniques such as lumbar and caudal epidural blocks, when the accepted procedures for these techniques as described in standard textbooks are observed.
CONTRAINDICATIONSLidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type.
WARNINGSLIDOCAINE HYDROCHLORIDE INJECTION, FOR INFILTRATION AND NERVE BLOCK, SHOULD BE EMPLOYED ONLY BY CLINICIANS WHO ARE WELL VERSED IN DIAGNOSIS AND MANAGEMENT OF DOSE-RELATED TOXICITY AND OTHER ACUTE EMERGENCIES THAT MIGHT ARISE FROM THE BLOCK TO BE EMPLOYED AND THEN ONLY AFTER ENSURING THE IMMEDIATE AVAILABILITY OF OXYGEN, OTHER RESUSCITATIVE DRUGS, CARDIOPULMONARY EQUIPMENT, AND THE PERSONNEL NEEDED FOR PROPER MANAGEMENT OF TOXIC REACTIONS AND RELATED EMERGENCIES (See also ADVERSE REACTIONS and PRECAUTIONS ). DELAY IN PROPER MANAGEMENT OF DOSE-RELATED TOXICITY, UNDERVENTILATION FROM ANY CAUSE AND/OR ALTERED SENSITIVITY MAY LEAD TO THE DEVELOPMENT OF ACIDOSIS, CARDIAC ARREST AND, POSSIBLY, DEATH.
Intra-articular infusions of local anesthetics following arthroscopic and other surgical procedures is an unapproved use, and there have been post-marketing reports of chondrolysis in patients receiving such infusions. The majority of reported cases of chondrolysis have involved the shoulder joint; cases of gleno-humeral chondrolysis have been described in pediatric and adult patients following intra-articular infusions of local anesthetics with and without epinephrine for periods of 48 to 72 hours. There is insufficient information to determine whether shorter infusion periods are not associated with these findings. The time of onset of symptoms, such as joint pain, stiffness and loss of motion can be variable, but may begin as early as the 2nd month after surgery. Currently, there is no effective treatment for chondrolysis; patients who experienced chondrolysis have required additional diagnostic and therapeutic procedures and some required arthroplasty or shoulder replacement.
To avoid intravascular injection, aspiration should be performed before the local anesthetic solution is injected. The needle must be repositioned until no return of blood can be elicited by aspiration. Note, however, that the absence of blood in the syringe does not guarantee that intravascular injection has been avoided.
Local anesthetic solutions containing antimicrobial preservatives (e.g., methylparaben) should not be used for epidural or spinal anesthesia because the safety of these agents has not been established with regard to intrathecal injection, either intentional or accidental.
PRECAUTIONSGeneral:The safety and effectiveness of lidocaine depend on proper dosage, correct technique, adequate precautions, and readiness for emergencies. Standard textbooks should be consulted for specific techniques and precautions for various regional anesthetic procedures.
Resuscitative equipment, oxygen, and other resuscitative drugs should be available for immediate use. (See WARNINGS and ADVERSE REACTIONS ). The lowest dosage that results in effective anesthesia should be used to avoid high plasma levels and serious adverse effects. Syringe aspirations should also be performed before and during each supplemental injection when using indwelling catheter techniques. During the administration of epidural anesthesia, it is recommended that a test dose be administered initially and that the patient be monitored for central nervous system toxicity and cardiovascular toxicity, as well as for signs of unintended intrathecal administration before proceeding. When clinical conditions permit, consideration should be given to employing local anesthetic solutions that contain epinephrine for the test dose because circulatory changes compatible with epinephrine may also serve as a warning sign of unintended intravascular injection. An intravascular injection is still possible even if aspirations for blood are negative. Repeated doses of lidocaine may cause significant increases in blood levels with each repeated dose because of slow accumulation of the drug or its metabolites. Tolerance to elevated blood levels varies with the status of the patient. Debilitated, elderly patients, acutely ill patients and children should be given reduced doses commensurate with their age and physical condition. Lidocaine should also be used with caution in patients with severe shock or heart block. Lumbar and caudal epidural anesthesia should be used with extreme caution in persons with the following conditions: existing neurological disease, spinal deformities, septicemia and severe hypertension.
Local anesthetic solutions containing a vasoconstrictor should be used cautiously and in carefully circumscribed quantities in areas of the body supplied by end arteries or having otherwise compromised blood supply. Patients with peripheral vascular disease and those with hypertensive vascular disease may exhibit exaggerated vasoconstrictor response. Ischemic injury or necrosis may result. Preparations containing a vasoconstrictor should be used with caution in patients during or following the administration of potent general anesthetic agents, since cardiac arrhythmias may occur under such conditions.
Careful and constant monitoring of cardiovascular and respiratory (adequacy of ventilation) vital signs and the patient’s state of consciousness should be accomplished after each local anesthetic injection. It should be kept in mind at such times that restlessness, anxiety, tinnitus, dizziness, blurred vision, tremors, depression or drowsiness may be early warning signs of central nervous system toxicity.
Since amide-type local anesthetics are metabolized by the liver, lidocaine should be used with caution in patients with hepatic disease. Patients with severe hepatic disease, because of their inability to metabolize local anesthetics normally, are at greater risk of developing toxic plasma concentrations. Lidocaine should also be used with caution in patients with impaired cardiovascular function since they may be less able to compensate for functional changes associated with the prolongation of A-V conduction produced by these drugs. Many drugs used during the conduct of anesthesia are considered potential triggering agents for familial malignant hyperthermia. Since it is not known whether amide-type local anesthetics may trigger this reaction and since the need for supplemental general anesthesia cannot be predicted in advance, it is suggested that a standard protocol for the management of malignant hyperthermia should be available. Early unexplained signs of tachycardia, tachypnea, labile blood pressure and metabolic acidosis may precede temperature elevation. Successful outcome is dependent on early diagnosis, prompt discontinuance of the suspect triggering agent(s) and institution of treatment, including oxygen therapy, indicated supportive measures and dantrolene (consult dantrolene sodium intravenous package insert before using).
Proper tourniquet technique, as described in publications and standard textbooks, is essential in the performance of intravenous regional anesthesia. Solutions containing epinephrine or other vasoconstrictors should not be used for this technique.
Lidocaine should be used with caution in persons with known drug sensitivities. Patients allergic to para-aminobenzoic acid derivatives (procaine, tetracaine, benzocaine, etc.) have not shown cross sensitivity to lidocaine.
Use in the Head and Neck Area: Small doses of local anesthetics injected into the head and neck area, including retrobulbar, dental and stellate ganglion blocks, may produce adverse reactions similar to systemic toxicity seen with unintentional intravascular injections of larger doses. Confusion, convulsions, respiratory depression and/or respiratory arrest and cardiovascular stimulation or depression have been reported. These reactions may be due to intra-arterial injections of the local anesthetic with retrograde flow to the cerebral circulation. Patients receiving these blocks should have their circulation and respiration monitored and be constantly observed. Resuscitative equipment and personnel for treating adverse reactions should be immediately available. Dosage recommendations should not be exceeded. (See DOSAGE AND ADMINISTRATION ).
When appropriate, patients should be informed in advance that they may experience temporary loss of sensation and motor activity, usually in the lower half of the body following proper administration of epidural anesthesia.
The administration of local anesthetic solutions containing epinephrine or norepinephrine to patients receiving monoamine oxidase inhibitors or tricyclic antidepressants may produce severe prolonged hypertension.
Phenothiazines and butyrophenones may reduce or reverse the pressor effect of epinephrine.
Concurrent use of these agents should generally be avoided. In situations when concurrent therapy is necessary, careful patient monitoring is essential.
Concurrent administration of vasopressor drugs (for the treatment of hypotension related to obstetric blocks) and ergot-type oxytoxic drugs may cause severe persistent hypertension or cerebrovascular accidents.
The intramuscular injection of lidocaine may result in an increase in creatine phosphokinase levels. Thus, the use of this enzyme determination without isoenzyme separation as a diagnostic test for the presence of acute myocardial infarction may be compromised by the intramuscular injection of lidocaine.
Studies of lidocaine in animals to evaluate the carcinogenic and mutagenic potential or the effect on fertility have not been conducted.
Teratogenic Effects. Pregnancy Category B. Reproduction studies have been performed in rats at doses up to 6.6 times the human dose and have revealed no evidence of harm to the fetus caused by lidocaine. There are, however, no adequate and well-controlled studies in pregnant women. Animal reproduction studies are not always predictive of human response. General consideration should be given to this fact before administering lidocaine to women of childbearing potential, especially during early pregnancy when maximum organogenesis takes place.
Local anesthetics rapidly cross the placenta and when used for epidural, paracervical, pudendal or caudal block anesthesia, can cause varying degrees of maternal, fetal and neonatal toxicity (See CLINICAL PHARMACOLOGY — Pharmacokinetics ). The potential for toxicity depends upon the procedure performed, the type and amount of drug used, and the technique of drug administration. Adverse reactions in the parturient, fetus and neonate involve alterations of the central nervous system peripheral vascular tone and cardiac function.
Maternal hypotension has resulted from regional anesthesia. Local anesthetics produce vasodilation by blocking sympathetic nerves. Elevating the patient’s legs and positioning her on her left side will help prevent decreases in blood pressure. The fetal heart rate also should be monitored continuously, and electronic fetal monitoring is highly advisable.
Epidural, spinal, paracervical, or pudendal anesthesia may alter the forces of parturition through changes in uterine contractility or maternal expulsive efforts. In one study, paracervical block anesthesia was associated with a decrease in the mean duration of first stage labor and facilitation of cervical dilation. However, spinal and epidural anesthesia have also been reported to prolong the second stage of labor by removing the parturient’s reflex urge to bear down or by interfering with motor function. The use of obstetrical anesthesia may increase the need for forceps assistance.
The use of some local anesthetic drug products during labor and delivery may be followed by diminished muscle strength and tone for the first day or two of life. The long-term significance of these observations is unknown. Fetal bradycardia may occur in 20 to 30 percent of patients receiving paracervical nerve block anesthesia with the amide-type local anesthetics and may be associated with fetal acidosis. Fetal heart rate should always be monitored during paracervical anesthesia. The physician should weigh the possible advantages against risks when considering paracervical block in prematurity, toxemia of pregnancy and fetal distress. Careful adherence to recommended dosage is of the utmost importance in obstetrical paracervical block. Failure to achieve adequate analgesia with recommended doses should arouse suspicion of intravascular or fetal intracranial injection. Cases compatible with unintended fetal intracranial injection of local anesthetic solution have been reported following intended paracervical or pudendal block or both. Babies so affected present with unexplained neonatal depression at birth, which correlates with high local anesthetic serum levels, and often manifest seizures within six hours. Prompt use of supportive measures combined with forced urinary excretion of the local anesthetic has been used successfully to manage this complication.
Case reports of maternal convulsions and cardiovascular collapse following use of some local anesthetics for paracervical block in early pregnancy (as anesthesia for elective abortion) suggest that systemic absorption under these circumstances may be rapid. The recommended maximum dose of each drug should not be exceeded. Injection should be made slowly and with frequent aspiration. Allow a 5-minute interval between sides.
It is not known whether this drug is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when lidocaine is administered to a nursing woman.
Dosages in pediatric patients should be reduced, commensurate with age, body weight and physical condition. See DOSAGE AND ADMINISTRATION .
ADVERSE REACTIONSSystemic: Adverse experiences following the administration of lidocaine are similar in nature to those observed with other amide local anesthetic agents. These adverse experiences are, in general, dose-related and may result from high plasma levels caused by excessive dosage, rapid absorption or inadvertent intravascular injection, or may result from a hypersensitivity, idiosyncrasy or diminished tolerance on the part of the patient. Serious adverse experiences are generally systemic in nature. The following types are those most commonly reported:
Central Nervous System: CNS manifestations are excitatory and/or depressant and may be characterized by lightheadedness, nervousness, apprehension, euphoria, confusion, dizziness, drowsiness, tinnitus, blurred or double vision, vomiting, sensations of heat, cold or numbness, twitching, tremors, convulsions, unconsciousness, respiratory depression and arrest. The excitatory manifestations may be very brief or may not occur at all, in which case the first manifestation of toxicity may be drowsiness merging into unconsciousness and respiratory arrest.
Drowsiness following the administration of lidocaine is usually an early sign of a high blood level of the drug and may occur as a consequence of rapid absorption.
Cardiovascular System: Cardiovascular manifestations are usually depressant and are characterized by bradycardia, hypotension, and cardiovascular collapse, which may lead to cardiac arrest.
Allergic: Allergic reactions are characterized by cutaneous lesions, urticaria, edema or anaphylactoid reactions. Allergic reactions may occur as a result of sensitivity either to local anesthetic agents or to the methylparaben used as a preservative in multiple dose vials. Allergic reactions as a result of sensitivity to lidocaine are extremely rare and, if they occur, should be managed by conventional means. The detection of sensitivity by skin testing is of doubtful value.
Neurologic: The incidences of adverse reactions associated with the use of local anesthetics may be related to the total dose of local anesthetic administered and are also dependent upon the particular drug used, the route of administration and the physical status of the patient. In a prospective review of 10,440 patients who received lidocaine for spinal anesthesia, the incidences of adverse reactions were reported to be about 3 percent each for positional headaches, hypotension and backache; 2 percent for shivering; and less than 1 percent each for peripheral nerve symptoms, nausea, respiratory inadequacy and double vision. Many of these observations may be related to local anesthetic techniques, with or without a contribution from the local anesthetic.
In the practice of caudal or lumbar epidural block, occasional unintentional penetration of the subarachnoid space by the catheter may occur. Subsequent adverse effects may depend partially on the amount of drug administered subdurally.
These may include spinal block of varying magnitude (including total spinal block), hypotension secondary to spinal block, loss of bladder and bowel control, and loss of perineal sensation and sexual function. Persistent motor, sensory and/or autonomic (sphincter control) deficit of some lower spinal segments with slow recovery (several months) or incomplete recovery have been reported in rare instances when caudal or lumbar epidural block has been attempted. Backache and headache have also been noted following use of these anesthetic procedures.
There have been reported cases of permanent injury to extraocular muscles requiring surgical repair following retrobulbar administration.
OVERDOSAGEAcute emergencies from local anesthetics are generally related to high plasma levels encountered during therapeutic use of local anesthetics or to unintended subarachnoid injection of local anesthetic solution (see ADVERSE REACTIONS, WARNINGS and PRECAUTIONS ).
Management of Local Anesthetic Emergencies: The first consideration is prevention, best accomplished by careful monitoring of cardiovascular and respiratory vital signs and the patient’s state of consciousness after each local anesthetic injection. At the first sign of change, oxygen should be administered.
The first step in the management of convulsions, as well as underventilation or apnea due to unintended subarachnoid injection of drug solution, consists of immediate attention to the maintenance of a patent airway and assisted or controlled ventilation with oxygen and a delivery system capable of permitting immediate positive airway pressure by mask. Immediately after the institution of these ventilatory measures, the adequacy of the circulation should be evaluated, keeping in mind that drugs used to treat convulsions sometimes depress the circulation when administered intravenously. Should convulsions persist despite adequate respiratory support, and if the status of the circulation permits, small increments of an ultra-short acting barbiturate (such as thiopental or thiamylal) or a benzodiazepine (such as diazepam) may be administered intravenously. The clinician should be familiar, prior to use of local anesthetics, with these anticonvulsant drugs. Supportive treatment of circulatory depression may require administration of intravenous fluids and, when appropriate, a vasopressor as directed by the clinical situation (e.g., ephedrine).
If not treated immediately, both convulsions and cardiovascular depression can result in hypoxia, acidosis, bradycardia, arrhythmias and cardiac arrest. Underventilation or apnea due to unintentional subarachnoid injection of local anesthetic solution may produce these same signs and also lead to cardiac arrest if ventilatory support is not instituted. If cardiac arrest should occur standard cardiopulmonary resuscitative measures should be instituted.
Endotracheal intubation, employing drugs and techniques familiar to the clinician, may be indicated, after initial administration of oxygen by mask, if difficulty is encountered in the maintenance of a patent airway or if prolonged ventilatory support (assisted or controlled) is indicated.
Dialysis is of negligible value in the treatment of acute overdosage with lidocaine.
The oral LD50 of lidocaine HCl in non-fasted female rats is 459 (346−773) mg/kg (as the salt) and 214 (159−324) mg/kg (as the salt) in fasted female rats.
DOSAGE AND ADMINISTRATIONTable 1 (Recommended Dosages) summarizes the recommended volumes and concentrations of Lidocaine Hydrochloride Injection, USP for various types of anesthetic procedures. The dosages suggested in this table are for normal healthy adults and refer to the use of epinephrine-free solutions. When larger volumes are required only solutions containing epinephrine should be used, except in those cases where vasopressor drugs may be contraindicated.
There have been adverse event reports of chondrolysis in patients receiving intra-articular infusions of local anesthetics following arthroscopic and other surgical procedures. Lidocaine is not approved for this use (see WARNINGS and DOSAGE AND ADMINISTRATION ).
These recommended doses serve only as a guide to the amount of anesthetic required for most routine procedures. The actual volumes and concentrations to be used depend on a number of factors such as type and extent of surgical procedure, depth of anesthesia and degree of muscular relaxation required, duration of anesthesia required, and the physical condition of the patient. In all cases the lowest concentration and smallest dose that will produce the desired result should be given. Dosages should be reduced for children and for elderly and debilitated patients and patients with cardiac and/or liver disease.
The onset of anesthesia, the duration of anesthesia and the degree of muscular relaxation are proportional to the volume and concentration (i.e., total dose) of local anesthetic used. Thus, an increase in volume and concentration of Lidocaine Hydrochloride Injection will decrease the onset of anesthesia, prolong the duration of anesthesia, provide a greater degree of muscular relaxation and increase the segmental spread of anesthesia. However, increasing the volume and concentration of Lidocaine Hydrochloride Injection may result in a more profound fall in blood pressure when used in epidural anesthesia. Although the incidence of side effects with lidocaine is quite low, caution should be exercised when employing large volumes and concentrations, since the incidence of side effects is directly proportional to the total dose of local anesthetic agent injected.
For intravenous regional anesthesia, only the 50 mL single-dose vial containing 0.5% Lidocaine Hydrochloride Injection, USP should be used.
Epidural Anesthesia
For epidural anesthesia, only the following available specific products of Lidocaine Hydrochloride Injection by Hospira are recommended:
1%. . . . . . . . . . . . . . . . . . . . 30 mL single-dose teartop vials
1.5%. . . . . . . . . . . . . . . . . . . . . . . 20 mL single-dose ampuls
2%. . . . . . . . . . . . . . . . . . . . . . . . . 10 mL single-dose ampuls
Although these solutions are intended specifically for epidural anesthesia, they may also be used for infiltration and peripheral nerve block provided they are employed as single dose units. These solutions contain no bacteriostatic agent. In epidural anesthesia, the dosage varies with the number of dermatomes to be anesthetized (generally 2−3 mL of the indicated concentration per dermatome).
Caudal and Lumbar Epidural Block: As a precaution against the adverse experiences sometimes observed following unintentional penetration of the subarachnoid space, a test dose such as 2−3 mL of 1.5% lidocaine hydrochloride should be administered at least 5 minutes prior to injecting the total volume required for a lumbar or caudal epidural block. The test dose should be repeated if the patient is moved in a manner that may have displaced the catheter. Epinephrine, if contained in the test dose (10−15 mcg have been suggested), may serve as a warning of unintentional intravascular injection. If injected into a blood vessel, this amount of epinephrine is likely to produce a transient "epinephrine response" within 45 seconds, consisting of an increase in heart rate and systolic blood pressure, circumoral pallor, palpitations and nervousness in the unsedated patient. The sedated patient may exhibit only a pulse rate increase of 20 or more beats per minute for 15 or more seconds. Patients on beta-blockers may not manifest changes in heart rate, but blood pressure monitoring can detect an evanescent rise in systolic blood pressure. Adequate time should be allowed for onset of anesthesia after administration of each test dose. The rapid injection of a large volume of Lidocaine Hydrochloride Injection through the catheter should be avoided, and, when feasible, fractional doses should be administered.
In the event of the known injection of a large volume of local anesthetic solutions into the subarachnoid space, after suitable resuscitation and if the catheter is in place, consider attempting the recovery of drug by draining a moderate amount of cerebrospinal fluid (such as 10 mL) through the epidural catheter.
Maximum Recommended Dosages
NOTE: The products accompanying this insert do not contain epinephrine.
Adults: For normal healthy adults, the individual maximum recommended dose of lidocaine HCl with epinephrine should not exceed 7 mg/kg (3.5 mg/lb) of body weight and in general it is recommended that the maximum total dose not exceed 500 mg. When used without epinephrine, the maximum individual dose should not exceed 4.5 mg/kg (2 mg/lb) of body weight and in general it is recommended that the maximum total dose does not exceed 300 mg. For continuous epidural or caudal anesthesia, the maximum recommended dosage should not be administered at intervals of less than 90 minutes. When continuous lumbar or caudal epidural anesthesia is used for non-obstetrical procedures, more drug may be administered if required to produce adequate anesthesia.
The maximum recommended dose per 90 minute period of lidocaine hydrochloride for paracervical block in obstetrical patients and non-obstetrical patients is 200 mg total. One-half of the total dose is usually administered to each side. Inject slowly five minutes between sides. (See also discussion of paracervical block in PRECAUTIONS ).
For intravenous regional anesthesia, the dose administered should not exceed 4 mg/kg in adults.
Children: It is difficult to recommend a maximum dose of any drug for children, since this varies as a function of age and weight. For children over 3 years of age who have a normal lean body mass and normal body development, the maximum dose is determined by the child’s age and weight. For example, in a child of 5 years weighing 50 lbs., the dose of lidocaine HCl should not exceed 75 — 100 mg (1.5 — 2 mg/lb). The use of even more dilute solutions (i.e., 0.25 — 0.5%) and total dosages not to exceed 3 mg/kg (1.4 mg/lb) are recommended for induction of intravenous regional anesthesia in children.
In order to guard against systemic toxicity, the lowest effective concentration and lowest effective dose should be used at all times. In some cases it will be necessary to dilute available concentrations with 0.9% sodium chloride injection in order to obtain the required final concentration.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration whenever the solution and container permit. Solutions that are discolored and/or contain particulate matter should not be used.
|
Table 1 |
|||
|
Recommended Dosages of Lidocaine Hydrochloride Injection, USP for Various Anesthetic |
|||
|
Procedures in Normal Healthy Adults |
|||
|
|
|
||
|
|
Lidocaine Hydrochloride Injection, USP (without Epinephrine) |
||
|
|
|
|
|
|
Procedure |
Conc. (%) |
Vol. (mL) |
Total Dose (mg) |
|
|
|
|
|
|
Infiltration |
|
|
|
|
Percutaneous |
0.5 or 1.0 |
1−60 |
5−300 |
|
Intravenous Regional |
0.5 |
10−60 |
50−300 |
|
|
|
|
|
|
Peripheral Nerve Blocks, e.g. |
|
|
|
|
Brachial |
1.5 |
15−20 |
225−300 |
|
Dental |
2.0 |
1−5 |
20−100 |
|
Intercostal |
1.0 |
3 |
30 |
|
Paravertebral |
1.0 |
3−5 |
30−50 |
|
Pudendal (each side) |
1.0 |
10 |
100 |
|
Paracervical |
|
|
|
|
Obstetrical Analgesia |
|
|
|
|
(each side) |
1.0 |
10 |
100 |
|
|
|
|
|
|
Sympathetic Nerve Blocks, e.g. |
|
|
|
|
Cervical (stellate ganglion) |
1.0 |
5 |
50 |
|
Lumbar |
1.0 |
5−10 |
50−100 |
|
|
|
|
|
|
Central Neural Blocks |
|
|
|
|
Epidural* |
|
|
|
|
Thoracic |
1.0 |
20−30 |
200−300 |
|
Lumbar |
|
|
|
|
Analgesia |
1.0 |
25−30 |
250−300 |
|
Anesthesia |
1.5 |
15−20 |
225−300 |
|
|
2.0 |
10−15 |
200−300 |
|
Caudal |
|
|
|
|
Obstetrical Analgesia |
1.0 |
20−30 |
200−300 |
|
Surgical Anesthesia |
1.5 |
15−20 |
225−300 |
|
|
|
|
|
|
|
|||
|
*Dose determined by number of dermatomes to be anesthetized (2 to 3 mL/dermatome). |
THE ABOVE SUGGESTED CONCENTRATIONS AND VOLUMES SERVE ONLY AS A GUIDE. OTHER VOLUMES AND CONCENTRATIONS MAY BE USED PROVIDED THE TOTAL MAXIMUM RECOMMENDED DOSE IS NOT EXCEEDED.
Sterilization, Storage and Technical Procedures: Disinfecting agents containing heavy metals, which cause release of respective ions (mercury, zinc, copper, etc.) should not be used for skin or mucous membrane disinfection as they have been related to incidence of swelling and edema. When chemical disinfection of multi-dose vials is desired, either isopropyl alcohol (91%) or 70% ethyl alcohol is recommended. Many commercially available brands of rubbing alcohol, as well as solutions of ethyl alcohol not of USP grade, contain denaturants which are injurious to rubber and, therefore, are not to be used. It is recommended that chemical disinfection be accomplished by wiping the vial stopper thoroughly with cotton or gauze that has been moistened with the recommended alcohol just prior to use.
HOW SUPPLIEDLidocaine Hydrochloride Injection, USP is supplied as follows:
|
NDC |
Container |
Concentration |
Size |
Total (mg) |
|
|
|
|
|
|
|
|
|
|
|
|
|
Single-dose: |
|
|
|
|
|
|
|
|
|
|
|
0409-4278-01 |
Glass Teartop Vial |
0.5% (5 mg/mL) |
50 mL |
250 |
|
0409-4713-01 |
Glass Ampul |
1% (10 mg/mL) |
2 mL (bulk – 400 units) |
20 |
|
0409-4713-02 |
Glass Ampul |
1% (10 mg/mL) |
5 mL |
50 |
|
0409-4713-05 |
Glass Ampul |
1% (10 mg/mL) |
5 mL (bulk – 400 units) |
50 |
|
0409-4713-20 |
Glass Ampul |
1% (10 mg/mL) |
20 mL |
200 |
|
0409-4713-32 |
Glass Ampul |
1% (10 mg/mL) |
2 mL |
20 |
|
0409-4713-62 |
Glass Ampul |
1% (10 mg/mL) |
2 mL (bulk – 800 units) |
20 |
|
0409-4713-65 |
Glass Ampul |
1% (10 mg/mL) |
5 mL (bulk – 800 units) |
50 |
|
0409-4279-02 |
Glass Teartop Vial |
1% (10 mg/mL) |
30 mL |
300 |
|
0409-4270-01 |
Sterile Glass Teartop Vial |
1% (10 mg/mL) |
30 mL |
300 |
|
0409-4776-01 |
Glass Ampul |
1.5% (15 mg/mL) |
20 mL |
300 |
|
0409-4056-01 |
Sterile Glass Ampul |
1.5% (15 mg/mL) |
20 mL |
300 |
|
0409-4282-01 |
Glass Ampul |
2% (20 mg/mL) |
2 mL |
40 |
|
0409-4282-02 |
Glass Ampul |
2% (20 mg/mL) |
10 mL |
200 |
|
|
|
|
|
|
|
Multiple-dose: |
|
|
|
|
|
0409-4275-01 |
Plastic Fliptop Vial |
0.5% (5 mg/mL) |
50 mL |
250 |
|
0409-4276-01 |
Plastic Fliptop Vial |
1% (10 mg/mL) |
20 mL |
200 |
|
0409-4276-02 |
Plastic Fliptop Vial |
1% (10 mg/mL) |
50 mL |
500 |
|
0409-4277-01 |
Plastic Fliptop Vial |
2% (20 mg/mL) |
20 mL |
400 |
|
0409-4277-02 |
Plastic Fliptop Vial |
2% (20 mg/mL) |
50 mL |
1000 |
|
|
|
|
|
|
Single-dose products are preservative-free.
Store at 20 to 25°C (68 to 77°F). [See USP Controlled Room Temperature.]
Lidocaine Hydrochloride Injection, USP solutions packaged in ampuls and glass teartop vials may be autoclaved one time only. Autoclave at 15 pounds pressure, 121°C (250°F) for 15 minutes. DO NOT AUTOCLAVE PRODUCT IN PLASTIC VIALS.
Revised: February, 2010
Printed in USA EN-2421
Hospira, Inc., Lake Forest, IL 60045 USA
Lidocaine Pack Label

Povidone-iodine 10%
Antiseptic
Warnings
Do not use
- if allergic to iodine
- in the eyes
For external use only
Ask a doctor before use if injuries are
- deep or puncture wounds
- serious burns
Stop use and ask a doctor if
- redness, irritation, swelling or pain persists or increases
- infection occurs
Avoid pooling beneath patient
Keep out of reach of children. In case of accidental ingestion, seek professional assistance or consult a poison control center immediately.
MARCAINE SPINAL
(bupivacaine hydrochloride)
injection, solution
[Hospira, Inc.]
bupivacaine hydrochloride in dextrose injection, USP
STERILE HYPERBARIC SOLUTION
FOR SPINAL ANESTHESIA
Rx only
Bupivacaine hydrochloride is 2-Piperidinecarboxamide, 1-butyl- N -(2,6-dimethylphenyl)-, monohydrochloride, monohydrate, a white crystalline powder that is freely soluble in 95 percent ethanol, soluble in water, and slightly soluble in chloroform or acetone. It has the following structural formula:
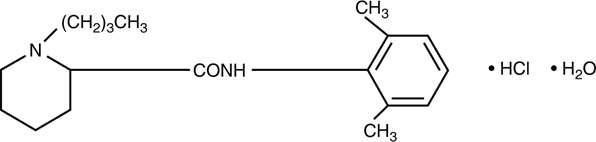
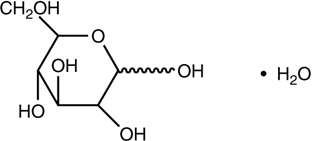
MARCAINETM Spinal is available in sterile hyperbaric solution for subarachnoid injection (spinal block).
Bupivacaine hydrochloride is related chemically and pharmacologically to the aminoacyl local anesthetics. It is a homologue of mepivacaine and is chemically related to lidocaine. All three of these anesthetics contain an amide linkage between the aromatic nucleus and the amino or piperidine group. They differ in this respect from the procaine-type local anesthetics, which have an ester linkage.
Each mL of MARCAINE Spinal contains 7.5 mg bupivacaine hydrochloride (anhydrous) and 82.5 mg dextrose (anhydrous). The pH of this solution is adjusted to between 4.0 and 6.5 with sodium hydroxide or hydrochloric acid.
The specific gravity of MARCAINE Spinal is between 1.030 and 1.035 at 25°C and 1.03 at 37°C.
MARCAINE Spinal does not contain any preservatives.
Local anesthetics block the generation and the conduction of nerve impulses, presumably by increasing the threshold for electrical excitation in the nerve, by slowing the propagation of the nerve impulse, and by reducing the rate of rise of the action potential. In general, the progression of anesthesia is related to the diameter, myelination, and conduction velocity of affected nerve fibers. Clinically, the order of loss of nerve function is as follows: (1) pain, (2) temperature, (3) touch, (4) proprioception, and (5) skeletal muscle tone.
Systemic absorption of local anesthetics produces effects on the cardiovascular and central nervous systems (CNS). At blood concentrations achieved with normal therapeutic doses, changes in cardiac conduction, excitability, refractoriness, contractility, and peripheral vascular resistance are minimal. However, toxic blood concentrations depress cardiac conduction and excitability, which may lead to atrioventricular block, ventricular arrhythmias, and cardiac arrest, sometimes resulting in fatalities. In addition, myocardial contractility is depressed and peripheral vasodilation occurs, leading to decreased cardiac output and arterial blood pressure. Recent clinical reports and animal research suggest that these cardiovascular changes are more likely to occur after unintended direct intravascular injection of bupivacaine. Therefore, when epidural anesthesia with bupivacaine is considered, incremental dosing is necessary.
Following systemic absorption, local anesthetics can produce central nervous system stimulation, depression, or both. Apparent central stimulation is manifested as restlessness, tremors and shivering, progressing to convulsions, followed by depression and coma progressing ultimately to respiratory arrest. However, the local anesthetics have a primary depressant effect on the medulla and on higher centers. The depressed stage may occur without a prior excited stage.
Pharmacokinetics: The rate of systemic absorption of local anesthetics is dependent upon the total dose and concentration of drug administered, the route of administration, the vascularity of the administration site, and the presence or absence of epinephrine in the anesthetic solution. A dilute concentration of epinephrine (1:200,000 or 5 mcg/mL) usually reduces the rate of absorption and peak plasma concentration of MARCAINE, permitting the use of moderately larger total doses and sometimes prolonging the duration of action.
The onset of action with MARCAINE is rapid and anesthesia is long lasting. The duration of anesthesia is significantly longer with MARCAINE than with any other commonly used local anesthetic. It has also been noted that there is a period of analgesia that persists after the return of sensation, during which time the need for strong analgesics is reduced.
The onset of sensory blockade following spinal block with MARCAINE Spinal is very rapid (within one minute); maximum motor blockade and maximum dermatome level are achieved within 15 minutes in most cases. Duration of sensory blockade (time to return of complete sensation in the operative site or regression of two dermatomes) following a 12 mg dose averages 2 hours with or without 0.2 mg epinephrine. The time to return of complete motor ability with 12 mg MARCAINE Spinal averages 3 1/2 hours without the addition of epinephrine and 4 1/2 hours if 0.2 mg epinephrine is added. When compared to equal milligram doses of hyperbaric tetracaine, the duration of sensory blockade was the same but the time to complete motor recovery was significantly longer for tetracaine. Addition of 0.2 mg epinephrine significantly prolongs the motor blockade and time to first postoperative narcotic with MARCAINE Spinal.
Local anesthetics appear to cross the placenta by passive diffusion. The rate and degree of diffusion is governed by (1) the degree of plasma protein binding, (2) the degree of ionization, and (3) the degree of lipid solubility. Fetal/maternal ratios of local anesthetics appear to be inversely related to the degree of plasma protein binding, because only the free, unbound drug is available for placental transfer. MARCAINE with a high protein binding capacity (95%) has a low fetal/maternal ratio (0.2 to 0.4). The extent of placental transfer is also determined by the degree of ionization and lipid solubility of the drug. Lipid soluble, nonionized drugs readily enter the fetal blood from the maternal circulation.
Depending upon the route of administration, local anesthetics are distributed to some extent to all body tissues, with high concentrations found in highly perfused organs such as the liver, lungs, heart, and brain.
Pharmacokinetic studies on the plasma profiles of MARCAINE after direct intravenous injection suggest a three-compartment open model. The first compartment is represented by the rapid intravascular distribution of the drug. The second compartment represents the equilibration of the drug throughout the highly perfused organs such as the brain, myocardium, lungs, kidneys, and liver. The third compartment represents an equilibration of the drug with poorly perfused tissues, such as muscle and fat. The elimination of drug from tissue distribution depends largely upon the ability of binding sites in the circulation to carry it to the liver where it is metabolized.
Various pharmacokinetic parameters of the local anesthetics can be significantly altered by the presence of hepatic or renal disease, addition of epinephrine, factors affecting urinary pH, renal blood flow, the route of drug administration, and the age of the patient. The half-life of MARCAINE in adults is 2.7 hours and in neonates 8.1 hours. In clinical studies, elderly patients exhibited a greater spread and higher maximal level of analgesia than younger patients. Elderly patients also reached the maximal level of analgesia more rapidly than younger patients, and exhibited a faster onset of motor blockade. The total plasma clearance was decreased and the terminal half-life was lengthened in these patients.
Amide-type local anesthetics such as MARCAINE are metabolized primarily in the liver via conjugation with glucuronic acid. Patients with hepatic disease, especially those with severe hepatic disease, may be more susceptible to the potential toxicities of the amide-type local anesthetics. Pipecolylxylidine is the major metabolite of MARCAINE.
The kidney is the main excretory organ for most local anesthetics and their metabolites. Urinary excretion is affected by urinary perfusion and factors affecting urinary pH. Only 6% of bupivacaine is excreted unchanged in the urine.
When administered in recommended doses and concentrations, MARCAINE does not ordinarily produce irritation or tissue damage and does not cause methemoglobinemia.
Uses
MARCAINE Spinal is indicated for the production of subarachnoid block (spinal anesthesia).
Standard textbooks should be consulted to determine the accepted procedures and techniques for the administration of spinal anesthesia.
MARCAINE Spinal is contraindicated in patients with a known hypersensitivity to it or to any local anesthetic agent of the amide-type.
The following conditions preclude the use of spinal anesthesia:
-
Severe hemorrhage, severe hypotension or shock and arrhythmias, such as complete heart block, which severely restrict cardiac output.
-
Local infection at the site of proposed lumbar puncture.
-
Septicemia.
LOCAL ANESTHETICS SHOULD ONLY BE EMPLOYED BY CLINICIANS WHO ARE WELL VERSED IN DIAGNOSIS AND MANAGEMENT OF DOSE-RELATED TOXICITY AND OTHER ACUTE EMERGENCIES WHICH MIGHT ARISE FROM THE BLOCK TO BE EMPLOYED, AND THEN ONLY AFTER INSURING THE IMMEDIATE AVAILABILITY OF OXYGEN, OTHER RESUSCITATIVE DRUGS, CARDIOPULMONARY RESUSCITATIVE EQUIPMENT, AND THE PERSONNEL RESOURCES NEEDED FOR PROPER MANAGEMENT OF TOXIC REACTIONS AND RELATED EMERGENCIES. (See also ADVERSE REACTIONS and PRECAUTIONS .) DELAY IN PROPER MANAGEMENT OF DOSE-RELATED TOXICITY, UNDERVENTILATION FROM ANY CAUSE AND/OR ALTERED SENSITIVITY MAY LEAD TO THE DEVELOPMENT OF ACIDOSIS, CARDIAC ARREST, AND, POSSIBLY, DEATH.
Intra-articular infusions of local anesthetics following arthroscopic and other surgical procedures is an unapproved use, and there have been post-marketing reports of chondrolysis in patients receiving such infusions. The majority of reported cases of chondrolysis have involved the shoulder joint; cases of gleno-humeral chondrolysis have been described in pediatric and adult patients following intra-articular infusions of local anesthetics with and without epinephrine for periods of 48 to 72 hours. There is insufficient information to determine whether shorter infusion periods are not associated with these findings. The time of onset of symptoms, such as joint pain, stiffness and loss of motion can be variable, but may begin as early as the 2nd month after surgery. Currently, there is no effective treatment for chondrolysis; patients who experienced chondrolysis have required additional diagnostic and therapeutic procedures and some required arthroplasty or shoulder replacement.
Spinal anesthetics should not be injected during uterine contractions, because spinal fluid current may carry the drug further cephalad than desired.
A free flow of cerebrospinal fluid during the performance of spinal anesthesia is indicative of entry into the subarachnoid space. However, aspiration should be performed before the anesthetic solution is injected to confirm entry into the subarachnoid space and to avoid intravascular injection.
MARCAINE solutions containing epinephrine or other vasopressors should not be used concomitantly with ergot-type oxytocic drugs, because a severe persistent hypertension may occur. Likewise, solutions of MARCAINE containing a vasoconstrictor, such as epinephrine, should be used with extreme caution in patients receiving monoamine oxidase inhibitors (MAOI) or antidepressants of the triptyline or imipramine types, because severe prolonged hypertension may result.
Until further experience is gained in patients younger than 18 years, administration of MARCAINE in this age group is not recommended.
Mixing or the prior or intercurrent use of any other local anesthetic with MARCAINE cannot be recommended because of insufficient data on the clinical use of such mixtures.
General: The safety and effectiveness of spinal anesthetics depend on proper dosage, correct technique, adequate precautions, and readiness for emergencies. Resuscitative equipment, oxygen, and other resuscitative drugs should be available for immediate use. (See WARNINGS and ADVERSE REACTIONS .) The patient should have IV fluids running via an indwelling catheter to assure a functioning intravenous pathway. The lowest dosage of local anesthetic that results in effective anesthesia should be used. Aspiration for blood should be performed before injection and injection should be made slowly. Tolerance varies with the status of the patient. Elderly patients and acutely ill patients may require reduced doses. Reduced doses may also be indicated in patients with increased intra-abdominal pressure (including obstetrical patients), if otherwise suitable for spinal anesthesia.
There should be careful and constant monitoring of cardiovascular and respiratory (adequacy of ventilation) vital signs and the patient’s state of consciousness after local anesthetic injection. Restlessness, anxiety, incoherent speech, lightheadedness, numbness and tingling of the mouth and lips, metallic taste, tinnitus, dizziness, blurred vision, tremors, depression, or drowsiness may be early warning signs of central nervous system toxicity.
Spinal anesthetics should be used with caution in patients with severe disturbances of cardiac rhythm, shock, or heart block.
Sympathetic blockade occurring during spinal anesthesia may result in peripheral vasodilation and hypotension, the extent depending on the number of dermatomes blocked. Patients over 65 years, particularly those with hypertension, may be at increased risk for experiencing the hypotensive effects of MARCAINE Spinal. Blood pressure should, therefore, be carefully monitored especially in the early phases of anesthesia. Hypotension may be controlled by vasoconstrictors in dosages depending on the severity of hypotension and response of treatment. The level of anesthesia should be carefully monitored because it is not always controllable in spinal techniques.
Because amide-type local anesthetics such as MARCAINE are metabolized by the liver, these drugs, especially repeat doses, should be used cautiously in patients with hepatic disease. Patients with severe hepatic disease, because of their inability to metabolize local anesthetics normally, are at a greater risk of developing toxic plasma concentrations. Local anesthetics should also be used with caution in patients with impaired cardiovascular function because they may be less able to compensate for functional changes associated with the prolongation of AV conduction produced by these drugs. However, dosage recommendations for spinal anesthesia are much lower than dosage recommendations for other major blocks and most experience regarding hepatic and cardiovascular disease dose-related toxicity is derived from these other major blocks.
Serious dose-related cardiac arrhythmias may occur if preparations containing a vasoconstrictor such as epinephrine are employed in patients during or following the administration of potent inhalation agents. In deciding whether to use these products concurrently in the same patient, the combined action of both agents upon the myocardium, the concentration and volume of vasoconstrictor used, and the time since injection, when applicable, should be taken into account.
Many drugs used during the conduct of anesthesia are considered potential triggering agents for familial malignant hyperthermia. Because it is not known whether amide-type local anesthetics may trigger this reaction and because the need for supplemental general anesthesia cannot be predicted in advance, it is suggested that a standard protocol for management should be available. Early unexplained signs of tachycardia, tachypnea, labile blood pressure, and metabolic acidosis may precede temperature elevation. Successful outcome is dependent on early diagnosis, prompt discontinuance of the suspect triggering agent(s) and institution of treatment, including oxygen therapy, indicated supportive measures, and dantrolene. (Consult dantrolene sodium intravenous package insert before using.)
The following conditions may preclude the use of spinal anesthesia, depending upon the physician’s evaluation of the situation and ability to deal with the complications or complaints which may occur:
-
Pre-existing diseases of the central nervous system, such as those attributable to pernicious anemia, poliomyelitis, syphilis, or tumor.
-
Hematological disorders predisposing to coagulopathies or patients on anticoagulant therapy. Trauma to a blood vessel during the conduct of spinal anesthesia may, in some instances, result in uncontrollable central nervous system hemorrhage or soft tissue hemorrhage.
-
Chronic backache and preoperative headache.
-
Hypotension and hypertension.
-
Technical problems (persistent paresthesias, persistent bloody tap).
-
Arthritis or spinal deformity.
-
Extremes of age.
-
Psychosis or other causes of poor cooperation by the patient.
Information for Patients: When appropriate, patients should be informed in advance that they may experience temporary loss of sensation and motor activity, usually in the lower half of the body, following proper administration of spinal anesthesia. Also, when appropriate, the physician should discuss other information including adverse reactions in the MARCAINE Spinal package insert.
Clinically Significant Drug Interactions: The administration of local anesthetic solutions containing epinephrine or norepinephrine to patients receiving monoamine oxidase inhibitors or tricyclic antidepressants may produce severe, prolonged hypertension. Concurrent use of these agents should generally be avoided. In situations when concurrent therapy is necessary, careful patient monitoring is essential.
Concurrent administration of vasopressor drugs and of ergot-type oxytocic drugs may cause severe persistent hypertension or cerebrovascular accidents.
Phenothiazines and butyrophenones may reduce or reverse the pressor effect of epinephrine.
Carcinogenesis, Mutagenesis, and Impairment of Fertility: Long-term studies in animals to evaluate the carcinogenic potential of bupivacaine hydrochloride have not been conducted. The mutagenic potential and the effect on fertility of bupivacaine hydrochloride have not been determined.
Pregnancy Category C: Decreased pup survival in rats and an embryocidal effect in rabbits have been observed when bupivacaine hydrochloride was administered to these species in doses comparable to 230 and 130 times respectively the maximum recommended human spinal dose. There are no adequate and well-controlled studies in pregnant women of the effect of bupivacaine on the developing fetus. Bupivacaine hydrochloride should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. This does not exclude the use of MARCAINE Spinal at term for obstetrical anesthesia. (See Labor and Delivery. )
Labor and Delivery: Spinal anesthesia has a recognized use during labor and delivery. Bupivacaine hydrochloride, when administered properly, via the epidural route in doses 10 to 12 times the amount used in spinal anesthesia has been used for obstetrical analgesia and anesthesia without evidence of adverse effects on the fetus.
Maternal hypotension has resulted from regional anesthesia. Local anesthetics produce vasodilation by blocking sympathetic nerves. Elevating the patient’s legs and positioning her on her left side will help prevent decreases in blood pressure. The fetal heart rate also should be monitored continuously and electronic fetal monitoring is highly advisable.
It is extremely important to avoid aortocaval compression by the gravid uterus during administrations of regional block to parturients. To do this, the patient must be maintained in the left lateral decubitus position or a blanket roll or sandbag may be placed beneath the right hip and the gravid uterus displaced to the left.
Spinal anesthesia may alter the forces of parturition through changes in uterine contractility or maternal expulsive efforts. Spinal anesthesia has also been reported to prolong the second stage of labor by removing the parturient’s reflex urge to bear down or by interfering with motor function. The use of obstetrical anesthesia may increase the need for forceps assistance.
The use of some local anesthetic drug products during labor and delivery may be followed by diminished muscle strength and tone for the first day or two of life. This has not been reported with bupivacaine.
There have been reports of cardiac arrest during use of MARCAINE 0.75% solution for epidural anesthesia in obstetrical patients. The package insert for MARCAINE hydrochloride for epidural, nerve block, etc., has a more complete discussion of preparation for, and management of, this problem. These cases are compatible with systemic toxicity following unintended intravascular injection of the much larger doses recommended for epidural anesthesia and have not occurred within the dose range of bupivacaine hydrochloride 0.75% recommended for spinal anesthesia in obstetrics. The 0.75% concentration of MARCAINE is therefore not recommended for obstetrical epidural anesthesia. MARCAINE Spinal (bupivacaine hydrochloride in dextrose injection) is recommended for spinal anesthesia in obstetrics.
Nursing Mothers: Bupivacaine has been reported to be excreted in human milk suggesting that the nursing infant could be theoretically exposed to a dose of the drug. Because of the potential for serious adverse reactions in nursing infants from bupivacaine, a decision should be made whether to discontinue nursing or not administer bupivacaine, taking into account the importance of the drug to the mother.
Pediatric Use: Until further experience is gained in patients younger than 18 years, administration of MARCAINE Spinal in this age group is not recommended.
Geriatric Use: Patients over 65 years, particularly those with hypertension, may be at increased risk for developing hypotension while undergoing spinal anesthesia with MARCAINE Spinal. (See PRECAUTIONS, General and ADVERSE REACTIONS , Cardiovascular System .)
Elderly patients may require lower doses of MARCAINE Spinal. (See PRECAUTIONS, General and DOSAGE AND ADMINISTRATION .)
In clinical studies, differences in various pharmacokinetic parameters have been observed between elderly and younger patients. (See CLINICAL PHARMACOLOGY, Pharmacokinetics .)
This product is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function. (See CLINICAL PHARMACOLOGY, Pharmacokinetics .)
Reactions to bupivacaine are characteristic of those associated with other amide-type local anesthetics.
The most commonly encountered acute adverse experiences which demand immediate countermeasures following the administration of spinal anesthesia are hypotension due to loss of sympathetic tone and respiratory paralysis or underventilation due to cephalad extension of the motor level of anesthesia. These may lead to cardiac arrest if untreated. In addition, dose-related convulsions and cardiovascular collapse may result from diminished tolerance, rapid absorption from the injection site, or from unintentional intravascular injection of a local anesthetic solution. Factors influencing plasma protein binding, such as acidosis, systemic diseases which alter protein production, or competition of other drugs for protein binding sites, may diminish individual tolerance.
Respiratory System: Respiratory paralysis or underventilation may be noted as a result of upward extension of the level of spinal anesthesia and may lead to secondary hypoxic cardiac arrest if untreated. Preanesthetic medication, intraoperative analgesics and sedatives, as well as surgical manipulation, may contribute to underventilation. This will usually be noted within minutes of the injection of spinal anesthetic solution, but because of differing maximal onset times, differing intercurrent drug usage and differing surgical manipulation, it may occur at any time during surgery or the immediate recovery period.
Cardiovascular System: Hypotension due to loss of sympathetic tone is a commonly encountered extension of the clinical pharmacology of spinal anesthesia. This is more commonly observed in elderly patients, particularly those with hypertension, and patients with shrunken blood volume, shrunken interstitial fluid volume, cephalad spread of the local anesthetic, and/or mechanical obstruction of venous return. Nausea and vomiting are frequently associated with hypotensive episodes following the administration of spinal anesthesia. High doses, or inadvertent intravascular injection, may lead to high plasma levels and related depression of the myocardium, decreased cardiac output, bradycardia, heart block, ventricular arrhythmias, and, possibly, cardiac arrest. (See WARNINGS , PRECAUTIONS , and OVERDOSAGE sections.)
Central Nervous System : Respiratory paralysis or underventilation secondary to cephalad spread of the level of spinal anesthesia (see Respiratory System ) and hypotension for the same reason (see Cardiovascular System ) are the two most commonly encountered central nervous system-related adverse observations which demand immediate countermeasures.
High doses or inadvertent intravascular injection may lead to high plasma levels and related central nervous system toxicity characterized by excitement and/or depression. Restlessness, anxiety, dizziness, tinnitus, blurred vision, or tremors may occur, possibly proceeding to convulsions. However, excitement may be transient or absent, with depression being the first manifestation of an adverse reaction. This may quickly be followed by drowsiness merging into unconsciousness and respiratory arrest.
Neurologic: The incidences of adverse neurologic reactions associated with the use of local anesthetics may be related to the total dose of local anesthetic administered and are also dependent upon the particular drug used, the route of administration, and the physical status of the patient. Many of these effects may be related to local anesthetic techniques, with or without a contribution from the drug.
Neurologic effects following spinal anesthesia may include loss of perineal sensation and sexual function; persistent anesthesia, paresthesia, weakness and paralysis of the lower extremities, and loss of sphincter control all of which may have slow, incomplete, or no recovery; hypotension, high or total spinal block; urinary retention; headache; backache; septic meningitis, meningismus; arachnoiditis; slowing of labor; increased incidence of forceps delivery; shivering; cranial nerve palsies due to traction on nerves from loss of cerebrospinal fluid; and fecal and urinary incontinence.
Allergic: Allergic-type reactions are rare and may occur as a result of sensitivity to the local anesthetic. These reactions are characterized by signs such as urticaria, pruritus, erythema, angioneurotic edema (including laryngeal edema), tachycardia, sneezing, nausea, vomiting, dizziness, syncope, excessive sweating, elevated temperature, and, possibly, anaphylactoid-like symptomatology (including severe hypotension). Cross sensitivity among members of the amide-type local anesthetic group has been reported. The usefulness of screening for sensitivity has not been definitely established.
Other: Nausea and vomiting may occur during spinal anesthesia.
Acute emergencies from local anesthetics are generally related to high plasma levels encountered during therapeutic use or to underventilation (and perhaps apnea) secondary to upward extension of spinal anesthesia. Hypotension is commonly encountered during the conduct of spinal anesthesia due to relaxation of sympathetic tone, and sometimes, contributory mechanical obstruction of venous return.
Management of Local Anesthetic Emergencies: The first consideration is prevention, best accomplished by careful and constant monitoring of cardiovascular and respiratory vital signs and the patient’s state of consciousness after each local anesthetic injection. At the first sign of change, oxygen should be administered.
The first step in the management of systemic toxic reactions, as well as underventilation or apnea due to a high or total spinal, consists of immediate attention to the establishment and maintenance of a patent airway and effective assisted or controlled ventilation with 100% oxygen with a delivery system capable of permitting immediate positive airway pressure by mask. This may prevent convulsions if they have not already occurred.
If necessary, use drugs to control the convulsions. A 50 mg to 100 mg bolus IV injection of succinylcholine will paralyze the patient without depressing the central nervous or cardiovascular systems and facilitate ventilation. A bolus IV dose of 5 mg to 10 mg of diazepam or 50 mg to 100 mg of thiopental will permit ventilation and counteract central nervous system stimulation, but these drugs also depress central nervous system, respiratory and cardiac function, add to postictal depression and may result in apnea. Intravenous barbiturates, anticonvulsant agents, or muscle relaxants should only be administered by those familiar with their use. Immediately after the institution of these ventilatory measures, the adequacy of the circulation should be evaluated. Supportive treatment of circulatory depression may require administration of intravenous fluids, and, when appropriate, a vasopressor dictated by the clinical situation (such as ephedrine or epinephrine to enhance myocardial contractile force).
Hypotension due to sympathetic relaxation may be managed by giving intravenous fluids (such as isotonic saline or lactated Ringer’s solution), in an attempt to relieve mechanical obstruction of venous return, or by using vasopressors (such as ephedrine which increases the force of myocardial contractions) and, if indicated, by giving plasma expanders or whole blood.
Endotracheal intubation, employing drugs and techniques familiar to the clinician, may be indicated after initial administration of oxygen by mask if difficulty is encountered in the maintenance of a patent airway, or if prolonged ventilatory support (assisted or controlled) is indicated.
Recent clinical data from patients experiencing local anesthetic-induced convulsions demonstrated rapid development of hypoxia, hypercarbia, and acidosis with bupivacaine within a minute of the onset of convulsions. These observations suggest that oxygen consumption and carbon dioxide production are greatly increased during local anesthetic convulsions and emphasize the importance of immediate and effective ventilation with oxygen which may avoid cardiac arrest.
If not treated immediately, convulsions with simultaneous hypoxia, hypercarbia, and acidosis plus myocardial depression from the direct effects of the local anesthetic may result in cardiac arrhythmias, bradycardia, asystole, ventricular fibrillation, or cardiac arrest. Respiratory abnormalities, including apnea, may occur. Underventilation or apnea due to a high or total spinal may produce these same signs and also lead to cardiac arrest if ventilatory support is not instituted. If cardiac arrest should occur, standard cardiopulmonary resuscitative measures should be instituted and maintained for a prolonged period if necessary. Recovery has been reported after prolonged resuscitative efforts.
The supine position is dangerous in pregnant women at term because of aortocaval compression by the gravid uterus. Therefore during treatment of systemic toxicity, maternal hypotension, or fetal bradycardia following regional block, the parturient should be maintained in the left lateral decubitus position if possible, or manual displacement of the uterus off the great vessels be accomplished.
The mean seizure dosage of bupivacaine in rhesus monkeys was found to be 4.4 mg/kg with mean arterial plasma concentration of 4.5 mcg/mL. The intravenous and subcutaneous LD50 in mice is 6 mg/kg to 8 mg/kg and 38 mg/kg to 54 mg/kg respectively.
The dose of any local anesthetic administered varies with the anesthetic procedure, the area to be anesthetized, the vascularity of the tissues, the number of neuronal segments to be blocked, the depth of anesthesia and degree of muscle relaxation required, the duration of anesthesia desired, individual tolerance, and the physical condition of the patient. The smallest dose and concentration required to produce the desired result should be administered. Dosages of MARCAINE Spinal should be reduced for elderly and debilitated patients and patients with cardiac and/or liver disease.
For specific techniques and procedures, refer to standard textbooks.
There have been adverse event reports of chondrolysis in patients receiving intra-articular infusions of local anesthetics following arthroscopic and other surgical procedures. MARCAINE Spinal is not approved for this use (see WARNINGS and DOSAGE AND ADMINISTRATION ).
The extent and degree of spinal anesthesia depend upon several factors including dosage, specific gravity of the anesthetic solution, volume of solution used, force of injection, level of puncture, and position of the patient during and immediately after injection.
Seven and one-half mg (7.5 mg or 1 mL) MARCAINE Spinal has generally proven satisfactory for spinal anesthesia for lower extremity and perineal procedures including TURP and vaginal hysterectomy. Twelve mg (12 mg or 1.6 mL) has been used for lower abdominal procedures such as abdominal hysterectomy, tubal ligation, and appendectomy. These doses are recommended as a guide for use in the average adult and may be reduced for the elderly or debilitated patients. Because experience with MARCAINE Spinal is limited in patients below the age of 18 years, dosage recommendations in this age group cannot be made.
Obstetrical Use: Doses as low as 6 mg bupivacaine hydrochloride have been used for vaginal delivery under spinal anesthesia. The dose range of 7.5 mg to 10.5 mg (1 mL to 1.4 mL) bupivacaine hydrochloride has been used for Cesarean section under spinal anesthesia.
In recommended doses, MARCAINE Spinal produces complete motor and sensory block.
Unused portions of solutions should be discarded following initial use.
MARCAINE Spinal should be inspected visually for discoloration and particulate matter prior to administration; solutions which are discolored or which contain particulate matter should not be administered.
Single-dose ampuls of 2 mL (15 mg bupivacaine hydrochloride with 165 mg dextrose), is supplied as follows:
| NDC No. | Container | Fill | Quantity |
| 0409-1761-02 | Uni-AmpTM | 2 mL | package of 10 |
| 0409-1761-62 | Uni-AmpTM | 2 mL | bulk package of 800 |
Store at 20 to 25ºC (68 to 77ºF). [See USP Controlled Room Temperature.]
MARCAINE Spinal solution may be autoclaved once at 15 pound pressure, 121°C (250°F) for 15 minutes. Do not administer any solution which is discolored or contains particulate matter.
Hospira, Inc., Lake Forest, IL 60045 USA
Package Label Display Panel

Package Label Display Panel

A3301-25 PORTEX SPINAL 25G WHITACRE C47916
| |||||||||||||||||||||||||||||||||||||||||||||