Naratriptan
Sun Pharmaceutical Industries Limited
Naratriptan Tablets, USP
FULL PRESCRIBING INFORMATION: CONTENTS*
- NARATRIPTAN DESCRIPTION
- CLINICAL PHARMACOLOGY
- CLINICAL TRIALS
- NARATRIPTAN INDICATIONS AND USAGE
- NARATRIPTAN CONTRAINDICATIONS
- WARNINGS
- PRECAUTIONS
- NARATRIPTAN ADVERSE REACTIONS
- DRUG ABUSE AND DEPENDENCE
- OVERDOSAGE
- NARATRIPTAN DOSAGE AND ADMINISTRATION
- HOW SUPPLIED
- PATIENT INFORMATION
- PRINCIPAL DISPLAY PANEL-label
- PRINCIPAL DISPLAY PANEL-showbox
FULL PRESCRIBING INFORMATION
NARATRIPTAN DESCRIPTION
Naratriptan tablets, USP contain naratriptan as the hydrochloride, which is a selective 5- hydroxytryptamine1 receptor subtype agonist. Naratriptan hydrochloride is chemically designated as N-methyl-3-(1-methyl-4-piperidinyl)-1H-indole-5-ethanesulfonamide monohydrochloride, and it has the following structure:
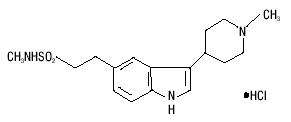
The molecular formula is C17H25N3O2S•HCl, representing a molecular weight of 371.93. Naratriptan hydrochloride is a white to pale yellow powder that is readily soluble in water. Each naratriptan tablet, USP for oral administration contains 2.78 mg of naratriptan hydrochloride USP equivalent to 2.5 mg of naratriptan. Each tablet also contains the inactive ingredients microcrystalline cellulose, anhydrous lactose, croscarmellose sodium, magnesium stearate; and polyethylene glycol, hypromellose, iron oxide yellow, FD&C Blue No. 2 aluminum lake and titanium dioxide for coloring.
CLINICAL PHARMACOLOGY
Mechanism of Action
Naratriptan binds with high affinity to 5-HT1D and 5-HT1B receptors and has no significant affinity or pharmacological activity at 5-HT2-4 receptor subtypes or at adrenergic α1, α2, or β; dopaminergic D1 or D2; muscarinic; or benzodiazepine receptors.
The therapeutic activity of naratriptan in migraine is generally attributed to its agonist activity at 5-HT1D/1B receptors. Two current theories have been proposed to explain the efficacy of 5-HT1D/1B receptor agonists in migraine. One theory suggests that activation of 5-HT1D/1B receptors located on intracranial blood vessels, including those on the arteriovenous anastomoses, leads to vasoconstriction, which is correlated with the relief of migraine headache. The other hypothesis suggests that activation of 5-HT1D/1B receptors on sensory nerve endings in the trigeminal system results in the inhibition of pro-inflammatory neuropeptide release.
In the anesthetized dog, naratriptan has been shown to reduce the carotid arterial blood flow with little or no effect on arterial blood pressure or total peripheral resistance. While the effect on blood flow was selective for the carotid arterial bed, increases in vascular resistance of up to 30% were seen in the coronary arterial bed. Naratriptan has also been shown to inhibit trigeminal nerve activity in rat and cat. In 10 human subjects with suspected coronary artery disease (CAD) undergoing coronary artery catheterization, there was a 1% to 10% reduction in coronary artery diameter following subcutaneous injection of 1.5 mg of naratriptan.
Pharmacokinetics
Naratriptan tablets are well absorbed, with about 70% oral bioavailability. Following administration of a 2.5 mg tablet orally, the peak concentrations are obtained in 2 to 3 hours. After administration of 1 mg or 2.5 mg tablets, the Cmax is somewhat (about 50%) higher in women (not corrected for milligram-per-kilogram dose) than in men. During a migraine attack, absorption was slower, with a Tmax of 3 to 4 hours. Food does not affect the pharmacokinetics of naratriptan. Naratriptan displays linear kinetics over the therapeutic dose range.
The steady-state volume of distribution of naratriptan is 170 L. Plasma protein binding is 28% to 31% over the concentration range of 50 to 1,000 ng/mL.
Naratriptan is predominantly eliminated in urine, with 50% of the dose recovered unchanged and 30% as metabolites in urine. In vitro, naratriptan is metabolized by a wide range of cytochrome P450 isoenzymes into a number of inactive metabolites.
The mean elimination half-life of naratriptan is 6 hours. The systemic clearance of naratriptan is 6.6 mL/min/kg. The renal clearance (220 mL/min) exceeds glomerular filtration rate, indicating active tubular secretion. Repeat administration of naratriptan tablets does not result in drug accumulation.
Special Populations
Age
A small decrease in clearance (approximately 26%) was observed in healthy elderly subjects (65 to 77 years) compared to younger patients, resulting in slightly higher exposure (see PRECAUTIONS).
Race
The effect of race on the pharmacokinetics of naratriptan has not been examined.
Renal Impairment
Clearance of naratriptan was reduced by 50% in patients with moderate renal impairment (creatinine clearance: 18 to 39 mL/min) compared to the normal group. Decrease in clearances resulted in an increase of mean half-life from 6 hours (healthy) to 11 hours (range: 7 to 20 hours). The mean Cmax increased by approximately 40%. The effects of severe renal impairment (creatinine clearance: ≤15 mL/min) on the pharmacokinetics of naratriptan has not been assessed (see CONTRAINDICATIONS and DOSAGE AND ADMINISTRATION).
Hepatic Impairment
Clearance of naratriptan was decreased by 30% in patients with moderate hepatic impairment (Child-Pugh grade A or B). This resulted in an approximately 40% increase in the half-life (range: 8 to 16 hours). The effects of severe hepatic impairment (Child-Pugh grade C) on the pharmacokinetics of naratriptan have not been assessed (see CONTRAINDICATIONS and DOSAGE AND ADMINISTRATION).
Drug Interactions
In normal volunteers, coadministration of single doses of naratriptan tablets and alcohol did not result in substantial modification of naratriptan pharmacokinetic parameters.
From population pharmacokinetic analyses, coadministration of naratriptan and fluoxetine, beta-blockers, or tricyclic antidepressants did not affect the clearance of naratriptan.
Naratriptan does not inhibit monoamine oxidase (MAO) enzymes and is a poor inhibitor of P450; metabolic interactions between naratriptan and drugs metabolized by P450 or MAO are therefore unlikely.
Oral Contraceptives
Oral contraceptives reduced clearance by 32% and volume of distribution by 22%, resulting in slightly higher concentrations of naratriptan. Hormone replacement therapy had no effect on pharmacokinetics in older female patients.
Smoking increased the clearance of naratriptan by 30%.
CLINICAL TRIALS
The efficacy of naratriptan tablets in the acute treatment of migraine headaches was evaluated in 6 randomized, double-blind, placebo-controlled studies of which 4 used the recommended dosing regimen and were conducted as outpatient trials. Three of these studies enrolled adult patients who were predominantly female (86%) and Caucasian (96%) with a mean age of 41 (range: 18 to 65). One study enrolled adolescents with a mean age of 14 (range: 12 to 17). In the adolescent study, 54% of the patients were female and 89% were Caucasian. In all studies, patients were instructed to treat at least 1 moderate to severe headache. Headache response, defined as a reduction in headache severity from moderate or severe pain to mild or no pain, was assessed up to 4 hours after dosing. Associated symptoms such as nausea, vomiting, photophobia, and phonophobia were also assessed. Maintenance of response was assessed for up to 24 hours postdose. A second dose of naratriptan tablets or other medication was allowed 4 to 24 hours after the initial treatment for recurrent headache. The frequency and time to use of these additional treatments were also determined.
In all 3 trials in adults utilizing the recommended dosage regimen and outpatient use, the percentage of patients achieving headache response 4 hours after treatment, the primary outcome measure, was significantly greater among patients receiving naratriptan hydrochloride compared to those who received placebo. In all studies, response to 2.5 mg was numerically greater than response to 1 mg and in the largest of the 3 studies, there was a statistically significant greater percentage of patients with headache response at 4 hours in the 2.5 mg group compared to the 1 mg group. The results are summarized in Table 1.
| Naratriptan Hydrochloride | Naratriptan Hydrochloride | ||
|---|---|---|---|
| Placebo | 1 mg | 2.5 mg | |
| Study 1 |
34% (n = 122) |
50% |
60% |
| Study 2 |
27% (n = 104) |
52% |
66%  |
| Study 3 |
32% (n = 169) |
54% |
65% |
In the single study in adolescents, there were no statistically significant differences between any of the treatment groups. The headache response rates at 4 hours (n) were 65% (n = 74), 67% (n = 78), and 64% (n = 70) for placebo, 1 mg, and 2.5 mg groups, respectively.
Comparisons of drug performance based upon results obtained in different clinical trials are never reliable. Because studies are conducted at different times, with different samples of patients, by different investigators, employing different criteria and/or different interpretations of the same criteria, under different conditions (dose, dosing regimen, etc.), quantitative estimates of treatment response and the timing of response may be expected to vary considerably from study to study.
The estimated probability of achieving an initial headache response in adults over the 4 hours following treatment is depicted in Figure 1.
Figure 1. Estimated Probability of Achieving Initial Headache Response Within 4 Hours*
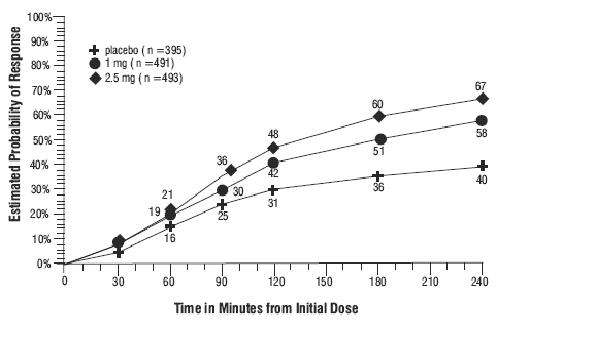
* The figure shows the probability over time of obtaining headache response (no or mild pain) following treatment with naratriptan tablets. The averages displayed are based on pooled data from the 3 controlled clinical trials providing evidence of efficacy (Studies 1, 2, and 3). In this Kaplan-Meier plot, patients not achieving response within 240 minutes were censored at 240 minutes.
For patients with migraine-associated nausea, photophobia, and phonophobia at baseline, there was a lower incidence of these symptoms 4 hours following administration of 1 mg and 2.5 mg naratriptan tablets compared to placebo.
Four to 24 hours following the initial dose of study treatment, patients were allowed to use additional treatment for pain relief in the form of a second dose of study treatment or other medication. The estimated probability of patients taking a second dose or other medication for migraine over the 24 hours following the initial dose of study treatment is summarized in Figure 2.
Figure 2. Estimated Probability of Patients Taking a Second Dose of Naratriptan Tablets or Other Medication for Migraine Over the 24 Hours Following the Initial Dose of Study Treatment*
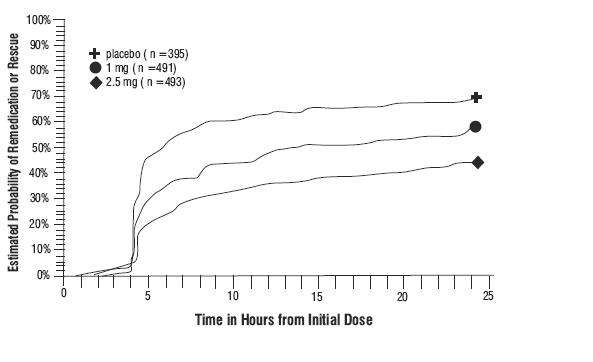
* Kaplan-Meier plot based on data obtained in the 3 controlled clinical trials (Studies 1, 2, and 3) providing evidence of efficacy with patients not using additional treatments censored at 24 hours. The plot also includes patients who had no response to the initial dose. Remedication was discouraged prior to 4 hours postdose.
There is no evidence that doses of 5 mg provide a greater effect than 2.5 mg. There was no evidence to suggest that treatment with naratriptan hydrochloride was associated with an increase in the severity or frequency of migraine attacks. The efficacy of naratriptan tablets was unaffected by presence of aura; gender, age, or weight of the patient; oral contraceptive use; or concomitant use of common migraine prophylactic drugs (e.g., beta-blockers, calcium channel blockers, tricyclic antidepressants). There was insufficient data to assess the impact of race on efficacy.
NARATRIPTAN INDICATIONS AND USAGE
Naratriptan tablets, USP are indicated for the acute treatment of migraine attacks with or without aura in adults.
Naratriptan tablets, USP are not intended for the prophylactic therapy of migraine or for use in the management of hemiplegic or basilar migraine (see CONTRAINDICATIONS). Safety and effectiveness of naratriptan tablets, USP have not been established for cluster headache, which is present in an older, predominantly male population.
NARATRIPTAN CONTRAINDICATIONS
Naratriptan tablets should not be given to patients with history, symptoms, or signs of ischemic cardiac, cerebrovascular, or peripheral vascular syndromes. In addition, patients with other significant underlying cardiovascular diseases should not receive naratriptan tablets. Ischemic cardiac syndromes include, but are not limited to, angina pectoris of any type (e.g., stable angina of effort, vasospastic forms of angina such as the Prinzmetal variant), all forms of myocardial infarction, and silent myocardial ischemia. Cerebrovascular syndromes include, but are not limited to, strokes of any type as well as transient ischemic attacks. Peripheral vascular disease includes, but is not limited to, ischemic bowel disease (see WARNINGS).
Because naratriptan tablets may increase blood pressure, they should not be given to patients with uncontrolled hypertension (see WARNINGS).
Naratriptan tablets are contraindicated in patients with severe renal impairment (creatinine clearance, <15 mL/min) (see CLINICAL PHARMACOLOGY and DOSAGE AND ADMINISTRATION).
Naratriptan tablets are contraindicated in patients with severe hepatic impairment (Child-Pugh grade C) (see CLINICAL PHARMACOLOGY and DOSAGE AND ADMINISTRATION).
Naratriptan tablets should not be administered to patients with hemiplegic or basilar migraine.
Naratriptan tablets should not be used within 24 hours of treatment with another 5-HT1 agonist, an ergotamine-containing or ergot-type medication like dihydroergotamine or methysergide.
Naratriptan tablets are contraindicated in patients with hypersensitivity to naratriptan or any of the components.
WARNINGS
Naratriptan tablets should only be used where a clear diagnosis of migraine has been established.
Risk of Myocardial Ischemia and/or Infarction and Other Adverse Cardiac Events:
Because of the potential of this class of compounds (5-HT1B/1D agonists) to cause coronary vasospasm, naratriptan should not be given to patients with documented ischemic or vasospastic coronary artery disease (CAD) (see CONTRAINDICATIONS). It is strongly recommended that 5-HT1 agonists (including naratriptan) not be given to patients in whom unrecognized CAD is predicted by the presence of risk factors (e.g., hypertension, hypercholesterolemia, smoker, obesity, diabetes, strong family history of CAD, female with surgical or physiological menopause, male over 40 years of age) unless a cardiovascular evaluation provides satisfactory clinical evidence that the patient is reasonably free of coronary artery and ischemic myocardial disease or other significant underlying cardiovascular disease. The sensitivity of cardiac diagnostic procedures to detect cardiovascular disease or predisposition to coronary artery vasospasm is modest, at best. If, during the cardiovascular evaluation, the patient’s medical history, electrocardiographic, or other investigations reveal findings indicative of, or consistent with, coronary artery vasospasm or myocardial ischemia, naratriptan should not be administered (see CONTRAINDICATIONS).
For patients with risk factors predictive of CAD, who are determined to have a satisfactory cardiovascular evaluation, it is strongly recommended that administration of the first dose of naratriptan take place in the setting of a physician’s office or similar medically staffed and equipped facility. Because cardiac ischemia can occur in the absence of clinical symptoms, consideration should be given to obtaining on the first occasion of use an electrocardiogram (ECG) during the interval immediately following administration of naratriptan tablets, in these patients with risk factors.
It is recommended that patients who are intermittent long-term users of 5-HT1 agonists, including naratriptan tablets, and who have or acquire risk factors predictive of CAD, as described above, undergo periodic cardiovascular evaluation as they continue to use naratriptan tablets.
The systematic approach described above is intended to reduce the likelihood that patients with unrecognized cardiovascular disease will be inadvertently exposed to naratriptan.
Cardiac Events and Fatalities Associated With 5-HT1 Agonists
Naratriptan can cause coronary artery vasospasm (see CLINICAL PHARMACOLOGY). Serious adverse cardiac events, including acute myocardial infarction, life-threatening disturbances of cardiac rhythm, and death have been reported within a few hours following the administration of 5-HT1 agonists. Considering the extent of use of 5-HT1 agonists in patients with migraine, the incidence of these events is extremely low.
Premarketing Experience With Naratriptan Tablets
Among approximately 3,500 patients with migraine who participated in premarketing clinical trials of naratriptan tablets, 4 patients treated with single oral doses of naratriptan ranging from 1 to 10 mg experienced asymptomatic ischemic ECG changes with at least 1, who took 7.5 mg, likely due to coronary vasospasm.
Cerebrovascular Events and Fatalities With 5-HT1 Agonists
Cerebral hemorrhage, subarachnoid hemorrhage, stroke, and other cerebrovascular events have been reported in patients treated with 5-HT1 agonists, and some have resulted in fatalities. In a number of cases, it appears possible that the cerebrovascular events were primary, the agonist having been administered in the incorrect belief that the symptoms experienced were a consequence of migraine, when they were not. It should be noted that patients with migraine may be at increased risk of certain cerebrovascular events (e.g., stroke, hemorrhage, transient ischemic attack).
Other Vasospasm-Related Events
5-HT1 agonists may cause vasospastic reactions other than coronary artery spasm. Both peripheral vascular ischemia and colonic ischemia with abdominal pain and bloody diarrhea have been reported with naratriptan.
Serotonin Syndrome
Serotonin syndrome may occur with triptans, including naratriptan hydrochloride, particularly during combined use with selective serotonin reuptake inhibitors (SSRIs) or serotonin norepinephrine reuptake inhibitors (SNRIs). Serotonin syndrome symptoms may include mental status changes (e.g., agitation, hallucinations, coma), autonomic instability (e.g., tachycardia, labile blood pressure, hyperthermia), neuromuscular aberrations (e.g., hyperreflexia, incoordination), and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). The onset of symptoms can occur within minutes to hours of receiving a new or a greater dose of a serotonergic medication. Treatment with naratriptan tablets should be discontinued if serotonin syndrome is suspected.
Increase in Blood Pressure
In healthy volunteers, dose-related increases in systemic blood pressure have been observed after administration of up to 20 mg of oral naratriptan. At the recommended doses, the elevations are generally small, although an increase of systolic pressure of 32 mmHg was seen in 1 patient following a single 2.5 mg dose. The effect may be more pronounced in the elderly and hypertensive patients. A patient who was mildly hypertensive (the baseline blood pressure was 150/98) experienced a significant increase in blood pressure to 204/144 mmHg 225 minutes after administration of a 10 mg oral dose. Significant elevation in blood pressure, including hypertensive crisis, has been reported on rare occasions in patients receiving 5-HT1 agonists with and without a history of hypertension. Naratriptan is contraindicated in patients with uncontrolled hypertension (see CONTRAINDICATIONS).
An 18% increase in mean pulmonary artery pressure and an 8% increase in mean aortic pressure was seen following dosing with 1.5 mg of subcutaneous naratriptan in a study evaluating 10 subjects with suspected CAD undergoing cardiac catheterization.
Hypersensitivity
Hypersensitivity (anaphylaxis/anaphylactoid) reactions may occur in patients receiving naratriptan. Such reactions can be life threatening or fatal. In general, hypersensitivity reactions to drugs are more likely to occur in individuals with a history of sensitivity to multiple allergens (see CONTRAINDICATIONS).
PRECAUTIONS
General
Chest discomfort (including pain, pressure, heaviness, tightness) has been reported after administration of 5-HT1 agonists, including naratriptan tablets. These events have not been associated with arrhythmias or ischemic ECG changes in clinical trials with naratriptan tablets. Because naratriptan may cause coronary artery vasospasm, patients who experience signs or symptoms suggestive of angina following naratriptan should be evaluated for the presence of CAD or a predisposition to Prinzmetal variant angina before receiving additional doses of naratriptan, and should be monitored electrocardiographically if dosing is resumed and similar symptoms recur. Similarly, patients who experience other symptoms or signs suggestive of decreased arterial flow, such as ischemic bowel syndrome or Raynaud's syndrome following naratriptan administration should be evaluated for atherosclerosis or predisposition to vasospasm (see CONTRAINDICATIONS and WARNINGS).
Naratriptan tablets should also be administered with caution to patients with diseases that may alter the absorption, metabolism, or excretion of drugs, such as impaired renal or hepatic function (see CLINICAL PHARMACOLOGY, CONTRAINDICATIONS, and DOSAGE AND ADMINISTRATION).
Care should be taken to exclude other potentially serious neurological conditions before treating headache in patients not previously diagnosed with migraine or who experience a headache that is atypical for them. There have been rare reports where patients received 5-HT1 agonists for severe headaches that were subsequently shown to have been secondary to an evolving neurologic lesion (see WARNINGS).
For a given attack, if a patient has no response to the first dose of naratriptan hydrochloride, the diagnosis of migraine should be reconsidered before administration of a second dose.
Overuse
Overuse of acute migraine drugs (e.g., ergotamine, triptans, opioids, or a combination of drugs for 10 or more days per month) may lead to exacerbation of headache (medication overuse headache). Medication overuse headache may present as migraine-like daily headaches, or as a marked increase in frequency of migraine attacks. Detoxification of patients, including withdrawal of the overused drugs, and treatment of withdrawal symptoms (which often includes a transient worsening of headache) may be necessary. Migraine patients should be informed about the risks of medication overuse and encouraged to record headache frequency and drug use.
Information for Patients
See PATIENT INFORMATION at the end of the full prescribing information for the text of the separate leaflet provided for patients.
Patients should be cautioned about the risk of serotonin syndrome with the use of naratriptan or other triptans, especially during combined use with SSRIs or SNRIs.
Laboratory Tests
No specific laboratory tests are recommended for monitoring patients prior to and/or after treatment with naratriptan tablets.
Drug Interactions
Selective Serotonin Reuptake Inhibitors/Serotonin Norepinephrine Reuptake Inhibitors and Serotonin Syndrome
Cases of life-threatening serotonin syndrome have been reported during combined use of SSRIs or SNRIs and triptans (see WARNINGS).
Ergot-Containing Drugs
Ergot-containing drugs have been reported to cause prolonged vasospastic reactions. Because there is a theoretical basis that these effects may be additive, use of ergotamine-containing or ergot-type medications (like dihydroergotamine or methysergide) and naratriptan within 24 hours is contraindicated (see CONTRAINDICATIONS).
Other 5-HT1 Agonists
The administration of naratriptan with other 5-HT1 agonists has not been evaluated in migraine patients. Because their vasospastic effects may be additive, coadministration of naratriptan and other 5-HT1 agonists within 24 hours of each other is not recommended (see CONTRAINDICATIONS).
Drug/Laboratory Test Interactions
Naratriptan tablets are not known to interfere with commonly employed clinical laboratory tests.
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Lifetime carcinogenicity studies, 104 weeks in duration, were carried out in mice and rats by oral gavage. There was no evidence of an increase in tumors related to naratriptan administration in mice receiving up to 200 mg/kg/day. That dose was associated with a plasma area-under-the-curve (AUC) exposure that was 110 times the exposure in humans receiving the maximum recommended daily dose of 5 mg. Two rat studies were conducted, 1 using a standard diet and the other a nitrite-supplemented diet (naratriptan can be nitrosated in vitro to form a mutagenic product that has been detected in the stomachs of rats fed a high nitrite diet). Doses of 5, 20, and 90 mg/kg were associated with week 13 AUC exposures that in the standard diet study were 7, 40, and 236 times, respectively, and in the nitrite-supplemented diet study were 7, 29, and 180 times, respectively, the exposure attained in humans given the maximum recommended daily dose of 5 mg. In both studies, there was an increase in the incidence of thyroid follicular hyperplasia in high-dose males and females and in thyroid follicular adenomas in high-dose males. In the standard diet study only, there was also an increase in the incidence of benign c-cell adenomas in the thyroid of high-dose males and females. The exposures achieved at the no-effect dose for thyroid tumors were 40 (standard diet) and 29 (nitrite-supplemented diet) times the exposure achieved in humans receiving the maximum recommended daily dose of 5 mg. In the nitrite-supplemented diet study only, the incidence of benign lymphocytic thymoma was increased in all treated groups of females. It was not determined if the nitrosated product is systemically absorbed. However, no changes were seen in the stomachs of rats in that study.
Mutagenesis
Naratriptan was not mutagenic when tested in 2 gene mutation assays, the Ames test and the in vitro thymidine locus mouse lymphoma assay. It was not clastogenic in 2 cytogenetics assays, the in vitro human lymphocyte assay and the in vivo mouse micronucleus assay. Naratriptan can be nitrosated in vitro to form a mutagenic product (WHO nitrosation assay) that has been detected in the stomachs of rats fed a nitrite-supplemented diet.
Impairment of Fertility
In a reproductive toxicity study in which male and female rats were dosed prior to and throughout the mating period with 10, 60, 170, or 340 mg/kg/day (plasma exposures [AUC] approximately 11, 70, 230, and 470 times, respectively, the human exposure at the maximum recommended daily dose [MRDD] of 5 mg), there was a treatment-related decrease in the number of females exhibiting normal estrous cycles at doses of 170 mg/kg/day or greater and an increase in preimplantation loss at 60 mg/kg/day or greater. In high-dose group males, testicular/epididymal atrophy accompanied by spermatozoa depletion reduced mating success and may have contributed to the observed preimplantation loss. The exposures achieved at the no-effect doses for preimplantation loss, anestrus, and testicular effects were approximately 11, 70, and 230 times, respectively, the exposures in humans receiving the MRDD.
In a study in which rats were dosed orally with 10, 60, or 340 mg/kg/day for 6 months, changes in the female reproductive tract including atrophic or cystic ovaries and anestrus were seen at the high dose. The exposure at the no-effect dose of 60 mg/kg was approximately 85 times the exposure in humans receiving the MRDD.
Pregnancy
Teratogenic Effects:
Pregnancy Category C. There are no adequate and well-controlled studies in pregnant women; therefore, naratriptan should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
In reproductive toxicity studies in rats and rabbits, oral administration of naratriptan was associated with developmental toxicity (embryolethality, fetal abnormalities, pup mortality, offspring growth retardation) at doses producing maternal plasma drug exposures as low as 11 and 2.5 times, respectively, the exposure in humans receiving the MRDD of 5 mg.
When pregnant rats were administered naratriptan during the period of organogenesis at doses of 10, 60, or 340 mg/kg/day, there was a dose-related increase in embryonic death, with a statistically significant difference at the highest dose, and incidences of fetal structural variations (incomplete/irregular ossification of skull bones, sternebrae, ribs) were increased at all doses. The maternal plasma exposures (AUC) at these doses were approximately 11, 70, and 470 times the exposure in humans at the MRDD. The high dose was maternally toxic, as evidenced by decreased maternal body weight gain during gestation. A no-effect dose for developmental toxicity in rats exposed during organogenesis was not established.
When doses of 1, 5, or 30 mg/kg/day were given to pregnant Dutch rabbits throughout organogenesis, the incidence of a specific fetal skeletal malformation (fused sternebrae) was increased at the high dose, and increased incidences of embryonic death and fetal variations (major blood vessel variations, supernumerary ribs, incomplete skeletal ossification) were observed at all doses (4, 20, and 120 times, respectively, the MRDD on a body surface area basis). Maternal toxicity (decreased body weight gain) was evident at the high dose in this study. In a similar study in New Zealand White rabbits (1, 5, or 30 mg/kg/day throughout organogenesis), decreased fetal weights and increased incidences of fetal skeletal variations were observed at all doses (maternal exposures equivalent to 2.5, 19, and 140 times exposure in humans receiving the MRDD), while maternal body weight gain was reduced at 5 mg/kg or greater. A no-effect dose for developmental toxicity in rabbits exposed during organogenesis was not established.
When female rats were treated with 10, 60, or 340 mg/kg/day during late gestation and lactation, offspring behavioral impairment (tremors) and decreased offspring viability and growth were observed at doses of 60 mg/kg or greater, while maternal toxicity occurred only at the highest dose. Maternal exposures at the no-effect dose for developmental effects in this study were approximately 11 times the exposure in humans receiving the MRDD.
Nursing Mothers
Naratriptan-related material is excreted in the milk of rats. Therefore, caution should be exercised when considering the administration of naratriptan tablets to a nursing woman.
Pediatric Use
Safety and effectiveness of naratriptan tablets in pediatric patients (younger than 18 years) have not been established.
One randomized, placebo-controlled clinical trial evaluating oral naratriptan (0.25 to 2.5 mg) in pediatric patients aged 12 to 17 years evaluated a total of 300 adolescent migraineurs. This study did not establish the efficacy of oral naratriptan compared to placebo in the treatment of migraine in adolescents (see CLINICAL TRIALS). Adverse events observed in this clinical trial were similar in nature to those reported in clinical trials in adults.
Geriatric Use
The use of naratriptan tablets in elderly patients is not recommended.
Naratriptan is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in elderly patients who have reduced renal function. In addition, elderly patients are more likely to have decreased hepatic function; they are at higher risk for CAD; and blood pressure increases may be more pronounced in the elderly. Clinical studies of naratriptan tablets did not include patients over 65 years of age.
NARATRIPTAN ADVERSE REACTIONS
Serious cardiac events, including some that have been fatal, have occurred following the use of 5-HT1 agonists. These events are extremely rare and most have been reported in patients with risk factors predictive of CAD. Events reported have included coronary artery vasospasm, transient myocardial ischemia, myocardial infarction, ventricular tachycardia, and ventricular fibrillation (see CONTRAINDICATIONS, WARNINGS, and PRECAUTIONS).
Incidence in Controlled Clinical Trials
The most common adverse events were paresthesias, dizziness, drowsiness, malaise/fatigue, and throat/neck symptoms, which occurred at a rate of 2% and at least 2 times placebo rate. Since patients treated only 1 to 3 headaches in the controlled clinical trials, the opportunity for discontinuation of therapy in response to an adverse event was limited. In a long-term, open-label study where patients were allowed to treat multiple migraine attacks for up to 1 year, 15 patients (3.6%) discontinued treatment due to adverse events.
Table 2 lists adverse events that occurred in 5 placebo-controlled clinical trials of approximately 1,752 exposures to placebo and naratriptan tablets in adult migraine patients. The events cited reflect experience gained under closely monitored conditions of clinical trials in a highly selected patient population. In actual clinical practice or in other clinical trials, these frequency estimates may not apply, as the conditions of use, reporting behavior, and the kinds of patients treated may differ. Only events that occurred at a frequency of 2% or more in the group treated with naratriptan tablets 2.5 mg and were more frequent in that group than in the placebo group are included in Table 2. From this table, it appears that many of these adverse events are dose related.
| Adverse Event Type |
Placebo (n = 498) |
Naratriptan Hydrochloride 1 mg (n = 627) |
Naratriptan Hydrochloride 2.5 mg (n = 627) |
| Atypical sensation |
1% |
2% |
4% |
| Paresthesias (all types) |
<1% |
1% |
2% |
| Gastrointestinal |
5% |
6% |
7% |
| Nausea |
4% |
4% |
5% |
| Neurological |
3% |
4% |
7% |
| Dizziness |
1% |
1% |
2% |
| Drowsiness |
<1% |
1% |
2% |
| Malaise/fatigue |
1% |
2% |
2% |
| Pain and pressure sensation |
2% |
2% |
4% |
| Throat/neck symptoms |
1% |
1% |
2% |
One event (vomiting) present in more than 1% of patients receiving naratriptan tablets occurred more frequently on placebo than on naratriptan 2.5 mg.
Naratriptan tablets are generally well tolerated. Most adverse reactions were mild and transient.
The incidence of adverse events in placebo-controlled clinical trials was not affected by age or weight of the patients, duration of headache prior to treatment, presence of aura, use of prophylactic medications, or tobacco use. There was insufficient data to assess the impact of race on the incidence of adverse events.
Other Events Observed in Association With the Administration of Naratriptan Tablets
In the paragraphs that follow, the frequencies of less commonly reported adverse clinical events are presented. Because the reports include events observed in open and uncontrolled studies, the role of naratriptan tablets in their causation cannot be reliably determined. Furthermore, variability associated with adverse event reporting, the terminology used to describe adverse events, etc., limit the value of the quantitative frequency estimates provided. Event frequencies are calculated as the number of patients reporting an event divided by the total number of patients (n = 3,557) exposed to oral naratriptan doses up to 10 mg. All reported events are included except those already listed in the previous table, those too general to be informative, and those not reasonably associated with the use of the drug. Events are further classified within body system categories and enumerated in order of decreasing frequency using the following definitions: frequent adverse events are those occurring in at least 1/100 patients, infrequent adverse events are those occurring in 1/100 to 1/1,000 patients, and rare adverse events are those occurring in fewer than 1/1,000 patients.
Atypical Sensations
Frequent were warm/cold temperature sensations. Infrequent were feeling strange and burning/stinging sensation.
Cardiovascular
Infrequent were palpitations, increased blood pressure, tachyarrhythmias, and abnormal ECG (PR prolongation, QTc prolongation, ST/T wave abnormalities, premature ventricular contractions, atrial flutter, or atrial fibrillation), and syncope. Rare were bradycardia, varicosities, hypotension, and heart murmurs.
Ear, Nose, and Throat
Frequent were ear, nose, and throat infections. Infrequent were phonophobia, sinusitis, upper respiratory inflammation, and tinnitus. Rare were allergic rhinitis; labyrinthitis; ear, nose, and throat hemorrhage; and hearing difficulty.
Endocrine and Metabolic
Infrequent were thirst and polydipsia, dehydration, and fluid retention. Rare were hyperlipidemia, hypercholesterolemia, hypothyroidism, hyperglycemia, glycosuria and ketonuria, and parathyroid neoplasm.
Eye
Frequent was photophobia. Infrequent was blurred vision. Rare were eye pain and discomfort, sensation of eye pressure, eye hemorrhage, dry eyes, difficulty focusing, and scotoma.
Gastrointestinal
Frequent were hyposalivation and vomiting. Infrequent were dyspeptic symptoms, diarrhea, gastrointestinal discomfort and pain, gastroenteritis, and constipation. Rare were abnormal liver function tests, abnormal bilirubin levels, hemorrhoids, gastritis, esophagitis, salivary gland inflammation, oral itching and irritation, regurgitation and reflux, and gastric ulcers.
Hematological Disorders
Infrequent was increased white cells. Rare were thrombocytopenia, quantitative red cell or hemoglobin defects, anemia, and purpura.
Lower Respiratory Tract
Infrequent were bronchitis, cough, and pneumonia. Rare were tracheitis, asthma, pleuritis, and airway constriction and obstruction.
Musculoskeletal
Infrequent were muscle pain, arthralgia and articular rheumatism, muscle cramps and spasms, joint and muscle stiffness, tightness, and rigidity. Rare were bone and skeletal pain.
Neurological
Frequent was vertigo. Infrequent were tremors, cognitive function disorders, sleep disorders, and disorders of equilibrium. Rare were compressed nerve syndromes, confusion, sedation, hyperesthesia, coordination disorders, paralysis of cranial nerves, decreased consciousness, dreams, altered sense of taste, neuralgia, neuritis, aphasia, hypoesthesia, motor retardation, muscle twitching and fasciculation, psychomotor restlessness, and convulsions.
Non-Site Specific
Infrequent were chills and/or fever, descriptions of odor or taste, edema and swelling, allergies, and allergic reactions. Rare were spasms and mobility disorders.
Pain and Pressure Sensations
Frequent were pressure/tightness/heaviness sensations.
Psychiatry
Infrequent were anxiety, depressive disorders, and detachment. Rare were aggression and hostility, agitation, hallucinations, panic, and hyperactivity.
Reproduction
Rare were lumps of female reproductive tract, breast inflammation, inflammation of vagina, inflammation of fallopian tube, breast discharge, endometrium disorders, decreased libido, and lumps of breast.
Skin
Infrequent were sweating, skin rashes, pruritus, and urticaria. Rare were skin erythema, dermatitis and dermatosis, hair loss and alopecia, pruritic skin rashes, acne and folliculitis, allergic skin reactions, macular skin/rashes, skin photosensitivity, photodermatitis, skin flakiness, and dry skin.
Urology
Infrequent were bladder inflammation and polyuria and diuresis. Rare were urinary tract hemorrhage, urinary urgency, pyelitis, and urinary incontinence.
Observed During Clinical Practice
The following section enumerates potentially important adverse events that have occurred in clinical practice and that have been reported spontaneously to various surveillance systems. The events enumerated represent reports arising from both domestic and nondomestic use of naratriptan. These events do not include those already listed in the ADVERSE REACTIONS section above. Because the reports cite events reported spontaneously from worldwide postmarketing experience, frequency of events and the role of naratriptan in their causation cannot be reliably determined.
Cardiovascular
Angina, myocardial infarction (see WARNINGS).
Gastrointestinal
Colonic ischemia (see WARNINGS).
Lower Respiratory
Dyspnea.
Miscellaneous
Hypersensitivity, including anaphylaxis/anaphylactoid reactions, in some cases severe (e.g., circulatory collapse) (see WARNINGS).
Neurologic
Cerebral vascular accident, including transient ischemic attack, subarachnoid hemorrhage, and cerebral infarction (see WARNINGS); serotonin syndrome.
DRUG ABUSE AND DEPENDENCE
In one clinical study enrolling 12 subjects, all of whom had experience using oral opiates and other psychoactive drugs, naratriptan tablets produced less intense subjective responses ordinarily associated with many drugs of abuse than did codeine (30 to 90 mg).
OVERDOSAGE
A patient who was mildly hypertensive experienced a significant increase in blood pressure after administration of a 10 mg dose starting at 30 minutes (baseline value of 150/98 to 204/144 mmHg 225 minutes). This event resolved after treatment with antihypertensive therapy. Oral administration of 25 mg of naratriptan in 1 healthy young male subject increased blood pressure from 120/67 mmHg pretreatment up to 191/113 mmHg at approximately 6 hours postdose and resulted in adverse events including lightheadedness, tension in the neck, tiredness, and loss of coordination. Blood pressure returned to near baseline by 8 hours after dosing without any pharmacological intervention.
Another subject experienced asymptomatic ischemic ECG changes likely due to coronary artery vasospasm approximately 2 hours following a 7.5 mg oral dose.
The elimination half-life of naratriptan is about 6 hours (see CLINICAL PHARMACOLOGY), and therefore monitoring of patients after overdose with naratriptan tablets should continue for at least 24 hours or while symptoms or signs persist. There is no specific antidote to naratriptan. Standard supportive treatment should be applied as required. If the patient presents with chest pain or other symptoms consistent with angina pectoris, ECG monitoring should be performed for evidence of ischemia. It is unknown what effect hemodialysis or peritoneal dialysis has on the serum concentrations of naratriptan.
NARATRIPTAN DOSAGE AND ADMINISTRATION
In controlled clinical trials, single doses of 1 mg and 2.5 mg of naratriptan tablets taken with fluid were effective for the acute treatment of migraines in adults. A greater proportion of patients had headache response following a 2.5 mg dose than following a 1 mg dose (see CLINICAL TRIALS). Individuals may vary in response to doses of naratriptan tablets. The choice of dose should therefore be made on an individual basis, weighing the possible benefit of the 2.5 mg dose with the potential for a greater risk of adverse events. If the headache returns or if the patient has only partial response, the dose may be repeated once after 4 hours, for a maximum dose of 5 mg in a 24-hour period. There is evidence that doses of 5 mg do not provide a greater effect than 2.5 mg.
The safety of treating, on average, more than 4 headaches in a 30-day period has not been established.
Renal Impairment
The use of naratriptan hydrochloride is contraindicated in patients with severe renal impairment (creatinine clearance, <15 mL/min) because of decreased clearance of the drug (see CONTRAINDICATIONS and CLINICAL PHARMACOLOGY). In patients with mild to moderate renal impairment, the maximum daily dose should not exceed 2.5 mg over a 24-hour period and a lower starting dose should be considered.
Hepatic Impairment
The use of naratriptan hydrochloride is contraindicated in patients with severe hepatic impairment (Child-Pugh grade C) because of decreased clearance (see CONTRAINDICATIONS and CLINICAL PHARMACOLOGY). In patients with mild or moderate hepatic impairment, the maximum daily dose should not exceed 2.5 mg over a 24-hour period and a lower starting dose should be considered (see CLINICAL PHARMACOLOGY).
HOW SUPPLIED
Naratriptan tablets, USP 2.5 mg of naratriptan (base) as the hydrochloride. Naratriptan tablets, USP, 2.5 mg, are green, round shaped, biconvex, film-coated tablets debossed with “437” on one side and plain on other side.
Bottles of 30’s with Child Resistant Cap……………NDC 62756-437-83
Bottles of 100’s with Child Resistant Cap…………..NDC 62756-437-88
Bottles of 100’s with Non Child Resistant Cap……..NDC 62756-437-08
Unit-of-Use
blister pack of 9 (1 x 9) tablets…………NDC 62756-437-69
Store at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F) [see USP Controlled Room Temperature].
Dispense in tight container (USP).
PATIENT INFORMATION
The following wording is contained in a separate leaflet provided for patients.
Patient Information
Naratriptan Tablets, USP
Read this Patient Information before you start taking naratriptan tablets and each time you get a refill. There may be new information. This information does not take the place of talking with your healthcare provider about your medical condition or treatment.
What is the most important information I should know about naratriptan tablets?
Naratriptan tablets can cause serious side effects, including:
Heart attack and other heart problems. Heart problems may lead to death.
Stop taking naratriptan tablets and get emergency medical help right away if you have any of the following symptoms of a heart attack:
- discomfort in the center of your chest that lasts for more than a few minutes, or that goes away and comes back.
- chest pain or chest discomfort that feels like heavy pressure, squeezing, or fullness
- pain or discomfort in your arms, back, neck, jaw, or stomach
- shortness of breath with or without chest discomfort
- breaking out in a cold sweat
- nausea or vomiting
- feeling lightheaded
Naratriptan tablets are not for people with risk factors for heart disease unless a heart exam is done and shows no problem. You have a higher risk for heart disease if you:
- have high blood pressure
- have high cholesterol levels
- smoke
- are overweight
- have diabetes
- have a family history of heart disease
- are a female who has gone through menopause
- are a male over age 40
Serotonin syndrome. Serotonin syndrome is a serious and life-threatening problem that can happen in people taking naratriptan tablets, especially if naratriptan tablets are used with anti-depressant medicines called selective serotonin reuptake inhibitors (SSRIs) or selective norepinephrine reuptake inhibitors (SNRIs).
Ask your healthcare provider or pharmacist for a list of these medicines if you are not sure.
Call your healthcare provider right away if you have any of the following symptoms of serotonin syndrome:
- mental changes such as seeing things that are not there (hallucinations), agitation, or coma
- fast heartbeat
- changes in blood pressure
- high body temperature
- tight muscles
- trouble walking
- nausea, vomiting, or diarrhea
What are naratriptan tablets?
Naratriptan tablets are prescription medicine used to treat acute migraine headaches with or without aura in adults.
Naratriptan tablets are not used to prevent or decrease the number of migraine headaches you have.
Naratriptan tablets are not used to treat other types of headaches such as hemiplegic migraines (that make you unable to move on one side of your body) or basilar migraines (rare form of migraine with aura).
It is not known if naratriptan tablets are safe and effective to treat cluster headaches.
It is not known if naratriptan tablets are safe and effective in children under 18 years of age.
Who should not take naratriptan tablets?
Do not take naratriptan tablets if you have:
- heart problems or a history of heart problems
- narrowing of blood vessels to your legs, arms, stomach, or kidney (peripheral vascular disease)
- uncontrolled high blood pressure
- severe kidney problems
- severe liver problems
- hemiplegic migraines or basilar migraines. If you are not sure if you have these types of migraines, ask your healthcare provider.
- had a stroke, transient ischemic attacks (TIAs), or problems with your blood circulation
- taken any of the following medicines in the last 24 hours:
- almotriptan (AXERT®*)
- eletriptan (RELPAX®*)
- frovatriptan (FROVA®*)
- rizatriptan (MAXALT®*, MAXALT-MLT®*)
- sumatriptan (IMITREX®*, SUMAVEL®* DosePro®*)
- sumatriptan and naproxen (TREXIMET®*)
- ergotamines (CAFERGOT®*, ERGOMAR®*, MIGERGOT®*)
- dihydroergotamine (D.H.E. 45®*, MIGRANAL®*)
Ask your doctor if you are not sure if your medicine is listed above.
- an allergy to naratriptan hydrochloride or any of the ingredients in naratriptan tablets. See the end of this leaflet for a complete list of ingredients in naratriptan tablets.
What should I tell my healthcare provider before taking naratriptan tablets?
Before you take naratriptan tablets, tell your healthcare provider about all of your medical conditions, including if you:
- have high blood pressure
- have high cholesterol
- have diabetes
- smoke
- are overweight
- are a female who has gone through menopause
- have heart disease or a family history of heart disease or stroke
- have kidney problems
- have liver problems
- have had epilepsy or seizures
- are not using effective birth control
- are pregnant or plan to become pregnant. It is not known if naratriptan tablets will harm your unborn baby.
- become pregnant while taking naratriptan tablets.
- are breastfeeding or plan to breastfeed. Naratriptan passes into your breast milk and may harm your baby. Talk with your healthcare provider about the best way to feed your baby if you take naratriptan tablets.
Tell your healthcare provider about all the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements.
Naratriptan tablets and other medicines may affect each other, causing side effects.
Especially tell your healthcare provider if you take anti-depressant medicines called:
- selective serotonin reuptake inhibitors (SSRIs)
- serotonin norepinephrine reuptake inhibitors (SNRIs)
- monoamine oxidase inhibitors (MAOIs)
Ask your healthcare provider or pharmacist for a list of these medicines if you are not sure.
Know the medicines you take. Keep a list of them to show your healthcare provider or pharmacist when you get a new medicine.
How should I take naratriptan tablets?
- Certain people should take their first dose of naratriptan tablets in their healthcare provider’s office or in another medical setting. Ask your healthcare provider if you should take your first dose in a medical setting.
- Take naratriptan tablets exactly as your healthcare provider tells you to take it.
- Your healthcare provider may change your dose. Do not change your dose without first talking with your healthcare provider.
- Take naratriptan tablets with water or other liquids.
- If you do not get any relief after your first naratriptan tablet, do not take a second tablet without first talking with your healthcare provider.
- If your headache comes back or you only get some relief from your headache, you can take a second tablet 4 hours after the first tablet.
- Do not take more than a total of 5 mg of naratriptan in a 24-hour period.
- Some people who take too many naratriptan tablets may have worse headaches (medication overuse headache). If your headaches get worse, your healthcare provider may decide to stop your treatment with naratriptan tablets.
- If you take too many naratriptan tablets, call your healthcare provider or go to the nearest hospital emergency room right away.
- You should write down when you have headaches and when you take naratriptan tablets so you can talk with your healthcare provider about how naratriptan tablets are working for you.
What should I avoid while taking naratriptan tablets?
Naratriptan tablets can cause dizziness, weakness, or drowsiness. If you have these symptoms, do not drive a car, use machinery, or do anything where you need to be alert.
What are the possible side effects of naratriptan tablets?
Naratriptan tablets may cause serious side effects. See “What is the most important information I should know about naratriptan tablets?”
These serious side effects include:
- changes in color or sensation in your fingers and toes (Raynaud’s syndrome)
- stomach and intestinal problems (gastrointestinal and colonic ischemic events). Symptoms of gastrointestinal and colonic ischemic events include:
- sudden or severe stomach pain
- stomach pain after meals
- weight loss
- nausea or vomiting
- constipation or diarrhea
- bloody diarrhea
- fever
- problems with blood circulation to your legs and feet (peripheral vascular ischemia). Symptoms of peripheral vascular ischemia include:
- cramping and pain in your legs or hips
- feeling of heaviness or tightness in your leg muscles
- burning or aching pain in your feet or toes while resting
- numbness, tingling, or weakness in your legs
- cold feeling or color changes in 1 or both legs or feet
- shortness of breath or wheezing
- hives (itchy bumps); swelling of your tongue, mouth, or throat
The most common side effects of naratriptan tablets include:
- dizziness
- warm, hot, burning feeling to your face (flushing)
- cold and hot temperature sensations
- sensitivity to light or vision problems
- ear, nose, and throat infections
- feeling weak, drowsy, or tired
- decrease in saliva
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
These are not all the possible side effects of naratriptan tablets. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
How should I store naratriptan tablets?
Store naratriptan tablets at 20° to 25°C (68° to 77°F); excursions permitted between 15° and 30°C (59° and 86°F).
Keep naratriptan tablets and all medicines out of the reach of children.
General information about the safe and effective use of naratriptan tablets.
Medicines are sometimes prescribed for purposes other than those listed in Patient Information leaflets. Do not use naratriptan tablets for a condition for which it was not prescribed. Do not give naratriptan tablets to other people, even if they have the same symptoms you have. It may harm them.
This Patient Information leaflet summarizes the most important information about naratriptan tablets. If you would like more information, talk with your healthcare provider. You can ask your healthcare provider or pharmacist for information about naratriptan tablets that is written for healthcare professionals.
For more information, call 1-800-818-4555.
What are the ingredients in naratriptan tablets?
Active ingredient: naratriptan hydrochloride
Inactive ingredients: microcrystalline cellulose, anhydrous lactose, croscarmellose sodium, magnesium stearate; and polyethylene glycol, hypromellose, iron oxide yellow, FD&C Blue No. 2 aluminum lake and titanium dioxide for coloring
* All trademark names are the property of their respective owners.
This Patient Information has been approved by the U.S. Food and Drug Administration.
Distributed by:
Caraco Pharmaceutical Laboratories, Ltd.
1150 Elijah McCoy Drive, Detroit, MI 48202
Manufactured by:
Sun Pharmaceutical Industries Ltd.
Acme Plaza, Andheri-Kurla Road,
Andheri (East), Mumbai – 400 059
India.
ISS. 04/2013
PGPI0171B
PRINCIPAL DISPLAY PANEL-label
NDC 62756-437-83
Naratriptan Tablets USP
2.5 mg
Rx only
30 TABLETS
SUN PHARMACEUTICAL INDUSTRIES LTD
PHARMACIST: Dispense the patient information leaflet with drug product.

PRINCIPAL DISPLAY PANEL-showbox
NDC 62756-437-69
Naratriptan Tablets USP
2.5 mg
Rx only
9 (1 x 9) Unit-of-Use Tablets
SUN PHARMACEUTICAL INDUSTRIES LTD

NaratriptanNaratriptan TABLET, FILM COATED
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||