Boniva
HIGHLIGHTS OF PRESCRIBING INFORMATIONThese highlights do not include all the information needed to use BONIVA Tablets safely and effectively. See full prescribing information for BONIVA Tablets. BONIVA® (ibandronate sodium) Tablets Initial U.S. Approval: 2003 RECENT MAJOR CHANGES Contraindications (4) 1/2010 Warnings and Precautions (5.1) 1/2010 INDICATIONS AND USAGEBONIVA is a bisphosphonate indicated for the treatment and prevention of postmenopausal osteoporosis. (1.1)DOSAGE AND ADMINISTRATIONOne 150 mg tablet taken once monthly or one 2.5 mg tablet taken once daily (2.1)Dosing instructions (2.2) Swallow whole tablet with 6-8 oz of plain water only, at least 60 minutes before the first food, beverage, or medication of the day. Do not lie down for at least 60 minutes after taking BONIVA. Do not eat, drink (except for water), or take other medication for 60 minutes after taking BONIVA. DOSAGE FORMS AND STRENGTHSTablets: 2.5 mg, 150 mg (3)CONTRAINDICATIONS Abnormalities of the esophagus which delay esophageal emptying such as stricture or achalasia (4, 5.1) Inability to stand or sit upright for at least 60 minutes (4, 5.1) Hypocalcemia (4) Hypersensitivity to BONIVA (4) WARNINGS AND PRECAUTIONS Severe irritation of the upper gastrointestinal (GI) mucosa can occur. Dosing instructions should be followed and caution should be used in patients with active upper GI disease. Discontinue use if new or worsening symptoms occur. (5.1) Hypocalcemia may worsen during treatment. Correct hypocalcemia before use. (5.2) Severe bone, joint, and muscle pain may occur. Consider discontinuing use if symptoms develop. (5.3) Osteonecrosis of the jaw has been reported. (5.4) Side EffectsThe most common adverse reactions (>5%) are back pain, dyspepsia, pain in extremity, diarrhea, headache, and myalgia. (6) To report SUSPECTED ADVERSE REACTIONS, contact Genentech at 1-888-835-2555 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch. DRUG INTERACTIONS Calcium supplements, antacids and some oral medications may interfere with absorption of ibandronate. (7.1) Use caution when co-prescribing aspirin/nonsteroidal anti-inflammatory drugs that may worsen gastrointestinal irritation. (7.2) USE IN SPECIFIC POPULATIONSBONIVA is not recommended in patients with severe renal impairment (creatinine clearance
FULL PRESCRIBING INFORMATION: CONTENTS*
- 1 BONIVA INDICATIONS AND USAGE
- 2 BONIVA DOSAGE AND ADMINISTRATION
- 3 DOSAGE FORMS AND STRENGTHS
- 4 BONIVA CONTRAINDICATIONS
- 5 WARNINGS AND PRECAUTIONS
- 6 BONIVA ADVERSE REACTIONS
- 7 DRUG INTERACTIONS
- 8 USE IN SPECIFIC POPULATIONS
- 10 OVERDOSAGE
- 11 BONIVA DESCRIPTION
- 12 CLINICAL PHARMACOLOGY
- 13 NONCLINICAL TOXICOLOGY
- 14 CLINICAL STUDIES
- 16 HOW SUPPLIED/STORAGE AND HANDLING
- 17 PATIENT COUNSELING INFORMATION
FULL PRESCRIBING INFORMATION
Enter section text here
1 INDICATIONS AND USAGE
Enter section text here
1.1 Treatment and Prevention of Postmenopausal Osteoporosis
BONIVA is indicated for the treatment and prevention of osteoporosis in postmenopausal women. BONIVA increases bone mineral density (BMD) and reduces the incidence of vertebral fractures.
2 DOSAGE AND ADMINISTRATION
Enter section text here
2.1 Dose
The dose of BONIVA is either one 150 mg tablet taken once monthly on the same date each month or one 2.5 mg tablet taken once daily.
2.2 Dosing Instructions
- To maximize absorption and clinical benefit, BONIVA should be taken at least 60 minutes before the first food or drink (other than water) of the day or before taking any oral medication or supplementation, including calcium, antacids, or vitamins (see DRUG INTERACTIONS [7.1]).
- To facilitate delivery to the stomach and thus reduce the potential for esophageal irritation, BONIVA tablets should be swallowed whole with a full glass of plain water (6 to 8 oz) while the patient is standing or sitting in an upright position. Patients should not lie down for 60 minutes after taking BONIVA (see WARNINGS AND PRECAUTIONS [5.1]).
- Patients should not eat, drink anything except water, or take other medications for at least 60 minutes after taking BONIVA.
- Plain water is the only drink that should be taken with BONIVA. Note that some mineral waters may have a higher concentration of calcium and therefore should not be used.
- Patients should not chew or suck the tablet because of a potential for oropharyngeal ulceration.
- The BONIVA 150 mg tablet should be taken on the same date each month (i.e., the patient's BONIVA day).
- The patient must not take two 150 mg tablets within the same week.
- If the once-monthly dose is missed, and the patient's next scheduled BONIVA day is more than 7 days away, the patient should be instructed to take one BONIVA 150 mg tablet in the morning following the date that it is remembered. The patient should then return to taking one BONIVA 150 mg tablet every month in the morning of their chosen day, according to their original schedule.
- If the once-monthly dose is missed, and the patient's next scheduled BONIVA day is only 1 to 7 days away, the patient must wait until the subsequent month's scheduled BONIVA day to take their tablet. The patient should then return to taking one BONIVA 150 mg tablet every month in the morning of their chosen day, according to their original schedule.
2.3 Recommendations for Calcium and Vitamin D Supplementation
Patients should receive supplemental calcium and vitamin D if dietary intake is inadequate (see DRUG INTERACTIONS [7.1]).
2.4 use in Specific Populations
BONIVA is not recommended for use in patients with severe renal impairment (creatinine clearance of <30 mL/min).
No dose adjustment is necessary for patients with mild or moderate renal impairment.
No dose adjustment is necessary for the elderly, or for patients with hepatic impairment.
3 DOSAGE FORMS AND STRENGTHS
Tablets, 2.5 mg and 150 mg
4 CONTRAINDICATIONS
- Abnormalities of the esophagus which delay esophageal emptying such as stricture or achalasia (see Upper Gastrointestinal Adverse Reactions [5.1])
- Inability to stand or sit upright for at least 60 minutes (see Dosing Instructions [2.2], Upper Gastrointestinal Adverse Reactions [5.1])
- Hypocalcemia (see WARNINGS AND PRECAUTIONS [5.2])
- Known hypersensitivity to BONIVA or to any of its excipients (see ADVERSE REACTIONS [6.2]).
5 WARNINGS AND PRECAUTIONS
Enter section text here
5.1 Upper Gastrointestinal Side Effects
BONIVA, like other bisphosphonates administered orally, may cause local irritation of the upper gastrointestinal mucosa. Because of these possible irritant effects and a potential for worsening of the underlying disease, caution should be used when BONIVA is given to patients with active upper gastrointestinal problems (such as known Barrett's esophagus, dysphagia, other esophageal diseases, gastritis, duodenitis or ulcers).
Esophageal adverse experiences, such as esophagitis, esophageal ulcers and esophageal erosions, occasionally with bleeding and rarely followed by esophageal stricture or perforation, have been reported in patients receiving treatment with oral bisphosphonates. In some cases, these have been severe and required hospitalization. Physicians should therefore be alert to any signs or symptoms signaling a possible esophageal reaction and patients should be instructed to discontinue BONIVA and seek medical attention if they develop dysphagia, odynophagia, retrosternal pain or new or worsening heartburn.
The risk of severe esophageal adverse experiences appears to be greater in patients who lie down after taking oral bisphosphonates and/or who fail to swallow it with the recommended full glass (6-8 oz) of water, and/or who continue to take oral bisphosphonates after developing symptoms suggestive of esophageal irritation. Therefore, it is very important that the full dosing instructions are provided to, and understood by, the patient (see DOSAGE AND ADMINISTRATION [2.2]). In patients who cannot comply with dosing instructions due to mental disability, therapy with BONIVA should be used under appropriate supervision.
There have been post-marketing reports of gastric and duodenal ulcers with oral bisphosphonate use, some severe and with complications, although no increased risk was observed in controlled clinical trials.
5.2 Hypocalcemia and Mineral Metabolsim
Treat hypocalcemia and other disturbances of bone and mineral metabolism before starting BONIVA therapy. Adequate intake of calcium and vitamin D is important in all patients to prevent hypocalcemia (see DOSAGE AND ADMINISTRATION [2.3]). Hypocalcemia following dosing has been reported postmarketing.
5.3 Musculoskeletal Pain
Severe and occasionally incapacitating bone, joint, and/or muscle pain has been reported in patients taking BONIVA and other bisphosphonates (see ADVERSE REACTIONS [6]). The time to onset of symptoms varied from one day to several months after starting the drug. Most patients had relief of symptoms after stopping. A subset had recurrence of symptoms when rechallenged with the same drug or another bisphosphonate. Consider discontinuing use if severe symptoms develop.
5.4 Jaw Osteonecrosis
Osteonecrosis, primarily in the jaw, has been reported in patients treated with bisphosphonates. Most cases have been in cancer patients undergoing dental procedures, but some have occurred in patients with postmenopausal osteoporosis or other diagnoses. Known risk factors for osteonecrosis include a diagnosis of cancer, concomitant therapies (e.g., chemotherapy, radiotherapy, corticosteroids), and co-morbid disorders (e.g., anemia, coagulopathy, infection, pre-existing dental disease). Most reported cases have been in patients treated with bisphosphonates intravenously but some have been in patients treated orally (see ADVERSE REACTIONS [6.2]).
For patients who develop osteonecrosis of the jaw (ONJ) while on bisphosphonate therapy, dental surgery may exacerbate the condition. For patients requiring dental procedures, there are no data available to suggest whether discontinuation of bisphosphonate treatment reduces the risk of ONJ. Clinical judgment of the treating physician should guide the management plan of each patient based on individual benefit/risk assessment.
5.5 Severe Renal Impairment
BONIVA is not recommended for use in patients with severe renal impairment (creatinine clearance of <30 mL/min).
6 ADVERSE REACTIONS
Enter section text here
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Treatment and Prevention of Postmenopausal Osteoporosis
Daily Dosing
The safety of BONIVA 2.5 mg once daily in the treatment and prevention of postmenopausal osteoporosis was assessed in 3577 patients aged 41 – 82 years. The duration of the trials was 2 to 3 years, with 1134 patients exposed to placebo and 1140 exposed to BONIVA 2.5 mg. Patients with pre-existing gastrointestinal disease and concomitant use of non-steroidal anti-inflammatory drugs, proton pump inhibitors and H2 antagonists were included in these clinical trials. All patients received 500 mg calcium plus 400 IU vitamin D supplementation daily.
The incidence of all-cause mortality was 1% in the placebo group and 1.2% in the BONIVA 2.5 mg daily group. The incidence of serious adverse events was 20% in the placebo group and 23% in the BONIVA 2.5 mg daily group. The percentage of patients who withdrew from treatment due to adverse events was approximately 17% in both the BONIVA 2.5 mg daily group and the placebo group. Table 1 lists adverse events from the treatment and prevention studies reported in ≥2% of patients and more frequently in patients treated daily with BONIVA than patients treated with placebo.
| Body System | Placebo % (n=1134) |
BONIVA 2.5 mg % (n=1140) |
|---|---|---|
| Body as a Whole |
|
|
| Back Pain | 12.2 | 13.5 |
| Pain in Extremity | 6.4 | 7.8 |
| Infection | 3.4 | 4.3 |
| Asthenia | 2.3 | 3.5 |
| Allergic Reaction | 1.9 | 2.5 |
| Digestive System |
|
|
| Dyspepsia | 9.8 | 11.9 |
| Diarrhea | 5.0 | 6.8 |
| Tooth Disorder | 2.3 | 3.5 |
| Vomiting | 2.1 | 2.7 |
| Gastritis | 1.9 | 2.2 |
| Metabolic and Nutritional Disorders |
|
|
| Hypercholesterolemia | 4.2 | 4.8 |
| Musculoskeletal System |
|
|
| Myalgia | 5.1 | 5.7 |
| Joint Disorder | 3.3 | 3.6 |
| Arthritis | 2.7 | 3.2 |
| Nervous System |
|
|
| Headache | 5.8 | 6.5 |
| Dizziness | 2.6 | 3.7 |
| Vertigo | 2.5 | 3.0 |
| Nerve Root Lesion | 1.9 | 2.2 |
| Respiratory System |
|
|
| Upper Respiratory Infection | 33.2 | 33.7 |
| Bronchitis | 6.8 | 10.0 |
| Pneumonia | 4.3 | 5.9 |
| Pharyngitis | 1.5 | 2.5 |
| Urogenital System |
|
|
| Urinary Tract Infection | 4.2 | 5.5 |
Gastrointestinal Adverse Events
The incidence of adverse events in the placebo and BONIVA 2.5 mg daily groups were: dyspepsia (10% vs. 12%), diarrhea (5% vs. 7%), and abdominal pain (5% vs. 6%).
Musculoskeletal Adverse Events
The incidence of adverse events in the placebo and BONIVA 2.5 mg daily groups were: back pain (12% vs. 14%), arthralgia (14% vs. 14%) and myalgia (5% vs. 6%).
Ocular Adverse Events
Reports in the medical literature indicate that bisphosphonates may be associated with ocular inflammation such as iritis and scleritis. In some cases, these events did not resolve until the bisphosphonate was discontinued. There were no reports of ocular inflammation in studies with BONIVA 2.5 mg daily.
Monthly Dosing
The safety of BONIVA 150 mg once monthly in the treatment of postmenopausal osteoporosis was assessed in a two year trial which enrolled 1583 patients aged 54 – 81 years, with 395 patients exposed to BONIVA 2.5 mg daily and 396 exposed to BONIVA 150 mg monthly. Patients with active or significant pre-existing gastrointestinal disease were excluded from this trial. Patients with dyspepsia or concomitant use of non-steroidal anti-inflammatory drugs, proton pump inhibitors and H2 antagonists were included in this study. All patients received 500 mg calcium plus 400 IU vitamin D supplementation daily.
After one year, the incidence of all-cause mortality was 0.3% in both the BONIVA 2.5 mg daily group and the BONIVA 150 mg monthly group. The incidence of serious adverse events was 5% in the BONIVA 2.5 mg daily group and 7% in the BONIVA 150 mg monthly group. The percentage of patients who withdrew from treatment due to adverse events was 9% in the BONIVA 2.5 mg daily group and 8% in the BONIVA 150 mg monthly group. Table 2 lists the adverse events reported in ≥2% of patients.
| Body System/Adverse Event | BONIVA 2.5 mg Daily % (n=395) |
BONIVA 150 mg Monthly % (n=396) |
|---|---|---|
| Vascular Disorders |
|
|
| Hypertension | 7.3 | 6.3 |
| Gastrointestinal Disorders |
|
|
| Dyspepsia | 7.1 | 5.6 |
| Nausea | 4.8 | 5.1 |
| Diarrhea | 4.1 | 5.1 |
| Constipation | 2.5 | 4.0 |
| Abdominal Pain* | 5.3 | 7.8 |
| Musculoskeletal and Connective Tissue Disorders |
|
|
| Arthralgia | 3.5 | 5.6 |
| Back Pain | 4.3 | 4.5 |
| Pain in Extremity | 1.3 | 4.0 |
| Localized Osteoarthritis | 1.3 | 3.0 |
| Myalgia | 0.8 | 2.0 |
| Muscle Cramp | 2.0 | 1.8 |
| Infections and Infestations |
|
|
| Influenza | 3.8 | 4.0 |
| Nasopharyngitis | 4.3 | 3.5 |
| Bronchitis | 3.5 | 2.5 |
| Urinary Tract Infection | 1.8 | 2.3 |
| Upper Respiratory Tract Infection | 2.0 | 2.0 |
| Nervous System Disorders |
|
|
| Headache | 4.1 | 3.3 |
| Dizziness | 1.0 | 2.3 |
| General Disorders and Administration Site Conditions |
|
|
| Influenza-like Illness† | 0.8 | 3.3 |
| Skin and Subcutaneous Tissue Disorders |
|
|
| Rash‡ | 1.3 | 2.3 |
| Psychiatric Disorders |
|
|
| Insomnia | 0.8 | 2.0 |
Gastrointestinal Adverse Events
The incidence of adverse events in the BONIVA 2.5 mg daily and BONIVA 150 mg monthly groups were: dyspepsia (7% vs. 6%), diarrhea (4% vs. 5%), and abdominal pain (5% vs. 8%).
Musculoskeletal Adverse Events
The incidence of adverse events in the BONIVA 2.5 mg daily and BONIVA 150 mg monthly groups were: back pain (4% vs. 5%), arthralgia (4% vs. 6%) and myalgia (1% vs. 2%).
Acute Phase Reactions
Symptoms consistent with acute phase reactions have been reported with bisphosphonate use. Over the two years of the study, the overall incidence of acute phase reaction symptoms was 3% in the BONIVA 2.5 mg daily group and 9% in the BONIVA 150 mg monthly group. These incidence rates are based on the reporting of any of 33 acute-phase reaction like symptoms within 3 days of the monthly dosing and lasting 7 days or less. Influenza like illness was reported in no patients in the BONIVA 2.5 mg daily group and 2% in the BONIVA 150 mg monthly group.
Ocular Adverse Events
Two patients who received BONIVA 150 mg once-monthly experienced ocular inflammation, one was a case of uveitis and the other scleritis.
One hundred sixty (160) postmenopausal women without osteoporosis participated in a 1-year, double-blind, placebo-controlled study of BONIVA 150 mg once-monthly for prevention of bone loss. Seventy-seven subjects received BONIVA and 83 subjects received placebo. The overall pattern of adverse events was similar to that previously observed.
6.2 Postmarketing Experience
The following adverse reactions have been identified during postapproval use of BONIVA. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Hypersensitivity
Allergic reactions including anaphylaxis, angioedema, bronchospasm and rash have been reported (see CONTRAINDICATIONS [4] ).
Hypocalcemia
Hypocalcemia has been reported in patients treated with BONIVA (see WARNINGS AND PRECAUTIONS [5.2]).
Musculoskeletal Pain
Bone, joint, or muscle pain (musculoskeletal pain), described as severe or incapacitating, has been reported (see WARNINGS AND PRECAUTIONS [5.3] ).
Jaw Osteonecrosis
Osteonecrosis of the jaw has been reported in patients treated with BONIVA (see WARNINGS AND PRECAUTIONS [5.4] ).
7 DRUG INTERACTIONS
Enter section text here
7.1 Calcium Supplements/Antacids
Products containing calcium and other multivalent cations (such as aluminum, magnesium, iron) are likely to interfere with absorption of BONIVA. BONIVA should be taken at least 60 minutes before any oral medications, including medications containing multivalent cations (such as antacids, supplements or vitamins). Also, patients should wait at least 60 minutes after dosing before taking any other oral medications (see PATIENT COUNSELING INFORMATION [17.1]).
7.2 Aspirin/Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
Because aspirin, NSAIDs, and bisphosphonates are all associated with gastrointestinal irritation, caution should be exercised in the concomitant use of aspirin or NSAIDs with BONIVA.
7.3 H2 Blockers
In healthy volunteers, co-administration with ranitidine resulted in a 20% increased bioavailability of ibandronate, which was not considered to be clinically relevant (see CLINICAL PHARMACOLOGY [12.3]).
7.4 Drug/Laboratory Test Interactions
Bisphosphonates are known to interfere with the use of bone-imaging agents. Specific studies with ibandronate have not been performed.
8 USE IN SPECIFIC POPULATIONS
Enter section text here
8.1 Pregnancy: Category C
There are no adequate and well-controlled studies in pregnant women. BONIVA should be used during pregnancy only if the potential benefit justifies the potential risk to the mother and fetus.
Bisphosphonates are incorporated into the bone matrix, from where they are gradually released over periods of weeks to years. The extent of bisphosphonate incorporation into adult bone, and hence, the amount available for release back into the systemic circulation, is directly related to the total dose and duration of bisphosphonate use. Although there are no data on fetal risk in humans, bisphosphonates do cause fetal harm in animals, and animal data suggest that uptake of bisphosphonates into fetal bone is greater than into maternal bone. Therefore, there is a theoretical risk of fetal harm (e.g., skeletal and other abnormalities) if a woman becomes pregnant after completing a course of bisphosphonate therapy. The impact of variables such as time between cessation of bisphosphonate therapy to conception, the particular bisphosphonate used, and the route of administration (intravenous versus oral) on this risk has not been established.
In female rats given ibandronate orally at doses ≥3 times human exposure at the recommended daily oral dose of 2.5 mg or ≥1 times human exposure at the recommended once-monthly oral dose of 150 mg beginning 14 days before mating and continuing through lactation, maternal deaths were observed at the time of delivery in all dose groups. Perinatal pup loss in dams given 45 times human exposure at the recommended daily dose and 13 times the recommended once-monthly dose was likely related to maternal dystocia. Calcium supplementation did not completely prevent dystocia and periparturient mortality in any of the treated groups at ≥16 times the recommended daily dose and ≥4.6 times the recommended once-monthly dose. A low incidence of postimplantation loss was observed in rats treated from 14 days before mating throughout lactation or during gestation, only at doses causing maternal dystocia and periparturient mortality. In pregnant rats dosed orally from gestation day 17 through lactation day 21 (following closure of the hard palate through weaning), maternal toxicity, including dystocia and mortality, fetal perinatal and postnatal mortality, were observed at doses equivalent to human exposure at the recommended daily and ≥4 times the recommended once-monthly dose. Periparturient mortality has also been observed with other bisphosphonates and appears to be a class effect related to inhibition of skeletal calcium mobilization resulting in hypocalcemia and dystocia (see NONCLINICAL TOXICOLOGY [13.2]).
Exposure of pregnant rats during the period of organogenesis resulted in an increased fetal incidence of RPU (renal pelvis ureter) syndrome at oral doses 30 times the human exposure at the recommended daily oral dose of 2.5 mg and ≥9 times the recommended once-monthly oral dose of 150 mg. Impaired pup neuromuscular development (cliff avoidance test) was observed at 45 times human exposure at the daily dose and 13 times the once-monthly dose (see NONCLINICAL TOXICOLOGY [13.2]).
In pregnant rabbits treated orally with ibandronate during gestation at doses ≥8 times the recommended human daily oral dose of 2.5 mg and ≥4 times the recommended human once-monthly oral dose of 150 mg, dose-related maternal mortality was observed in all treatment groups. The deaths occurred prior to parturition and were associated with lung edema and hemorrhage. No significant fetal anomalies were observed (see NONCLINICAL TOXICOLOGY [13.2]).
8.3 Nursing Mothers
It is not known whether BONIVA is excreted in human milk. Because many drugs are excreted in human milk, caution should be exercised when BONIVA is administered to a nursing woman. In lactating rats treated with intravenous doses, ibandronate was present in breast milk from 2 to 24 hours after dose administration. Concentrations in milk averaged 1.5 times plasma concentrations.
8.4 Pediatric Use
Safety and effectiveness in pediatric patients have not been established.
8.5 Geriatric Use
Of the patients receiving BONIVA 2.5 mg daily in postmenopausal osteoporosis studies, 52% were over 65 years of age, and 10% were over 75 years of age. Of the patients receiving BONIVA 150 mg once-monthly in the postmenopausal osteoporosis 1-year study, 52% were over 65 years of age, and 9% were over 75 years of age. No overall differences in effectiveness or safety were observed between these patients and younger patients but greater sensitivity in some older individuals cannot be ruled out.
8.6 Renal Impairment
BONIVA is not recommended for use in patients with severe renal impairment (creatinine clearance <30 mL/min).
10 OVERDOSAGE
No specific information is available on the treatment of overdosage of BONIVA. However, based on knowledge of this class of compounds, oral overdosage may result in hypocalcemia, hypophosphatemia, and upper gastrointestinal adverse events, such as upset stomach, dyspepsia, esophagitis, gastritis, or ulcer. Milk or antacids should be given to bind BONIVA. Due to the risk of esophageal irritation, vomiting should not be induced, and the patient should remain fully upright. Dialysis would not be beneficial.
11 DESCRIPTION
BONIVA (ibandronate sodium) is a nitrogen-containing bisphosphonate that inhibits osteoclast-mediated bone resorption. The chemical name for ibandronate sodium is 3-(N-methyl-N-pentyl) amino-1-hydroxypropane-1,1-diphosphonic acid, monosodium salt, monohydrate with the molecular formula C9H22NO7P2Na•H2O and a molecular weight of 359.24. Ibandronate sodium is a white- to off-white powder. It is freely soluble in water and practically insoluble in organic solvents. Ibandronate sodium has the following structural formula:
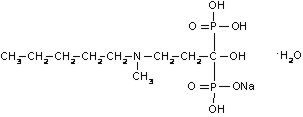
BONIVA is available as a white, oblong, 2.5 mg film-coated tablet for daily oral administration or as a white, oblong, 150 mg film-coated tablet for once-monthly oral administration. One 2.5 mg film-coated tablet contains 2.813 mg ibandronate monosodium monohydrate, equivalent to 2.5 mg free acid. One 150 mg film-coated tablet contains 168.75 mg ibandronate monosodium monohydrate, equivalent to 150 mg free acid. BONIVA also contains the following inactive ingredients: lactose monohydrate, povidone, microcrystalline cellulose, crospovidone, purified stearic acid, colloidal silicon dioxide, and purified water. The tablet film coating contains hypromellose, titanium dioxide, talc, polyethylene glycol 6000, and purified water.
12 CLINICAL PHARMACOLOGY
Enter section text here
12.1 Mechanism of Action
The action of ibandronate on bone tissue is based on its affinity for hydroxyapatite, which is part of the mineral matrix of bone. Ibandronate inhibits osteoclast activity and reduces bone resorption and turnover. In postmenopausal women, it reduces the elevated rate of bone turnover, leading to, on average, a net gain in bone mass.
12.2 Pharmacodynamics
Osteoporosis is characterized by decreased bone mass and increased fracture risk, most commonly at the spine, hip, and wrist. The diagnosis can be confirmed by a finding of low bone mass, evidence of fracture on x-ray, a history of osteoporotic fracture, or height loss or kyphosis indicative of vertebral fracture. While osteoporosis occurs in both men and women, it is most common among women following menopause. In healthy humans, bone formation and resorption are closely linked; old bone is resorbed and replaced by newly formed bone. In postmenopausal osteoporosis, bone resorption exceeds bone formation, leading to bone loss and increased risk of fracture. After menopause, the risk of fractures of the spine and hip increases; approximately 40% of 50-year-old women will experience an osteoporosis-related fracture during their remaining lifetimes.
BONIVA produced biochemical changes indicative of dose-dependent inhibition of bone resorption, including decreases of biochemical markers of bone collagen degradation (such as deoxypyridinoline, and cross-linked C-telopeptide of Type I collagen) in the daily dose range of 0.25 mg to 5 mg and once-monthly doses from 100 mg to 150 mg in postmenopausal women.
Treatment with 2.5 mg daily BONIVA resulted in decreases in biochemical markers of bone turnover, including urinary C-terminal telopeptide of Type I collagen (uCTX) and serum osteocalcin, to levels similar to those in premenopausal women. Changes in markers of bone formation were observed later than changes in resorption markers, as expected, due to the coupled nature of bone resorption and formation. Treatment with 2.5 mg daily BONIVA decreased levels of uCTX within 1 month of starting treatment and decreased levels of osteocalcin within 3 months. Bone turnover markers reached a nadir of approximately 64% below baseline values by 6 months of treatment and remained stable with continued treatment for up to 3 years. Following treatment discontinuation, there is a return to pretreatment baseline rates of elevated bone resorption associated with postmenopausal osteoporosis.
In a 1-year, study comparing once-monthly vs. once-daily oral dosing regimens, the median decrease from baseline in serum CTX values was -76% for patients treated with the 150 mg once-monthly regimen and -67% for patients treated with the 2.5 mg daily regimen. In a 1-year, prevention study comparing BONIVA 150 mg once-monthly to placebo, the median placebo-subtracted decrease in sCTX was -49.8%.
12.3 Pharmacokinetics
Absorption
The absorption of oral ibandronate occurs in the upper gastrointestinal tract. Plasma concentrations increase in a dose-linear manner up to 50 mg oral intake and increases nonlinearly above this dose.
Following oral dosing, the time to maximum observed plasma ibandronate concentrations ranged from 0.5 to 2 hours (median 1 hour) in fasted healthy postmenopausal women. The mean oral bioavailability of 2.5 mg ibandronate was about 0.6% compared to intravenous dosing. The extent of absorption is impaired by food or beverages (other than plain water). The oral bioavailability of ibandronate is reduced by about 90% when BONIVA is administered concomitantly with a standard breakfast in comparison with bioavailability observed in fasted subjects. There is no meaningful reduction in bioavailability when ibandronate is taken at least 60 minutes before a meal. However, both bioavailability and the effect on bone mineral density (BMD) are reduced when food or beverages are taken less than 60 minutes following an ibandronate dose.
Distribution
After absorption, ibandronate either rapidly binds to bone or is excreted into urine. In humans, the apparent terminal volume of distribution is at least 90 L, and the amount of dose removed from the circulation via the bone is estimated to be 40% to 50% of the circulating dose. In vitro protein binding in human serum was 99.5% to 90.9% over an ibandronate concentration range of 2 to 10 ng/mL in one study and approximately 85.7% over a concentration range of 0.5 to 10 ng/mL in another study.
Metabolism
Ibandronate does not undergo hepatic metabolism and does not inhibit the hepatic cytochrome P450 system. Ibandronate is eliminated by renal excretion. Based on a rat study, the ibandronate secretory pathway does not appear to include known acidic or basic transport systems involved in the excretion of other drugs. There is no evidence that ibandronate is metabolized in humans.
Elimination
The portion of ibandronate that is not removed from the circulation via bone absorption is eliminated unchanged by the kidney (approximately 50% to 60% of the absorbed dose). Unabsorbed ibandronate is eliminated unchanged in the feces.
The plasma elimination of ibandronate is multiphasic. Its renal clearance and distribution into bone accounts for a rapid and early decline in plasma concentrations, reaching 10% of the Cmax within 3 or 8 hours after intravenous or oral administration, respectively. This is followed by a slower clearance phase as ibandronate redistributes back into the blood from bone. The observed apparent terminal half-life for ibandronate is generally dependent on the dose studied and on assay sensitivity. The observed apparent terminal half-life for the 150 mg ibandronate tablet upon oral administration to healthy postmenopausal women ranges from 37 to 157 hours.
Total clearance of ibandronate is low, with average values in the range 84 to 160 mL/min. Renal clearance (about 60 mL/min in healthy postmenopausal females) accounts for 50% to 60% of total clearance and is related to creatinine clearance. The difference between the apparent total and renal clearances likely reflects bone uptake of the drug.
Specific Populations
Pediatrics
The pharmacokinetics of ibandronate has not been studied in patients <18 years of age.
Geriatric
Because ibandronate is not known to be metabolized, the only difference in ibandronate elimination for geriatric patients versus younger patients is expected to relate to progressive age-related changes in renal function.
Gender
The bioavailability and pharmacokinetics of ibandronate are similar in both men and women.
Race
Pharmacokinetic differences due to race have not been studied.
Renal Impairment
Renal clearance of ibandronate in patients with various degrees of renal impairment is linearly related to creatinine clearance (CLcr).
Following a single dose of 0.5 mg ibandronate by intravenous administration, patients with CLcr 40 to 70 mL/min had 55% higher exposure (AUC∞) than the exposure observed in subjects with CLcr >90 mL/min. Patients with CLcr <30 mL/min had more than a two-fold increase in exposure compared to the exposure for healthy subjects (see DOSAGE AND ADMINISTRATION [2.4]).
Hepatic Impairment
No studies have been performed to assess the pharmacokinetics of ibandronate in patients with hepatic impairment because ibandronate is not metabolized in the human liver.
Drug Interactions
Products containing calcium and other multivalent cations (such as aluminum, magnesium, iron), including milk, food, and antacids are likely to interfere with absorption of ibandronate, which is consistent with findings in animal studies.
H2 Blockers
A pharmacokinetic interaction study in healthy volunteers demonstrated that 75 mg ranitidine (25 mg injected intravenously 90 and 15 minutes before and 30 minutes after ibandronate administration) increased the oral bioavailability of 10 mg ibandronate by about 20%. This degree of increase is not considered to be clinically relevant.
13 NONCLINICAL TOXICOLOGY
Enter section text here
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
In a 104-week carcinogenicity study, doses of 3, 7, or 15 mg/kg/day were administered by oral gavage to male and female Wistar rats (systemic exposures up to 12 and 7 times, respectively, human exposure at the recommended daily oral dose of 2.5 mg, and cumulative exposures up to 3.5 and 2 times, respectively, human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). There were no significant drug-related tumor findings in male or female rats. In a 78-week carcinogenicity study, doses of 5, 20, or 40 mg/kg/day were administered by oral gavage to male and female NMRI mice (exposures up to 475 and 70 times, respectively, human exposure at the recommended daily oral dose of 2.5 mg and cumulative exposures up to 135 and 20 times, respectively, human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). There were no significant drug-related tumor findings in male or female mice. In a 90-week carcinogenicity study, doses of 5, 20, or 80 mg/kg/day were administered in the drinking water to NMRI mice (cumulative monthly exposures in males and females up to 70 and 115 times, respectively, human exposure at the recommended dose of 150 mg, based on AUC comparison). A dose-related increased incidence of adrenal subcapsular adenoma/carcinoma was observed in female mice, which was statistically significant at 80 mg/kg/day (220 to 400 times human exposure at the recommended daily oral dose of 2.5 mg and 115 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). The relevance of these findings to humans is unknown.
Mutagenesis
There was no evidence for a mutagenic or clastogenic potential of ibandronate in the following assays: in vitro bacterial mutagenesis assay in Salmonella typhimurium and Escherichia coli (Ames test), mammalian cell mutagenesis assay in Chinese hamster V79 cells, and chromosomal aberration test in human peripheral lymphocytes, each with and without metabolic activation. Ibandronate was not genotoxic in the in vivo mouse micronucleus tests for chromosomal damage.
Impairment of Fertility
In female rats treated from 14 days prior to mating through gestation, decreases in fertility, corpora lutea, and implantation sites were observed at an oral dose of 16 mg/kg/day (45 times human exposure at the recommended daily oral dose of 2.5 mg and 13 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison).
13.2 Animal Reproductive and Developmental Toxicology
In female rats given oral doses of 1, 4, or 16 mg/kg/day beginning 14 days before mating and continuing through lactation, maternal deaths were observed at the time of delivery in all dose groups (≥3 times human exposure at the recommended daily oral dose of 2.5 mg or ≥1 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). Perinatal pup loss in dams given 16 mg/kg/day (45 times human exposure at the recommended daily oral dose of 2.5 mg and 13 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison) was likely related to maternal dystocia. In pregnant rats given oral doses of 6, 20, or 60 mg/kg/day during gestation, calcium supplementation (32 mg/kg/day by subcutaneous injection from gestation day 18 to parturition) did not completely prevent dystocia and periparturient mortality in any of the treated groups (≥16 times human exposure at the recommended daily oral dose of 2.5 mg and ≥4.6 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). A low incidence of postimplantation loss was observed in rats treated from 14 days before mating throughout lactation or during gestation, only at doses causing maternal dystocia and periparturient mortality. In pregnant rats dosed orally with 1, 5, or 20 mg/kg/day from gestation day 17 through lactation day 21 (following closure of the hard palate through weaning), maternal toxicity, including dystocia and mortality, fetal perinatal and postnatal mortality, were observed at doses ≥5 mg/kg/day (equivalent to human exposure at the recommended daily oral dose of 2.5 mg and ≥4 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). Periparturient mortality has also been observed with other bisphosphonates and appears to be a class effect related to inhibition of skeletal calcium mobilization resulting in hypocalcemia and dystocia.
Exposure of pregnant rats during the period of organogenesis resulted in an increased fetal incidence of RPU (renal pelvis ureter) syndrome at oral doses ≥10 mg/kg/day (≥30 times human exposure at the recommended daily oral dose of 2.5 mg and ≥9 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison). Impaired pup neuromuscular development (cliff avoidance test) was observed at 16 mg/kg/day when dams were dosed from 14 days before mating through lactation (45 times human exposure at the recommended daily oral dose of 2.5 mg and 13 times human exposure at the recommended once-monthly oral dose of 150 mg, based on AUC comparison).
In pregnant rabbits given oral doses of 1, 4, or 20 mg/kg/day during gestation, dose-related maternal mortality was observed in all treatment groups (≥8 times the recommended human daily oral dose of 2.5 mg and ≥4 times the recommended human once-monthly oral dose of 150 mg, based on body surface area comparison, mg/m2). The deaths occurred prior to parturition and were associated with lung edema and hemorrhage. No significant fetal anomalies were observed.
13.3 Animal Pharmacology
Animal studies have shown that ibandronate is an inhibitor of osteoclast-mediated bone resorption. In the Schenk assay in growing rats, ibandronate inhibited bone resorption and increased bone volume, based on histologic examination of the tibial metaphyses. There was no evidence of impaired mineralization at the highest dose of 5 mg/kg/day (subcutaneously), which is 1000 times the lowest antiresorptive dose of 0.005 mg/kg/day in this model, and 5000 times the optimal antiresorptive dose of 0.001 mg/kg/day in the aged ovariectomized rat. This indicates that BONIVA administered at therapeutic doses is unlikely to induce osteomalacia.
Long-term daily or once-monthly intermittent administration of ibandronate to ovariectomized rats or monkeys was associated with suppression of bone turnover and increases in bone mass. In both rats and monkeys, vertebral BMD, trabecular density, and biomechanical strength were increased dose-dependently at doses up to 15 times the recommended human daily oral dose of 2.5 mg, or cumulative monthly doses up to 8 times (rat) or 6 times (monkey) the recommended human once-monthly oral dose of 150 mg, based on body surface area (mg/m2) or AUC comparison. In monkeys, ibandronate maintained the positive correlation between bone mass and strength at the ulna and femoral neck. New bone formed in the presence of ibandronate had normal histologic structure and did not show mineralization defects.
14 CLINICAL STUDIES
Enter section text here
14.1 Treatment of Postmenopausal Osteoporosis
Daily Dosing
The effectiveness and safety of BONIVA were demonstrated in a randomized, double-blind, placebo-controlled, multinational study (Treatment Study) of 2946 women aged 55 to 80 years, who were on average 21 years postmenopause, who had lumbar spine BMD 2 to 5 SD below the premenopausal mean (T-score) in at least one vertebra [L1-L4], and who had 1 to 4 prevalent vertebral fractures. BONIVA was evaluated at oral doses of 2.5 mg daily and 20 mg intermittently. The main outcome measure was the occurrence of new radiographically diagnosed vertebral fractures after 3 years of treatment. The diagnosis of an incident vertebral fracture was based on both qualitative diagnosis by the radiologist and quantitative morphometric criterion. The morphometric criterion required the dual occurrence of 2 events: a relative height ratio or relative height reduction in a vertebral body of at least 20%, together with at least a 4 mm absolute decrease in height. All women received 400 IU vitamin D and 500 mg calcium supplementation per day.
Effect on Fracture Incidence
BONIVA 2.5 mg daily significantly reduced the incidence of new vertebral (primary efficacy measure) and of new and worsening vertebral fractures. Over the course of the 3-year study, the risk for vertebral fracture was 9.6% in the placebo-treated women and 4.7% in the women treated with BONIVA 2.5 mg (p<0.001) (see Table 3).
|
|
Proportion of Patients with Fracture (%) | |||
|---|---|---|---|---|
|
|
Placebo n=975 |
BONIVA 2.5 mg Daily n=977 |
Absolute Risk Reduction (%) 95% CI |
Relative Risk Reduction (%) 95% CI |
| New Vertebral Fracture | 9.6 | 4.7 | 4.9 | 52 † |
| 0-3 Year |
|
|
(2.3, 7.4) | (29, 68) |
| New and Worsening Vertebral Fracture | 10.4 | 5.1 | 5.3 | 52 |
| 0-3 Year |
|
|
(2.6, 7.9) | (30, 67) |
| Clinical (Symptomatic) Vertebral Fracture | 5.3 | 2.8 | 2.5 | 49 |
| 0-3 Year |
|
|
(0.6, 4.5) | (14, 69) |
BONIVA 2.5 mg daily did not reduce the incidence of nonvertebral fractures (secondary efficacy measure). There was a similar number of nonvertebral osteoporotic fractures at 3 years reported in women treated with BONIVA 2.5 mg daily [9.1%, (95% CI: 7.1%, 11.1%)] and placebo [8.2%, (95% CI: 6.3%, 10.2%)]. The two treatment groups were also similar with regard to the number of fractures reported at the individual nonvertebral sites: pelvis, femur, wrist, forearm, rib, and hip.
Bone Mineral Density (BMD)
BONIVA significantly increased BMD at the lumbar spine and hip relative to treatment with placebo. In the 3-year osteoporosis treatment study, BONIVA 2.5 mg daily produced increases in lumbar spine BMD that were progressive over 3 years of treatment and were statistically significant relative to placebo at 6 months and at all later time points. Lumbar spine BMD increased by 6.4% after 3 years of treatment with 2.5 mg daily BONIVA compared with 1.4% in the placebo group. Table 4 displays the significant increases in BMD seen at the lumbar spine, total hip, femoral neck, and trochanter compared to placebo. Thus, overall BONIVA reverses the loss of BMD, a central factor in the progression of osteoporosis.
|
|
Placebo | BONIVA 2.5 mg Daily |
|---|---|---|
| Lumbar Spine | 1.4 (n=693) |
6.4 (n=712) |
| Total Hip | -0.7 (n=638) |
3.1 (n=654) |
| Femoral Neck | -0.7 (n=683) |
2.6 (n=699) |
| Trochanter | 0.2 (n=683) |
5.3 (n=699) |
Bone Histology
The effects of BONIVA 2.5 mg daily on bone histology were evaluated in iliac crest biopsies from 16 women after 22 months of treatment and 20 women after 34 months of treatment.
The histological analysis of bone biopsies showed bone of normal quality and no indication of osteomalacia or a mineralization defect.
Once-Monthly Dosing
The effectiveness and safety of BONIVA once-monthly were demonstrated in a randomized, double-blind, multinational, noninferiority trial in 1602 women aged 54 to 81 years, who were on average 18 years postmenopause, and had L2-L4 lumbar spine BMD T-score below -2.5 SD at baseline. The main outcome measure was the comparison of the percentage change from baseline in lumbar spine BMD after 1 year of treatment with once-monthly ibandronate (100 mg, 150 mg) to daily ibandronate (2.5 mg). All patients received 400 IU vitamin D and 500 mg calcium supplementation per day.
BONIVA 150 mg once-monthly (n=327) was shown to be noninferior to BONIVA 2.5 mg daily (n=318) in lumbar spine BMD in a 1-year, double-blind, multicenter study of women with postmenopausal osteoporosis. In the primary efficacy analysis (per-protocol population), the mean increases from baseline in lumbar spine BMD at 1 year were 3.86% (95% CI: 3.40%, 4.32%) in the 2.5 mg daily group and 4.85% (95% CI: 4.41%, 5.29%) in the 150 mg once-monthly group; the mean difference between 2.5 mg daily and 150 mg once-monthly was 0.99% (95% CI: 0.38%, 1.60%), which was statistically significant (p=0.002). The results of the intent-to-treat analysis were consistent with the primary efficacy analysis. The 150 mg once-monthly group also had consistently higher BMD increases at the other skeletal sites compared to the 2.5 mg daily group.
14.2 Prevention of Postmenopausal Osteoporosis
Daily Dosing
The safety and effectiveness of BONIVA 2.5 mg daily for the prevention of postmenopausal osteoporosis were demonstrated in a randomized, double-blind, placebo-controlled 2-year study (Prevention Study) of 653 postmenopausal women without osteoporosis at baseline. Women were aged 41 to 82 years, were on average 8.5 years postmenopause, and had lumbar spine BMD T-scores >-2.5. Women were stratified according to time since menopause (1 to 3 years, >3 years) and baseline lumbar spine BMD (T-score: >-1, -1 to -2.5). The study compared daily BONIVA at three dose levels (0.5 mg, 1.0 mg, 2.5 mg) with placebo. All women received 500 mg of supplemental calcium per day.
The primary efficacy measure was the change in BMD of lumbar spine after 2 years of treatment. BONIVA 2.5 mg daily resulted in a mean increase in lumbar spine BMD of 3.1% compared with placebo following 2 years of treatment. Increases in BMD were seen at 6 months and at all later time points. Irrespective of the time since menopause or the degree of pre-existing bone loss, treatment with BONIVA resulted in a higher BMD response at the lumbar spine compared with placebo across all four baseline strata [time since menopause (1 to 3 years, >3 years) and baseline lumbar spine BMD (T-score: >-1, -1 to -2.5)].
Compared with placebo, treatment with BONIVA 2.5 mg daily increased BMD of the total hip by 1.8%, the femoral neck by 2.0%, and the trochanter by 2.1%.
Once-Monthly Dosing
BONIVA 150 mg once-monthly prevented bone loss in a majority (88.2%) of women in a randomized, double-blind, placebo-controlled 1-year study (Monthly Prevention Study) of 160 postmenopausal women with low bone mass at baseline (T-score of -1 to -2.5). Women, aged 46 to 60 years, were on average 5.4 years postmenopause. All women received 400 IU of vitamin D and 500 mg calcium supplementation daily.
The primary efficacy measure was the relative change in BMD at the lumbar spine after 1 year of treatment. BONIVA 150 mg once-monthly resulted in a mean increase in lumbar spine BMD of 4.12% (95% confidence interval 2.96 – 5.28) compared with placebo following 1 year of treatment (p<0.0001), based on a 3.73% and -0.39% mean change in BMD from baseline in the 150 mg once-monthly BONIVA and placebo treatment groups, respectively. BMD at other skeletal sites was also increased relative to baseline values.
16 HOW SUPPLIED/STORAGE AND HANDLING
Enter section text here
16.1 How Supplied
BONIVA 150 mg tablets: supplied as white, oblong, film-coated tablets, engraved with "BNVA" on one side and "150" on the other side. Packaged in
| 3 blister packs of 1 tablet each |
NDC 54868-5322-0 |
| 1 blister pack of 1 tablet each |
NDC 54868-5322-1 |
16.2 Storage and Handling
Store at 25°C (77°F); excursions permitted between 15° and 30°C (59° and 86°F) [see USP Controlled Room Temperature].
17 PATIENT COUNSELING INFORMATION
See FDA-APPROVED PATIENT LABELING (17.2)
17.1 Information for Patients
Patients should be instructed to read the Patient Information Leaflet carefully before taking BONIVA, to re-read it each time the prescription is renewed and to pay particular attention to the dosing instructions in order to maximize absorption and clinical benefit.
- BONIVA should be taken at least 60 minutes before the first food or drink (other than water) of the day and before taking any oral medication or supplementation including calcium, antacids or vitamins (see DRUG INTERACTIONS [7.1]).
- To facilitate delivery to the stomach, and thus reduce the potential for esophageal irritation, BONIVA tablets should be swallowed whole with a full glass of plain water (6 to 8 oz) while the patient is standing or sitting in an upright position. Patients should not lie down for 60 minutes after taking BONIVA.
- Patients should not eat, drink anything except for water, or take other medications for 60 minutes after taking BONIVA.
- Plain water is the only drink that should be taken with BONIVA. Note that some mineral waters may have a higher concentration of calcium and therefore should not be used.
- Patients should not chew or suck the tablet because of a potential for oropharyngeal ulceration.
- The BONIVA 2.5 mg tablet should be taken at the same time each day.
- If a once-daily dose is missed, the patient should be instructed to skip that dose and return to their normal schedule the next day.
- The patient must not take two 2.5 mg tablets within the same day.
- The BONIVA 150 mg tablet should be taken on the same date each month (i.e., the patient's BONIVA day).
- The patient must not take two 150 mg tablets within the same week.
- If the once-monthly dose is missed, and the patient's next scheduled BONIVA day is more than 7 days away, the patient should be instructed to take one BONIVA 150 mg tablet in the morning following the date that it is remembered (see DOSAGE AND ADMINISTRATION [2.3]). The patient should then return to taking one BONIVA 150 mg tablet every month in the morning of their chosen day, according to their original schedule.
- If the once-monthly dose is missed, and the patient's next scheduled BONIVA day is only 1 to 7 days away, the patient must wait until the subsequent month's scheduled BONIVA day to take their tablet. The patient should then return to taking one BONIVA 150 mg tablet every month in the morning of their chosen day, according to their original schedule.
Patients should receive supplemental calcium and vitamin D if dietary intake is inadequate. Intake of supplemental calcium and vitamin D should be delayed for at least 60 minutes following oral administration of BONIVA in order to maximize absorption of BONIVA.
Physicians should be alert to signs or symptoms signaling a possible esophageal reaction during therapy, and patients should be instructed to discontinue BONIVA and seek medical attention if they develop symptoms of esophageal irritation such as new or worsening dysphagia, pain on swallowing, retrosternal pain, or heartburn.
17.2 FDA-Approved Patient Labeling
Read this patient information carefully before you start taking BONIVA. Read this patient information each time you get a refill for BONIVA. There may be new information. This information is not everything you need to know about BONIVA. It does not take the place of talking with your health care provider about your condition or your treatment. Talk about BONIVA with your health care provider before you start taking it, and at your regular check-ups.
What is the most important information I should know about BONIVA?
BONIVA may cause serious problems in the stomach and the esophagus (the tube that connects your mouth and stomach) such as trouble swallowing, heartburn, and ulcers (see "What are the possible side effects of BONIVA?").
You must take BONIVA exactly as prescribed for BONIVA to work for you and to lower the chance of serious side effects (see "How should I take BONIVA?").
What is BONIVA?
BONIVA is a prescription medicine used to treat or prevent osteoporosis in women after menopause (see the end of this leaflet for "What is osteoporosis?").
BONIVA may reverse bone loss by stopping more loss of bone and increasing bone mass in most women who take it, even though they won't be able to see or feel a difference. BONIVA may help lower the chances of breaking bones (fractures).
For BONIVA to treat or prevent osteoporosis, you have to take it as prescribed. BONIVA will not work if you stop taking it.
Who should not take BONIVA?
Do not take BONIVA if you:
- have certain problems with your esophagus, the tube that connects your mouth and stomach
- cannot sit or stand up for at least 60 minutes
- have low blood calcium (hypocalcemia)
- are allergic to ibandronate sodium or any of the other ingredients of BONIVA (see the end of this leaflet for a list of all the ingredients in BONIVA)
- have kidneys that work very poorly
Tell your health care provider before using BONIVA:
- if you are pregnant or planning to become pregnant. It is not known if BONIVA can harm your unborn baby.
- if you are breast-feeding. It is not known if BONIVA passes into your milk and if it can harm your baby.
- have swallowing problems or other problems with your esophagus (the tube that connects your mouth and stomach)
- if you have kidney problems
- if you are planning a dental procedure such as tooth extraction
Tell your health care provider (including your dentist) about all the medicines you take including prescription and non-prescription medicines, vitamins and supplements. Some medicines, especially certain vitamins, supplements, and antacids can stop BONIVA from getting to your bones. This can happen if you take other medicines too close to the time that you take BONIVA (see "How should I take BONIVA?").
How should I take BONIVA?
- Take BONIVA exactly as instructed by your health care provider.
- Take BONIVA first thing in the morning at least 60 minutes before you eat, drink anything other than plain water, or take any other oral medicine.
- Take BONIVA with 6 to 8 ounces (about 1 full cup) of plain water. Do not take it with any drink other than plain water. Do not take it with other drinks, such as mineral water, sparkling water, coffee, tea, dairy drinks (such as milk), or juice.
- Swallow BONIVA whole. Do not chew or suck the tablet or keep it in your mouth to melt or dissolve.
- After taking BONIVA you must wait at least 60 minutes before: –Lying down. You may sit, stand, or do normal activities like read the newspaper or take a walk.–Eating or drinking anything except for plain water.–Taking other oral medicines including vitamins, calcium, or antacids. Take your vitamins, calcium, and antacids at a different time of the day from the time when you take BONIVA.
- If you take too much BONIVA, drink a full glass of milk and call your local poison control center or emergency room right away. Do not make yourself vomit. Do not lie down.
- Keep taking BONIVA for as long as your health care provider tells you. BONIVA will not work if you stop taking it.
- Your health care provider may tell you to exercise and take calcium and vitamin supplements to help your osteoporosis.
- Your health care provider may do a test to measure the thickness (density) of your bones or do other tests to check your progress.
What is my BONIVA schedule?
Schedule for taking BONIVA 2.5 mg once-daily:
- Take one BONIVA 2.5 mg tablet once a day first thing in the morning at least 60 minutes before you eat, drink anything other than plain water, or take any other oral medicine (see "How should I take BONIVA?").
What to do if I miss a daily dose:
- If you forget to take your BONIVA 2.5 mg tablet in the morning, do not take it later in the day. Just return to your normal schedule and take 1 tablet the next morning. Do not take two tablets on the same day.
- If you are not sure what to do if you miss a dose, contact your health care provider who will be able to advise you.
Schedule for taking BONIVA 150 mg once-monthly:
- Take one BONIVA 150 mg tablet once a month.
- Choose one date of the month (your BONIVA day) that you will remember and that best fits your schedule to take your BONIVA 150 mg tablet.
- Take one BONIVA 150 mg tablet in the morning of your chosen day (see "How should I take BONIVA?").
What to do if I miss a monthly dose:
- If your next scheduled BONIVA day is more than 7 days away, take one BONIVA 150 mg tablet in the morning following the day that you remember (see "How should I take BONIVA?"). Then return to taking one BONIVA 150 mg tablet every month in the morning of your chosen day, according to your original schedule.
- Do not take two 150 mg tablets within the same week. If your next scheduled BONIVA day is only 1 to 7 days away, wait until your next scheduled BONIVA day to take your tablet. Then return to taking one BONIVA 150 mg tablet every month in the morning of your chosen day, according to your original schedule.
- If you are not sure what to do if you miss a dose, contact your health care provider who will be able to advise you.
What should I avoid while taking BONIVA?
- Do not take other medicines, or eat or drink anything but plain water before you take BONIVA and for at least 60 minutes after you take it.
- Do not lie down for at least 60 minutes after you take BONIVA.
What are the possible side effects of BONIVA?
Stop taking BONIVA and call your health care provider right away if you have:
- pain or trouble with swallowing
- chest pain
- very bad heartburn or heartburn that does not get better
BONIVA MAY CAUSE:
- pain or trouble swallowing (dysphagia)
- heartburn (esophagitis)
- ulcers in your stomach or esophagus (the tube that connects your mouth and stomach)
Common side effects with BONIVA are:
- diarrhea
- pain in extremities (arms or legs)
- dyspepsia (upset stomach)
Less common side effects with BONIVA are short-lasting, mild flu-like symptoms (which usually improve after the first dose). These are not all the possible side effects of BONIVA. For more information ask your health care provider or pharmacist.
Rarely, patients have reported allergic and skin reactions. Contact your health care provider if you develop any symptoms of an allergic reaction including skin rash (with or without blisters), hives, wheezing, or swelling of the face, lips, tongue or throat. Get medical help right away if you have trouble breathing, swallowing or feel light-headed.
Rarely, patients have reported severe bone, joint, and/or muscle pain starting within one day to several months after beginning to take, by mouth, bisphosphonate drugs to treat osteoporosis (thin bones). This group of drugs includes BONIVA. Most patients experienced relief after stopping the drug. Contact your health care provider if you develop these symptoms after starting BONIVA.
Rarely, patients taking bisphosphonates have reported serious jaw problems associated with delayed healing and infection, often following dental procedures such as tooth extraction. If you experience jaw problems, contact your health care provider and dentist.
What is osteoporosis?
Osteoporosis is a disease that causes bones to become thinner. Thin bones can break easily. Most people think of their bones as being solid like a rock. Actually, bone is living tissue, just like other parts of the body, such as your heart, brain, or skin. Bone just happens to be a harder type of tissue. Bone is always changing. Your body keeps your bones strong and healthy by replacing old bone with new bone.
Osteoporosis causes the body to remove more bone than it replaces. This means that bones get weaker. Weak bones are more likely to break. Osteoporosis is a bone disease that is quite common in women after menopause. At first, osteoporosis has no symptoms, but people with osteoporosis may develop loss of height and are more likely to break (fracture) their bones, especially the back (spine), wrist, and hip bones.
Osteoporosis can be prevented, and with proper therapy it can be treated.
Who is at risk for osteoporosis?
Talk to your health care provider about your chances for getting osteoporosis.
Many things put people at risk for osteoporosis. The following people have a higher chance of getting osteoporosis:
Women who:
- are going through or who are past menopause ("the change")
- are white (Caucasian) or Asian
People who:
- are thin
- have a family member with osteoporosis
- do not get enough calcium or vitamin D
- do not exercise
- smoke
- drink alcohol often
- take bone thinning medicines (like prednisone) for a long time
General information about BONIVA
Do not use BONIVA for a condition for which it was not prescribed. Do not give BONIVA to other people, even if they have the same symptoms you have. It may harm them.
Store BONIVA at 77°F (25°C) or at room temperature between 59°F and 86°F (15°C and 30°C).
Keep BONIVA and all medicines out of the reach of children.
This summarizes the most important information about BONIVA. If you would like more information, talk with your health care provider. You can ask your health care provider or pharmacist for information about BONIVA that is written for health professionals.
For more information about BONIVA, call 1-888-MY-BONIVA or visit www.myboniva.com.
What are the ingredients of BONIVA?
BONIVA (active ingredient): ibandronate sodium
BONIVA (inactive ingredients): lactose monohydrate, povidone, microcrystalline cellulose, crospovidone, purified stearic acid, colloidal silicon dioxide, and purified water. The tablet film coating contains hypromellose, titanium dioxide, talc, polyethylene glycol 6000 and purified water.
BONIVA is a registered trademark of Roche Therapeutics Inc.
Distributed by:
Genentech USA, Inc.
A Member
of the Roche Group
1 DNA Way
South San Francisco, CA 94080-4990
BAT_2005450_PI_AR2010_K(1)
Revised: January 2010
© 2010 Genentech, Inc. All rights reserved.
(see the HOW SUPPLIED section for complete
listing)
Relabeling of "Additional Barcode Label" by:
Physicians Total Care, Inc.
Tulsa, OK 74146
PRINCIPAL DISPLAY PANEL - 3 Pack Carton
once-monthly
Boniva®
(ibandronate sodium) Tablets
One tablet contains 168.75 mg ibandronate monosodium
monohydrate,
equivalent to 150 mg free acid.
USUAL DOSAGE: For dosage recommendations and other
important
prescribing information, read accompanying insert.
PHARMACIST: Dispense with important patient information.
150 mg
3 Packs–One Tablet Per Pack
Rx only

Bonivaibandronate sodium TABLET, FILM COATED
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||